Clinics in Family
Practice
Volume 2 • Number 3 • September 2000
Copyright © 2000 W. B. Saunders Company
|
|
|
|
|
|
OFFICE MANAGEMENT OF TRAUMA
MANAGEMENT OF ACUTE FRACTURES AROUND THE KNEE, ANKLE, AND
FOOT
Phillip M. Steele MD
Charles Bush-Joseph MD
Bernard Bach Jr. MD
Department of Family Practice, MacNeal
Hospital, Berwyn, Illinois; and Department of Orthopaedic Surgery, Rush Medical
College, Chicago, Illinois
Address reprint requests to
Phillip M. Steele, MD
Gem City Bone and Joint
1909 Vista Drive
Laramie, WY 82070
Primary care physicians commonly see fractures to the lower
extremity. Isolated injuries to the metatarsals and phalanxes account for up to
15% of all fractures presenting to emergency departments. Ankle injuries,
including sprains and fractures, account for 10% of all radiographs ordered in
an emergency room setting. With the advent of improved orthotic bracing and of
surgical and nonsurgical techniques, the management of lower extremity
fractures is evolving. This article reviews current concepts in the evaluation
and management of these injuries. Indications for radiographic evaluation and
treatment with splinting or casting are also reviewed.
ACUTE CARE
Acute care of the injured patient includes initial triage of the
unstable patient, identification of musculoskeletal injuries, and provisional
splinting of injured extremities. Initial evaluation requires evaluation for
closed head, cervical spine, intrathoracic, and intra-abdominal injuries.
Checking vital signs, symptoms of shock, and potential risks of bleeding should
be done immediately. Examination for the presence of gross deformity, loss of
pulses, or impaired neurologic function distal to the injury should also be
included in the initial evaluation. Provisional splinting of injured
extremities and sterile dressing of open wounds will ease the patient's
discomfort and allow a more detailed examination. A warm blanket for the torso
and a supine position will increase the patient's comfort and decrease the risk
for shock. Comfort care includes minimizing patient transfers and early
administration of analgesia, because radiologic positioning can be very
painful.
High-energy trauma, including motor vehicle injuries, falls from
height, or injuries with possible spine or pelvic fractures, have a greater
potential for internal bleeding. If a high-energy hip or pelvic fracture is
suspected, large-bore intravenous access may be necessary to control shock.
A padded fiberglass posterior or stirrup splint can be used for
lower leg injuries.[22] An elastic bandage or tape measure can
be used to determine the length of splint needed. For correct width sizing, a
4- or 5-inch rolled elastic bandage can be used to estimate the splint width
size that provides the best fit. The choice of precut or rolled splinting
material is a matter of preference, because each has its own merits. Using cool water will lengthen the setting time.
Avoiding oversaturation of the splint makes molding the splint more comfortable
for the patient and improves fit.[23] For stability, an assistant should hold
the extremity above and below the fracture site while an elastic bandage is
rolled with light tension and a 50% overlap. A 3-inch elastic bandage is best
for the ankle and foot area. Wrapping the tibia and fibula area with a 4-inch
wrap while smoothing the cast padding will also improve comfort. The toes
should be left exposed to check for circulation. The patient should be
instructed to check the FACTS: Function,
Arterial pulses, Capillary refill, Temperature of the skin, and Sensation. Rest, Ice, Compression and Elevation (RICE) instructions and the proper use of crutches
should be reviewed with the patient. The patient should be given clear
instructions on recognizing the symptoms of compartment syndrome and when to
call with questions or concerns that develop before the next scheduled visit.
For patients with fractures requiring urgent or possible surgical
management, an additional history of last meal, medical problems, and
medications should be sought. Patients should take nothing by mouth until
surgical consultation has established a definitive treatment.
OPEN FRACTURES
Although definitive treatment of closed fractures should be
considered urgent, all open fractures should be treated as a true medical
emergency to minimize the risk of infection. An open fracture is a fracture
that communicates with an open wound. Skin abrasions or simple lacerations not
communicating with the fracture hematoma are not considered open fractures and
are treated as closed injuries.
Although open fractures should ideally be graded under operative
conditions to minimize the risk for infection,[1] [26] [28] communicating the type of open fracture
can help the surgical consultant assess the urgency of the situation. The most
common classification system for open fractures divides open fractures into
three main types based on the mechanism of injury, the vascular status of the
extremity, the extent of soft-tissue damage, the amount of comminution and bone
loss, and the degree of bacterial contamination. Type I fractures are
low-energy injuries with minimal soft-tissue damage and a surface wound smaller
than 1 cm. This type of open wound is created from an inside-to-outside
puncture from the underlying bone. A type II fracture occurs with moderate
energy forces and causes an associated soft-tissue laceration of less than 10
cm. The most severe open fracture pattern is type III, which results from
highenergy forces causing extensive soft-tissue damage. Extensive comminution
or a segmental fracture pattern generally occurs with this type of fracture,
and bacterial contamination is often suspected.[1] [28]
Medical management of open fractures should be oriented at
preventing additional contamination by rapid transport and by minimizing
dressing changes and the number of persons inspecting the wound outside the
operating room. The wound should be covered with moist sterile bandaging, and
the extremity should be splinted in place.
Acute management should not
include routine wound cultures in the emergency department, because
in patients who have undergone repeated dressing changes and cultures taken
before surgery the risk of infection increases from 4.3% to 19.2%.[1] [26] Initial cultures are generally not
effective in predicting sepsis. Early intravenous administration of antibiotic
should be routine for all open fractures. Antibiotic coverage for a type I open
fracture should be oriented towards gram-positive organisms, using cefazolin.
Combination therapy using an aminoglycoside for gram-negative coverage plus
cefazolin should be used for type II and III open fractures.[1] [26] [28] If Clostridium
perfringens contamination is suspected (e.g., from soil near
farmlands), penicillin coverage should be added.[26] If surgical delay is anticipated,
intravenous antibiotics should be started in the Emergency Department.
The speed and urgency of transportation to the hospital has a
great effect on prognosis. Helicopter transfer is associated with an infection
rate of about 3%, whereas the rate of infection following ground transport is
12%.[26] Primary care management should include
transport coordination to optimize patient prognosis.
COMPARTMENT SYNDROME
Although compartment syndrome (CS) may occur after any fracture,
it is more commonly associated with long-bone fractures. Compartment syndrome
is associated with about 20% of tibial fractures.[1] [26] [28] The force required to fracture long
bones causes extensive muscular contusion, swelling, and hemorrhage. With early
cast immobilization, muscle expansion is limited, increasing the risks for CS.
As fascial compartment pressure increases, it may exceed capillary blood pressures
to the involved area. Although arterial pressure may be sufficient for distal
pulses, capillary flow is diminished, and muscular ischemia may occur. The
finding of diminished or absent pulses is a late clinical sign of CS, and
intervention should have already occurred. Clinical signs of CS include
increasing, disproportionate pain after casting or splinting and pain incurred
with passive motion of the involved compartment.[28] After the first 24 hours, there may also
be tenderness over the involved compartment, as well as at the site of the
fracture, and weakness of the musculature of the compartment involved (Table
1) . Immediate removal of constricting or circumferential dressings or
splints is the first intervention with suspected CS. Orthopedic referral is
indicated if symptoms are not promptly relieved with splint and dressing
removal. Evaluation and management include compartment pressure measurement and
surgical fasciotomies for pressures above 30 mm Hg.
|
TABLE 1 -- Physical Examination Findings for
Anterior and Posterior Compartment Syndrome |
|
|
Involved Compartment |
Symptoms |
|
Anterior Compartment |
Decreased
sensation 1st web space, weakness of toe extension, pain with passive
toe flexion |
|
Posterior Compartment |
Decreased
sensation over sole of foot, pain with passive toe extension, weakness of toe
flexion |
FOLLOW-UP
Patients with a suspected or confirmed fracture should be
re-examined in 2 to 5 days. Repeat radiographs are recommended for injuries
with a high index of suspicion based on history and physical examination but an
initially negative radiographic study. Nondisplaced stable fractures usually do
not require re-imaging at the first follow-up appointment. For injuries that
require casting as a definitive treatment, evolving or resolving swelling may
interfere with adequate immobilization, and casting may require delay or
recasting to ensure proper fit. Lowerextremity fractures involving the tibia
above the level of the malleolus often require surgical management or the use
of a long leg cast and should be referred to a specialist.
As a general rule, the more complicated the fracture, the more
frequent the follow-up. Less compliant patients should also be seen more
frequently. Fractures with a poor blood supply may require radiographs every 2
weeks, whereas stable, nondisplaced fractures can be evaluated radiographically
for healing at 4 to 6 weeks.[11] [28] [32] [35]
Two weeks after casting, follow-up either by telephone or office
visit is advisable to check cast comfort, compliance, and pain. Most fractures
heal in 6 to 8 weeks but vary depending on location, type, blood supply, and
the age of the patient.[11] [28] Once radiographic evidence of fracture
healing has occurred and there is no tenderness over the fracture site, the
cast can be safely discontinued. The patient can be referred to physical or
home therapy for a strengthening and range-of-motion program, depending on age,
motivation, and joint involvement.
EVIDENCE-BASED DIAGNOSTIC TESTING
To discourage the indiscriminate use of radiographs, Brand et al
in 1980 developed a protocol for selecting patients with injuries who need
radiographic examination (Table
2). [6] Studying 848 patients, they found that
strict adherence to the protocol would have decreased unnecessary radiographic
procedures by 12% in upper-extremity injuries and by 19% in lower-extremity
injuries. By eliminating unnecessary radiographic procedures, they concluded
that $79 to $139 million annually could be saved nationwide. Since this
pioneering study, the use of radiographs to assess ankle, knee, nursemaid's
elbow, and shoulder injuries and for pediatric comparison views has been
extensively reviewed. Clinical decision rules (CDRs) for determining the need
for radiologic evaluation exist at many institutions and should be familiar to
primary care providers. In this article, the specific CDRs for each joint are
discussed with each specific joint fracture.
|
TABLE 2 -- Evolution of the Ottawa Ankle
Rules |
|
|
Original Ottawa Ankle
Rules |
Refined Ankle/Foot Rules |
|
Age > 55 |
No
age limits |
|
Unable to bear weight (4 steps) both
immediately and in emergency department |
Inability
to bear weight (4 steps) both immediately and in the emergency department |
|
Bone tenderness (at the posterior edge
or top of either malleolus) |
Bone
tenderness (at the posterior edge or top of either malleolus) |
|
Bone tenderness of the navicular, the
cuboid, base of the fifth metatarsal |
Bone
tenderness at the navicular or the base of the fifth metatarsal |
|
Pain in the midfoot |
Pain
in the midfoot |
In a recent meta-analysis by Kaufman et al, CDRs were evaluated
based on study type, power, sensitivity, specificity, and validity.[17] The goal was to determine whether CDRs
have been reliably developed and validated for plain radiography of extremity
trauma. They found that the existing literature supports the use of CDRs to
evaluate isolated blunt trauma in healthy adults and that CDRs are designed to
detect common fractures. They also found that patient education and follow-up
care are essential, because patients who were not radiologically assessed could
have an insignificant avulsion fracture. Furthermore, patients who are sent
home without a diagnosis and treated as having "no significant
fracture" must understand that they could have a significant ligament
injury, a rare fracture, or an occult fracture. Because CDRs have not
demonstrated 100% sensitivity, the obvious risk of using CDRs is that some
nonsignificant fractures may be missed.
FRACTURES AROUND THE KNEE
The need for selective radiographic evaluation of ankle injuries
has been well described with the Ottawa Ankle Rules (OAR). Guidelines for the
use of knee radiography have not met with widespread acceptance.[25] [31] [36] To establish guidelines that can be
considered the Ottawa Knee Rules, Stiell et al evaluated 1047 adults with acute
knee injuries.[25] [31] [36] They evaluated decision rules including
(1) patient age of 55 years and older, (2) tenderness at the head of the
fibula, (3) isolated tenderness of the patella, (4) inability to flex to 90°,
and (5) inability to bear weight for four steps, both immediately and in the
emergency department. The presence of one or more of these findings was found
to have a 100% sensitivity and a 54% specificity.
Application of these decision rules reduced radiography of acute
knee injuries from 68.6% to 49.4% and reduced time in the emergency room by an
average of 39 minutes.[25] [31] Although decision rules were developed
for emergency department management, application of these decision rules in
primary care may prove to be equally beneficial.[31]
Imaging
Assessment of acute knee injuries should begin with
anterior-posterior (AP) and lateral views. If tenderness of the patella exists,
a sunrise or merchant view should be included.[30] For patients who are unable to bear
weight and in whom a plateau injury is suspected, oblique views or a plateau
view should be added to the routine knee series. If a tibial spine fracture is
suspected with an anterior cruciate ligament injury, a notch or tunnel view can
help visualize this area. Radiographically detected defects in the knee include
the ABCs:
Alignment
(varus or valgus joint space narrowing, rotational defects of the femoral
condyle and shaft, patella alta, or patella baja [the normal length of the
patella ligament is equal to the patella length ±20%; Bone (cortical
defects and defects of the tibial plateau structure); and Cartilaginous
(flattening of the condyles, reactive sclerosis, or a radiolucent defect may
represent an osteochondral defect). Soft-tissue swelling and a hemarthrosis
should increase the suspicion for a fracture.[14] [30]
DISTAL FEMUR FRACTURES
Distal femur fractures are uncommon fractures that generally
result from high-velocity trauma involving direct forces, such as
hyperabduction or adduction, hyperextension, and axial loading. Significant
knee pain and notable hemarthrosis or swelling and deformity are frequently
present. External rotation and shortening of the thigh should increase
suspicion of a displaced supracondylar fracture, because the quadriceps muscle
will pull the proximal fragment forward while the gastrocnemius causes
posterior displacement of the distal fragment.[1] [28] The considerable force necessary to
fracture the femur causes extensive muscular contusion to the quadriceps and
increases the risk for compartment syndrome. This extensive soft-tissue injury
makes fracture management, pain control, and rehabilitation more difficult, and
the extent of the injury should be included in the decision process for
nonoperative or operative management.
Imaging
Anterior-posterior and lateral radiographs of the distal femur are
usually sufficient to demonstrate most fractures. However, an AP pelvis and AP
and lateral hip radiographs should be included, because ipsilateral hip
fracture, dislocation, and multiple fractures are common with high-energy
trauma.[14] [30]
Acute Care
The proximity of the femoral artery to the popliteal fossa
necessitates an accurate assessment of distal pulses and palpation for a
possible pulsitile hematoma in the popliteal fossa. Any suspicion of vascular
compromise should be further evaluated with Doppler ultrasound imaging. Emergent
consultation with vascular or orthopedic surgeons is imperative when vascular
compromise exists. Injury to the peroneal and deep peroneal nerves can occur
with fractures to the distal femur; sensory integrity can be assessed at the
interspace between the first and second toe. Muscular testing is usually
difficult because of pain during the acute management of distal femoral
fractures. Adequate analgesia can contribute to the effectiveness of initial
assessment of these injuries.[1] [28]
Classification
In adults, distal femur fractures are divided into three main
types (Fig.
1) . Supracondylar fractures include fractures found in the area just above
the femoral condyles (metaphysis) to the junction of the femoral shaft
(diaphysis). These fractures are extra-articular and are not associated with a
hemarthrosis. Intra-articular fractures consist of intercondylar and condylar fractures.
They are associated with significant hemarthrosis and should be suspected in
any patient presenting with a history of trauma and intra-articular swelling.
Isolated condylar fractures are uncommon and can be associated with knee
dislocation and muscular or ligamentous attachment avulsion.[2] [14] [28] [30]
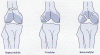 Figure 1. Types of distal femur fractures.
Figure 1. Types of distal femur fractures.
No universal classification system has been accepted, because
surgical management of distal femoral fractures is very individualized. The
evaluation of each fracture should be based on displacement, comminution,
associated soft-tissue injury, neurovascular status, osteoporosis, joint
involvement, and functional status. The fracture should be described as either
displaced or nondisplaced, and involvement of one or both condyles, extension
into the metaphysis or diaphysis, and neurovascular status should be noted.
Care must be taken to confirm whether the fracture is open or closed, because
open fractures require urgent irrigation and debridement.[2] [14] [28] [30]
Treatment
Complications for distal femur fractures include deep vein
thrombosis, fat embolism, delayed union or malunion, valgus or varus angulation
deformities, chronic arthritis, compartment syndrome, and growth disturbances
in adolescents. Orthopedic management is generally required except for simple
nondisplaced fractures.[21] [65] Prompt early referral is important,
because definitive treatment of these fractures varies depending on type of
fracture. Alignment of the femoral condyles must be precise, and any
abnormalities will disrupt joint mechanics and increase wear of the
cartilaginous surfaces. Current strategies include cast-bracing immobilization
or open reduction with internal fixation (ORIF).[65] [68] Medical management involves prevention
of shock, immobilization, and pain control. Neurovascular deficits should
prompt urgent referral to a vascular surgeon or orthopedist.
PATELLAR FRACTURES
As the largest sesamoid bone, the patella has an important
biomechanical role in knee extension by increasing the length of lever arm. The
principal quadriceps insertion site is the superior edge of the patella. The
inferior edge acts as the site of attachment for the patellar tendon.
Contraction of the quadriceps muscle transmits force through the patella to the
patellar tendon and tibial tuberosity. Because cosiderable forces can be
transmitted across the knee during running and jumping, fractures of the
patella are common.[2] [14] [28] [30]
Two main types of patellar fractures are caused by indirect and
direct trauma. Indirect trauma is the most frequent cause of patellar fracture
and occurs during unexpected, rapid, forceful flexion of the knee against a
fully contracted quadriceps. Horizontal or transverse fractures are the most
common fractures caused by indirect trauma. Fractures from direct trauma occur
as a result of a direct blow or a fall onto the knee. Generally, direct trauma
causes considerable comminution, because little soft tissue is present to
buffer the blow. Because many fractures result from a combination of indirect
and direct forces (it is difficult to remain completely relaxed while falling),
many fractures present multiple patterns.[2] [14] [28] [30]
During the physical examination assessing patellar injury, it is
essential to check the ability to extend the knee completely against gravity.
Loss of knee extension may signify disruption of the quadriceps mechanism,
necessitating emergent referral.[2] [9] When the physical examination is limited
because of pain, aspiration of a hemarthrosis and instillation of a local
anesthetic may assist in determining the integrity of the quadriceps tendon.
The patient will generally complain of pain localized to the patella area and
exhibit notable prepatellar swelling. Joint hemarthrosis is frequently present,
and a defect or crepitus may be noted on palpitation of the quadriceps and
patella tendon.[2] [9]
Classification
The classification system for patellar fractures is based on
fracture descriptions, not on prognosis. They are classified as vertical,
transverse, marginal, comminuted (stellate), or osteochondral (Fig.
2) . Transverse fractures account for about one half of all patellar
fractures, followed next in frequency by comminuted fracture. Marginal
fractures are found along the edge of the patella and are not associated with
disruption of the extensor mechanism. Fractures found with more than 2 mm of
displacement or with any articular surface step-off should be considered
displaced and referred for orthopedic management.[2] [9] [11] [30] [38]
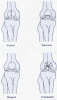 Figure 2. Types of patella fractures.
Figure 2. Types of patella fractures.
Osteochondral fractures result from either direct forces or from
patellar dislocation. Directed pressures around a point of contact cause
separation of the articular surface from the subchondral bone and from the
supporting trabecular bone. These osteochondral fragments usually heal without
complications but on occasion may become detached and form a loose body.[9]
Imaging
The patella is often difficult to evaluate in an AP knee
radiograph because of distal femur overlap. Therefore, special views of the
patella are helpful in identifying suspected fractures. Many physicians
consider merchant and sunrise views to be identical, but they are actually
obtained with different orientations. In the sunrise view, the patient is in a
prone position, and the knee flexed 115°. The x-ray beam is directed tangentially
through the patellofemoral joint with about 15° cephalad angulation.[14] The merchant view is imaged with the
patient supine and knee flexion at 45°. The central beam is caudally directed
with a 60° orientation through the patellofemoral joint.[14] Both views are adequate for assessing
vertical fractures and osteochondral defects. A sunrise view is better for
evaluating acute fractures, and a merchant view is better for assessing
cartilaginous changes to the patellofemoral joint. A lateral knee view is best
for identifying horizontal fractures and patella location.
Using the Insall-Salvati ratio, patella alta may be assessed for
possible quadriceps tendon rupture. The normal relationship is 0.8 to 1.2,
measured by comparing the length of the infrapatellar tendon (inferior pole of
the patella to the tibial tuberosity) to the length of the patella on a
lateral-view radiograph.[14] [30]
Vertically oriented grooves on the anterior surface of the patella
are normal findings and should not be considered evidence of a fracture.
Bipartite and multipartite patellae are unfused accessory ossification centers
and are normal variants.[14] They are generally found in the
superolateral corner and are often bilateral, smooth, or rounded. They should
not be confused with a fracture, and comparison views of the contralateral knee
are often helpful.
Treatment
After confirming an intact extensor mechanism, acute care consists
of controlling swelling and pain with a long straight-leg immobilizer in full
extension for 4 to 5 days, ice, compression and elevation. Initially a
non-weight bearing status is more comfortable, with advancement to toe touch
and full weight bearing as tolerated. Quadriceps strengthening should begin
during the acute phase with straight leg lifts.[2] After the acute period, patients with
nondisplaced fractures and good quadriceps control can be treated with
continuation of the straight-leg immobilizer or with above-the-knee casting.[2] [9] [11] [32] Only persons experienced with long-leg
casting should apply a full-length cast.[2] [11] The knee should be in full extension for
a total of 4 to 6 weeks. Immobilization is generally required until evidence of
fracture healing is present on repeat radiographs. After initial follow-up,
displacement of the fragments should be checked at 2 weeks with repeat
radiographs.
Referral
A major portion of the blood supply to the patella enters from the
central portion of the distal pole. A transverse fracture through the
midportion of the patella with displacement can result in nonunion or avascular
necrosis (AVN) of the proximal portion of the patella. Referral is indicated
for all displaced fractures and with any evidence of articular surface
displacement of 2 mm or more.[11] [28] [32]
PROXIMAL TIBIAL INJURIES
Tibial condylar injury ("car-bumper injury") is commonly
found after automobile/pedestrian accidents. Frequently the lateral plateau is
injured, because valgus force is the most common. Ligamentous injury is often
associated with tibial condylar injuries, because a varus or valgus force
causes a compressive force opposite the ligament being stressed until its
rupture. Thus, a valgus force applying stress to the medial collateral ligament
cantilevers a compressive force onto the lateral tibial condyle.[2] [11] [28]
Osteoporotic individuals may fracture the tibial plateau with
relatively minor trauma. Therefore any elderly person with a hemarthrosis
should be suspected of having a tibial plateau injury until proven otherwise.[28] Patients will present with inability to
bear weight, a significant effusion, joint-line or proximal tibial pain, and
decreased range of motion. Complaints of instability are common, as is ligament
instability during physical examination. A patient presenting acutely with an
isolated anterior cruciate ligament (ACL) rupture generally complains only of
instability and can usually bear weight for at least four steps. Conversely,
those with a proximal tibial fracture will not be able to bear weight (Ottawa
Knee Rules), and this finding should prompt further evaluation.
Complete assessment for ligament instability is crucial for
management. A simple nondisplaced lateral fracture with an associated ACL
rupture should be referred for surgical management,[28] whereas a nondisplaced lateral fracture
with intact ligaments could be managed by an experienced primary care
physician.[1] Acutely, analgesia is often required
before ligament assessment can be undertaken. Arthrocentesis of a tense
hemarthrosis and instillation of long-acting local anesthetic can provide
adequate analgesia and improve ligament evaluation.[32] When laxity of the joint is found,
careful assessment for fracture stability must also be made. Because an
unstable fracture can mimic a collateral injury on stressing, careful palpation
of the fracture fragment during ligament testing is crucial. Plain-film stress
views, CT scanning, or MR imaging can clarify questionable physical examination
findings.[28] Assessment of suspected proximal tibial
injuries includes a complete neurovascular examination with emphasis on
peroneal nerve testing. Therefore, evaluation of nerve and muscular function should
include ankle dorsiflexion and eversion as well as sensation in the lateral
lower leg.
Imaging
Radiographic evaluation of a suspected ligamentous knee injury
includes an AP and lateral view.[14] [30] Patients not able to ambulate at least
four steps (Ottawa Knee Rules) should have additional plain films taken to
evaluate the tibial plateau. Internal and external oblique views or tibial
plateau view (AP with 15° vertical orientation) are frequently used.[14] [30] The normal tibial plateau slopes downward
from anterior to posterior, thus making compression fractures very subtle. In
the lateral view, the normal medial tibial condyle is concave, whereas the
lateral tibial condyle is convex. A small avulsion fracture on the lateral
margin of the lateral tibial condyle near the insertion site of the lateral
capsular ligament is commonly found with internal rotation and varus stress
injuries. This type of fracture has been termed a Segond fracture after Paul Segond who first described this
injury.[2] [14] This fracture is significant, because
there is a 75% to 100% association with concurrent ACL rupture (Fig.
3) .[14] [30]
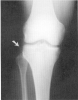 Figure 3. Segond fracture suggesting a torn ACL.
Figure 3. Segond fracture suggesting a torn ACL.
Classification
The most widely accepted classification system for plateau fractures
is the Schatzker system (Fig.
4) .[14] [28] [30] It is helpful to use a precise
description of the amount of displacement, angulation, and number of fragments,
and the classification type when describing a plateau injury to an orthopedic
consultant. Fracture types I through III are lateral plateau fractures. Type I
is a split fracture without articular depression of the lateral plateau. With
displacement, the lateral meniscus is usually torn or detached. A split
fracture with depression is a type II injury and usually results from a
combined axial and lateral force. Large compression areas usually include
meniscus entrapment and should be managed surgically. Type III injuries occur
as isolated areas of lateral plateau depression and, if extensive, may also
entrap the meniscus.[14] [28] [30] A type IV fracture is isolated to the
medial plateau, whereas types V and VI are bicondylar and bicondylar plus
tibial shaft, respectively. Experienced primary care physicians can manage
simple, nondisplaced (3 mm) types I-III fractures with no associated
ligamentous injury.[11] [32] [35] Schatzker types IV through VI are medial
plateau and bicondylar fractures and should always be referred for orthopedic
management.[28] Acute management includes long leg
immobilization, use of crutches, and RICE therapy.
 Figure 4. Lateral plateau Schatzker classification.
Figure 4. Lateral plateau Schatzker classification.
Treatment
The goal for management of tibial plateau fracture includes
minimizing the risk for posttraumatic osteoarthritis, restoring articular function,
and correcting malalignment.[28] Because limited data are available on
the maximal acceptable area of articular depression that reduces the risk for
articular dysfunction and osteoarthritis, a conservative approach may be
warranted.[16] Factors that contribute to the choice of
operative or nonoperative management include ligament and fracture stability,
displacement greater than 3 mm, comminution, and fracture location.[16] [28] In general, all high-energy fractures
should be referred for orthopedic management.[4] [16] [28] Additional factors to consider include
the patient's age and level of activity, associated medical conditions, and
osteoporosis.[4] [16] [28] Many variables affect the long-term
functional outcome of tibial plateau fractures. The single most important is
knee instability. Ligamentous instability that goes undiagnosed during the
acute assessment can profoundly affect functional recovery. Tibial plateau
fractures are often associated with incarceration of the meniscus into the
fracture site. Split and compression fractures with more than 3 mm of
displacement are at increased risk for meniscus entrapment (Fig.
5) .[4] [16] [28] Arthroscopic evaluation before ORIF may
identify incarceration of the meniscus and allow concurrent repair with the
plateau fracture. Evaluation by MR imaging should be considered when
uncertainty exists about open versus closed management.
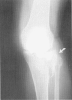 Figure 5. Schatzker type II and proximal fibular fracture.
Figure 5. Schatzker type II and proximal fibular fracture.
Drainage of a significant hemarthrosis and instillation of local
anesthetic should be used to confirm ligament and fracture stability and to
decrease pain. After stability is assured, low-energy nondisplaced type I-III
fractures can be managed with a long leg compressive stocking and a hinged knee
brace locked in full extension.[28] The patient should not bear weight for a
total of 4 to 6 weeks. Gradual passive range of motion exercises can begin
after 2 weeks, with a goal of passive flexion to 90° by 4 weeks.[28] A total of 8 to 12 weeks of
immobilization is usually necessary. Radiographs should be taken weekly for the
first 3 to 4 weeks and then spaced every 3 to 4 weeks until fracture healing.[28]
TIBIAL SPINE INJURIES
Although injuries of the tibial spine (intercondyle eminence) are
uncommon, they may be seen with an acute ACL rupture.[2] [4] [32] With the knee in a flexed position,
rotational forces can produce excessive tension of the ACL, causing either
ligament rupture or tibial spine avulsion. Because in younger pediatric
patients the ligament structure is relatively stronger than bone, tibial spine
injuries should be suspected with a positive Lachman test, hemarthrosis, and
painful ambulation.[4] Anterior-posterior and lateral
radiographs should be routinely scrutinized for a nondisplaced or hinged tibial
spine fracture when plain films of patients with acute ACL injury are examined (Fig
6) .[30] Most isolated ACL ruptures will cause
symptoms of instability, painful range of motion, and intra-articular swelling.
Inability to bear weight is not always a typical finding with cruciate injury.
Tibial plateau or tibial spine fracture should be considered in patients
presenting with ACL rupture and inability to bear weight. For suspected tibial
spine injuries, the addition of a tunnel or oblique view can increase the
sensitivity and specificity of a radiographic knee series.[14] [30]
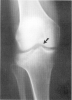 Figure 6. Type II tibial spine avulsion fracture.
Figure 6. Type II tibial spine avulsion fracture.
Classification
Three types of intercondylar eminence fracture patterns have been
described. Type I injuries are nondisplaced or incomplete avulsions. Fractures
that have displacement of the anterior one third to one half of the avulsed
fragment and that are hinged on the posterior border are classified as type II.
In the most common pattern, type III, the avulsed fragment is completely
separated from the tibial plateau.[4] [32]
Acute Care and Treatment
Early treatment includes knee immobilization in a full-length knee
immobilizer and no weight bearing. Aspiration of a tense hemarthrosis and
standard RICE therapy can significantly help control pain. Type I and II
injuries can usually be managed with closed reduction using hyperextension of
the knee and cast immobilization at 10° to 15° of flexion for 4 to 6 weeks.[4] [28] Because controversy exists over the
angle of immobilization that is recommended, orthopedic consultation is usually
indicated. All type III and irreducible type I and II fractures should be
referred for ORIF.[4]
TIBIAL TUBEROSITY FRACTURES
Sudden forced flexion of the knee against a contracted quadriceps
muscle, as occurs during a jump and forceful landing, may cause a tibial
tuberosity fracture. This injury is uncommon after apophysis closure, but may
be seen in younger patients, because their tendons can be stronger than bone.[2] [4] Care must be taken not to confuse this
injury with Osgood-Schlatter disease, which involves the anterior surface of
the tubercle.[2] [4] [32] The physical examination should include
assessment of the quadriceps extension mechanism, because its loss mandates
urgent referral. Although both types of injury can cause pain and tenderness
directly over the tuberosity, apophysis fracture will result in the knee's
being held in slight flexion (20°-40°) and in difficulty with knee extension
against resistance. Tuberosity fractures involve complete or incomplete
avulsion of the tibial tubercle, the insertion site of the patella tendon.
Classification and
Imaging
Lateral radiographs allow visualization of these fractures and the
amount of displacement. In type I injuries, the distal fragment of the tibial
tuberosity is displaced proximally and anteriorly. The patient can usually
extend the knee against gravity but has difficulty extending the knee against
resistance. Patients with type II and III tibial tuberosity fractures are
unable to extend the knee against gravity. Type II fragments are hinged at the
proximal portion, with a larger fragment extending into the physis of the
tibia. Fractures with extension into the articular surface are termed type III
injuries.[2] [4]
Treatment
Type I injuries with minimal displacement can be treated with cast
immobilization in full extension for 6 weeks.[2] [4] Postreduction displacement greater than
5 mm requires orthopedic referral and surgical management. Displacement in
younger patients should be compared with radiographs of the contralateral knee.
All type II and III injuries should be referred for ORIF.[2] [4] Routine knee films adequately
demonstrate these fractures, but comparison views are useful for suspected
nondisplaced apophysis fractures (Fig.
7) .
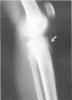 Figure 7. Type II tibial tuberosity fracture.
Figure 7. Type II tibial tuberosity fracture.
FRACTURES OF THE TIBIAL SHAFT
The tibia is the most commonly fractured long bone, and these
fractures are frequently associated with severe complications. Tibial fracture
can be challenging for both the orthopedist and primary care physician.
Controversy exists over the method of treatment, because there is a lack of
adequate randomized, controlled trials comparing closed management versus ORIF
or fixation with intramedullary rod. A recent meta-analysis found that time to
union was 20 weeks for intramedullary rod placement, 14.7 weeks for cast
immobilization, and 13 weeks for ORIF.[20] The difference between cast
immobilization and ORIF was not found to be significant. Differences in the
definitions of healing, union, and functional outcome make clinical correlation
difficult, however. The authors concluded that for most closed fractures of the
tibia time to union may be shorter after ORIF than after cast immobilization;
however, there may be a higher incidence of complications with ORIF.
Although debate continues over surgical versus conservative
management of tibial shaft fractures, acute care and fracture stabilization
principles are the basis of primary care management.[5] [15] [20] Besides being the most commonly
fractured long bone, the tibia is also the most common open fracture.[1] [26] Initial evaluation should include a
thorough inspection for soft-tissue defects. Wounds to the surface of the lower
leg may communicate with an underlying fracture, which may have become
partially reduced. When in doubt the primary care physician should assume that
an open fracture is present and seek prompt orthopedic consultation. Open
fractures should be dressed with moist, sterile bandaging and splinted in
place. If the patient has absent distal pulses, an attempt at fracture
reduction may be warranted.[1] A long-leg, padded posterior splint with
the knee in about 10° of flexion should be placed with two assistants holding
above and below the fracture site. An elastic bandage should be lightly wrapped
around the limb.
Regular neurovascular checks should be carried out, because
compartment syndrome is a frequent sequela of lower-extremity injury.[28] If the skin over the fracture site is
tented and ischemic, some gentle axial traction may lessen the risk for an
evolving open fracture. Acute care should include adequate analgesia, because
the process of splint immobilization and patient transfer can be quite painful.
Frequently, intravenous access is warranted for pain control, administration of
antiemetics, and fluid replacement.
Imaging and Classification
A cross-table lateral and AP view of the entire tibia is generally
sufficient for diagnosis (Fig.
8) .[14] [30] Fracture immobilization should take
place before radiologic studies, because moving patients with lower-extremity
trauma can cause unnecessary pain and increase the odds of converting a closed
fracture to an open one. For patients with gross deformity, intravenous access
and analgesia is preferable before splint immobilization. Careful assessment of
the knee and ankle is required before imaging studies, because there is a high
incidence of associated knee and ankle injuries. Long-bone fractures are best
described in terms of their features, because no classification scheme has been
universally accepted.[26] Table
3 . lists the features of long-bone fractures in the order in which they
should be communicated to another physician.
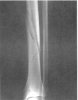 Figure 8. Closed distal third comminuted fracture of the left tibia.
The fracture is considered nondisplaced, as there is less than 5°
angulation in the AP plane
and no rotation abnormality.
Figure 8. Closed distal third comminuted fracture of the left tibia.
The fracture is considered nondisplaced, as there is less than 5°
angulation in the AP plane
and no rotation abnormality.
|
TABLE 3 -- Descriptive Terminology For
Long-Bone Fracture |
|
|
Type |
Open versus Closed |
|
Location |
Proximal,
middle, and distal third |
|
|
Proximal
or dustal diaphyseal-metaphyseal junction |
|
Configuration |
Transverse,
oblique, spiral, and comminuted |
|
Displacement |
25%,
50%, 75%, complete |
|
Angulation |
In
degrees of distal fragment in relation to the proximal fragment. AP, varus,
or valgus (apex of the fracture points towards the force) |
|
Length |
Measured
in mm of overlap or distraction |
|
Rotation |
Degrees |
|
Associated |
Fibula
fracture and other injuries |
|
Nondisplaced |
|
|
AP = anterior-posterior. |
|
Treatment
Because no clear consensus exists for management of tibial shaft
fractures, assessment of a patient's likelihood for early weight bearing helps
provide indications for surgical versus conservative management.[29] [40] A retrospective, nonrandomized study
found earlier rates of healing with early weight bearing than with non-weight
bearing.[15] Multiple studies have corroborated this
finding and the correlation between delayed weight bearing and delayed union
and nonunion.[40] Therefore, patients who have comorbid
conditions that limit early ambulation should be considered for ORIF. When
making decisions about fracture management each fracture should be treated as
unique. All factors involved contribute to the management decision and
prognosis.
Primary care physicians experienced in plaster casting can manage
lowenergy, minimally displaced (<4 mm), stable, isolated shaft fractures
with closed reduction and long leg casting.[11] [35] After the acute swelling has stabilized
with elevation and ice, a walking long leg cast should be applied with the knee
in 0° to 5° of flexion.[28] A walking boot should be placed over the
cast to assist with ambulation. Gradual weight bearing should be initiated as
tolerated, with the goal of full weight bearing by 2 weeks. Early ambulation
should be with assistance of crutches and heel pressure. Weekly radiographs
should be taken to confirm fracture stability.[28] At 4 weeks, the plaster cast should be
removed, and the leg should be assessed for fracture healing. At this time,
reliable patients can be switched to a patellar tendon-bearing orthosis or a
long-leg fiberglass cast.[5] [15] [20] [28] [29] A common complication of prolonged knee
immobilization is knee stiffness. Many studies have found that the rates of
union using a patellar tendon-bearing cast or orthosis that allows earlier knee
motion are comparable to those obtained with long-leg casting. [29]
Patients should be cautioned about compartment syndrome after
casting and given instructions for quadriceps-strengthening exercises. After
weekly evaluations for the first month, the patient can have follow-up visits
lengthened to every 3 to 4 weeks. Radiographs should be taken with each
re-examination; evidence of fracture healing should be present by 14 weeks. The
rate of healing is quite variable, and patients should be counseled that
low-energy, minimally displaced fractures heal by 21 weeks in 75% of patients.
About 90% of patients are clinically healed by 26 weeks.[29]
Referral
Indications for referral include combined tibial and fibular
injuries, floating knee injuries, unstable or displaced fractures greater than
4 mm, and comminuted fractures. All high-energy fractures should be referred,
as should rotational or angulation abnormalities greater than 5°. Although
fractures are considered nondisplaced with less than 10° angulation in the
anterior/posterior plane, multiple planes and multiple factors are involved
with a tibial shaft injury, and most primary care physicians should seek
orthopedic consultation.[5] [15] [20] [26] [28] [40]
PROXIMAL AND MIDSHAFT FIBULAR FRACTURES
Although the fibula is not significantly involved in weight
bearing, it does have a critical role in knee and ankle stability. The proximal
fibula serves as the attachment site for the lateral collateral ligament and
biceps femoris. It also acts to dissipate torsional stress of the ankle, so it
must be examined in ankle injuries to rule out a compensatory Maisonneuve
fracture. The distal portion helps form the lateral support of the ankle and
serves as the attachment point for the lateral ligaments. Primary care
physicians can manage isolated fibular fractures, with this caveat: proximal fibular fractures indicate knee instability
until proven otherwise.[32] Proximal fractures may also be
associated with common peroneal nerve injury. Therefore, testing for ankle
dorsiflexion and sensation of the first web space is essential.
Isolated fractures of the fibula can be caused by direct or
indirect forces. A direct blow to the lateral leg tends to cause a transverse
or comminuted fracture. Indirect rotational force tends to cause oblique
fractures, whereas varus stress causes avulsion injury. Most patients will be
able to walk with an isolated fibular fracture, but difficulty in walking
should prompt further evaluation for associated fracture or ligament
instability.[11] [28]
Imaging and
Classification
When ordering radiographic studies, it is advisable to obtain
studies above and below the joint if any ankle or knee tenderness is elicited
on physical examination. Identification of a spiral fibula fracture or a
fracture that occurs at the junction of the middle and distal thirds may
warrant ankle radiographs, because associated ligament and ankle injury are
common with these fracture patterns.[14] [30] Lateral and AP views are generally
sufficient for fracture identification. Descriptive terminology is best used,
as was discussed previously (Table
3) . Because proximal fibular fractures are commonly associated with tibial
plateau fractures (split and compression, type II), a thorough inspection of the
radiographs is warranted.
Treatment
As with any lower-extremity injury, elevation, ice, analgesics,
and immobilization with a posterior splint are the mainstays of acute care. The
patient should not bear weight until the initial follow-up visit. Management of
isolated proximal fibular head fractures should include careful evaluation for
common peroneal nerve injury and lateral collateral ligament rupture.[28] Small avulsion and nondisplaced
fractures to the fibula neck and head can be treated symptomatically with a
knee immobilizer and crutches for comfort.[28] The patient can advance to a hinged knee
brace when able to bear weight comfortably. Four to 6 weeks of protection from
lateral motion and rotational forces is generally sufficient for healing.
For unstable midshaft combination fractures, a dual posterior and
stirrup splint provides excellent stabilization. Application first of the
full-length posterior splint with a light elastic wrap (leaving the toes
exposed) followed by a full-length stirrup splint will provide excellent
fracture stabilization and pain relief. Leaving a small opening with the
elastic bandage near the medial malleolus (posterior tibial artery) and the
dorsalis pedis artery is helpful for future pulse checks. Excessive cast molding
and elastic bandage tension can increase the likelihood of developing
compartment syndrome.
Because the fibula is minimally involved with weight bearing,
nondisplaced midshaft fractures usually heal without complications. Casting,
however, can cause a serious complication related to inadequate padding near
the peroneal nerve. Injury to the peroneal nerve can cause long-term
disability, and additional cast padding near the proximal portion of the fibula
is advisable. After the acute period, in 4 to 5 days, a short leg walking cast
or cast walking boot should be applied for 4 to 6 weeks.[8] [28] [32] Gradual progression to weight bearing
should be as tolerated, and healing of the fracture should be completed by 8
weeks. For reliable patients with minimal tenderness, assisted ambulation with
crutches and elastic wrap from the ankle to above the knee may be adequate.[11] [28]
Referral is indicated for significant displacement and severe
comminution. Development of compartment syndrome or peroneal nerve involvement
is also an indication for orthopedic consultation.[11] [26] [28] [40]
INJURIES TO THE ANKLE JOINT
Ankle injury is the most common lower-extremity injury seen in
many primary care practices.[10] Familiarity with a thorough ligamentous
examination and the OAR is essential for proper management. Approximately 15%
of persons evaluated for acute ankle injury have a significant fracture.
Application of CDRs can benefit patient care by decreasing cost and time spent
waiting.[22] Multiple studies have validated the
original ankle rules, and attempts to refine these rules have not significantly
improved their sensitivity or specificity. Pooled analysis of the OAR conducted
at university and community hospital emergency departments had a combined
sensitivity of 97% or higher for ankle and foot injuries and a negative
predictive value of 99%.[22] Although the specificity is only 31% to
63% and the positive predictive value is 20%, the OAR have consistently been
shown to be effective in decreasing the number of radiologic studies needed by
34%. Therefore, the OAR are more effective in ruling out fractures than ruling
them in.[22]
The clinical usefulness of the OAR in the primary care setting has
been an area of debate. Proponents argue that extrapolation of emergency room
CDRs are not valid, because the fracture frequency of the foot and ankle
approaches 20% in the emergency room, compared with only about 8.5% in the
primary care setting.[22] More recently, several studies involving
pediatric and primary care physician clinics found sensitivity and specificity
identical to emergency department CDRs, and similar time and cost benefits.[22]
Successful management requires determination of a stable versus
unstable fracture. The bones and ligaments of the ankle form a ring around the
ankle mortise. For instability to occur, ligamentous injury or fracture must
include both medial and lateral sides of the ring. Generally, isolated
nondisplaced distal fibular or distal tibial fractures are stable when no
ligamentous instability is present on the opposite side of the ring. Careful
evaluation of the ankle for medial and lateral swelling and ecchymosis should
be routine, and their presence should increase suspicion of an unstable injury.[10] [11] [21] [24] [39]
The three bones that make up the ankle joint (distal tibia, distal
fibula, and talus) are bound together by the joint capsule and surrounding
ligaments. The anatomic relationship of the tibial plafond (joint surface of
the distal tibia and fibula) to the talus is important for ankle stability. The
talus is broader anteriorly, and dorsiflexion increases bone surface contact,
thus improving stability. This relationship causes decreased stability with
plantarflexion and accounts for the vulnerability to ligamentous injuries in
this position.[10] [11] [21] [24] [39] [42]
Forces acting on the ankle lead to typical fracture or ligamentous
patterns. Determining the position of the ankle during injury can assist in
assessment of ligament stability. Although simple, unidirectional forces can be
involved in ankle injury, generally a multidirectional component is present,
making diagnosis challenging.[21] [24] [39]
Medial complex injuries typically occur from an eversion and
abduction force. The medial complex consists of the medial malleolus, the
medial facet of the talus, and the superficial and deep components of the
deltoid ligament. Eversion of the ankle causes injury to the superficial
deltoid ligaments and, if sufficient, to the deep deltoid ligament. Avulsion of
the distal medial malleolus tends to occur with younger and older patients,
because ligamentous strength may be relatively greater in these individuals.
With continuation of these forces, impaction of the distal lateral malleolus
occurs, resulting in either rupture of the syndesmosis or oblique fracture of
the distal fibula. When external rotation is combined with an eversion force, a
proximal fibula fracture (Maisonneuve fracture) may occur.[10] [11] [21] [24]
The lateral complex, which consists of the distal fibula, the
lateral facet of the talus, and the lateral collateral ligaments of the ankle
and subtalar joint, is the most common ankle injury. Lateral malleolus injury
typically occurs with inversion and adduction forces. The inversion force first
strains the lateral ligament complex or avulses (transverse fracture) the
lateral malleolus. With continuation of this force, the talus impacts the
medial malleolus, causing an oblique fracture of the distal tibia (Fig.
9) . Posterior malleolus injury is found with a combination of forces
(eversion, abduction, and vertical loading). When high-energy impaction or
axial compression is involved, a severely comminuted fracture of the tibial
plafond, called a pilon fracture, may occur.[10] [11] [21] [24] [39]
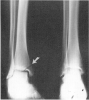 Figure 9. Oblique fracture of the medial malleolus fracture.
Figure 9. Oblique fracture of the medial malleolus fracture.
Physical examination of the ankle should assess for swelling and
ecchymosis. Swelling is, however, a function of time and is an unreliable
indicator of the presence or severity of injury. Fractures can easily be missed
by failure to check the joint above and below the area of chief complaint.
Squeezing the tibia or fibula at mid-calf allows assessment of a proximal
Maisonneuve fracture. The clinician should always remember to document
neurovascular function.
Imaging
Radiographs should include an AP, lateral, and mortise view, which
is taken with the foot externally rotated 15° to 20°.[14] [30] Important radiographic relationships are
listed in Tables
4 and
5 and Figure
10 . Stress view radiographs have a limited role in evaluation of the acute
ankle injury. They should only be taken under anesthesia before reconstructive
surgery. A standing mortise view of the ankle can help identify ligamentous
instability in difficult-to-examine patients.[30] Comparison of the normal radiographic
relationships from the mortise and standing mortise view will show loss of the
normal tibiofibular overlap and asymmetry of clear spaces. A comparison view
with the uninjured ankle can also be useful in difficult cases.[30]
|
TABLE 4 -- Radiographic Relationships of the
Ankle Mortise View |
|
|
Area |
Normal Values |
|
Lateral clear space |
Greater
than 2 mm is suspicious for a syndesmosis sprain |
|
Tibiofibular overlap |
Greater
than 1 mm |
|
Medial clear space |
Symmetrical
with lateral clear space |
|
TABLE 5 -- Radiographic Relationships of the
AP Ankle View |
|
|
Area |
Normal Values |
|
Medial clear space |
Greater
than 3 mm can indicate deltoid ligament of syndesmosis |
|
Tibiofibular clear |
Normally
less than 6 mm |
|
Standing AP View |
Syndesmotic
widening greater than 3 mm from the AP view indicates an syndesmotic sprain |
|
AP = anterior-posterior. |
|
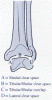 Figure 10. Radiographic anatomy of the ankle mortise. A
= medial clear space; B
= tibular/fibular clear
space; C = tibular/fibular
overlap; D = lateral clear space.
Figure 10. Radiographic anatomy of the ankle mortise. A
= medial clear space; B
= tibular/fibular clear
space; C = tibular/fibular
overlap; D = lateral clear space.
In reviewing ankle radiographs, it should be remembered that
transverse fractures usually result from avulsion forces, whereas oblique
fractures usually result from impaction of the talus against the malleoli.[30] [32] Vertical malleolar fractures are caused
by impaction with the talus. Any displaced malleolar fracture should be
considered as unstable and is almost always associated with ligamentous injury
of the opposite side. In general, all oblique fractures of the medial malleolus
and oblique fractures 2 to 3 inches proximal to the joint line should be
assumed to have associated ligament injury and should be considered unstable.[32]
In addition to using the radiographic ABCs to evaluate ankle
films, checking for the five most commonly missed foot and ankles fractures is
advisable.[30] [35] The mnemonic FLOAT is helpful for recall (Fig.
11) : close attention to the Fifth metatarsal base, Lateral process of
the talus, Os
trigone or posterior malleolus, Anterior process of the calcaneus, and Talar dome can help
correlate radiographic findings with tenderness on physical examination (Fig.
12) .
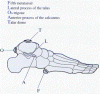 Figure 11. Five most commonly missed ankle and foot fractures using the
FLOAT mnemonic. (Adapted from Steinberg GG, Akins CM: Orthopaedics in Primary
Care, ed 3. Philadelphia, Lippincott Williams & Wilkins,
1999; with permission.)
Figure 11. Five most commonly missed ankle and foot fractures using the
FLOAT mnemonic. (Adapted from Steinberg GG, Akins CM: Orthopaedics in Primary
Care, ed 3. Philadelphia, Lippincott Williams & Wilkins,
1999; with permission.)
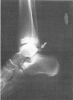 Figure 12. Os trigone fracture of the right ankle.
Figure 12. Os trigone fracture of the right ankle.
Classification
The Danis-Weber system of classification for ankle fractures is
the most useful for primary care management. This classification system is
simple and helpful in deciding which fractures need referral.[14] [30] This classification scheme is based on
the level of the fracture in relationship to the joint mortise of the distal
fibula (Fig.
13) . [11] [14] [30] [35] Type A fractures are horizontal avulsion
fractures found below the mortise. They are stable and amenable to being
treated with closed reduction and casting unless accompanied with a medial
malleolus fracture. A spiral fracture that starts at the level of the mortise
is a type B fracture (Figs.
13 , 14)
, which occurs as the result of external rotational forces. These fractures may
be stable or unstable, depending on ligamentous involvement and associated
fractures. The type C fracture is above the level of the mortise and disrupts
the ligamentous attachment between the fibula and tibia inferior to the
fracture. These fractures are considered very unstable and require open
reduction and internal fixation.[14] [24] [28] [39]
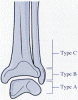 Figure 13. Danis-Weber classification of fibular fractures.
Figure 13. Danis-Weber classification of fibular fractures.
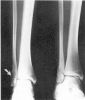 Figure 14. Danis-Weber class II fracture.
Figure 14. Danis-Weber class II fracture.
Acute Care
As always, acute management involves analgesia for pain,
immobilization, keeping the patient comfortable, and preventing shock. Using
either a well-padded posterior or stirrup splint, the patient should not bear
weight until definitive treatment in 3 to 4 days. Small avulsion Danis-Weber
type A fractures can be treated symptomatically with an ankle stirrup brace and
with ambulation allowed as tolerated. The patient should apply ice to the
injured area over a compressive dressing for 20 minutes every 2 to 3 hours for
the first 24 hours, then every 4 to 6 hours until casting. Keeping the limb
elevated above the level of the heart will also significantly reduce swelling.
Treatment
Isolated lateral malleolus fractures are the most common fractures
involving the ankle. Most inversion injuries result in an isolated sprain of
the anterior talofibular ligament. A small avulsion fracture, however, can
occasionally be seen near the distal portion of the lateral malleolus. Barely
visible osseous chip fractures should not alter the routine active management
of grade 1 and grade 2 ankle sprains.[11] [32]
Most primary care physicians can manage isolated nondisplaced type
A Danis-Weber fractures.[11] [32] [37] More experienced providers can treat
stable, nondisplaced fractures to the medial or posterior malleolus with
involvement of less than 25% of the articular surface. Instability is probable
with vertical medial malleolar fractures, displaced medial or lateral
fractures, and inversion medial malleolar fractures.[10] [11] [32] [37] Cast immobilization can be accomplished
after the acute period with either a short leg walking cast or a walking cast
fracture boot for a reliable patient. The ankle should be casted in a neutral
position to avoid shortening of the Achilles tendon. Generally, 4 to 6 weeks
are required for evidence of radiographic healing.[11] [28] [37] If the fracture site is not tender,
gradual weight bearing and ankle rehabilitation can begin. If no evidence of
fracture healing is present, an additional 2 to 4 weeks may be required. If
there is no evidence of fracture healing by 8 weeks, orthopedic referral is mandatory.[11] [28] [37]
After the immobilization period, the patient should begin ankle
rehabilitation. Range of motion and strength return quickly in young patients,
and referral to physical therapy may not be needed. Calf stretching and
strengthening exercises and with range-of-motion exercises can be performed at
home by the motivated patient. Patients with premorbid conditions and increased
age usually require formal physical therapy.
Referral
Orthopedic consultation is advisable for all fractures displaced
greater than 2 mm, because minor changes involving the joint mortise can cause
chronic pain and early osteoarthritis.[11] [28] [32] [42] Any suspected unstable injury
(Danis-Weber classification type B or C) should be referred, as should all
bimalleolar fractures. Referral is also indicated for all trimalleolar
fractures, which involve fracture to both the medial and lateral malleoli and a
fracture to the posterior lip of the tibial plafond (Fig.
15) . This fracture usually results from an avulsion of the posterior
tibiofibular ligament at its insertion site. In the presence of medial
malleolar tenderness and more than 5 mm of medial clear space on the mortise
view, a presumptive diagnosis of deltoid ligament rupture should be made.[30] [32] Such an injury should be treated as
bimalleolar fracture and referred for management.[24] Fractures that show no radiographic evidence
of healing after 8 weeks should also be evaluated for ORIF.[28]
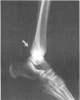 Figure 15. Bimalleolar fracture, posterior and lateral malleolus.
Figure 15. Bimalleolar fracture, posterior and lateral malleolus.
TARSAL INJURIES
Foot injuries are frequently seen by primary care physicians and
can provide ample frustration to those who are not familiar with the anatomy
and function of the foot. The tarsal bones make up the hindfoot (calcaneus and
talus) and midfoot (navicular, cuneiforms, and cuboid); the forefoot comprises
the metatarsals. Injuries to the tarsal bones are infrequent but should be
treated cautiously when present. These bones are crucial for walking, and
injuries often have a poor prognosis.[10] [18] [37] A calcaneus body fracture should prompt
a thorough thoracolumbar examination and imaging because a significant fall is
the most common cause.[30]
The mainstay of foot injury diagnosis is a careful, complete
physical examination, because evaluation of plain films of the foot can be
challenging. A systematic evaluation should include a stepwise review of the
bones found in the hindfoot, midfoot, and forefoot. The calcaneus is the most
commonly fractured tarsal bone; injury usually results from compressive forces
from a fall or motor vehicle accident. Talus fractures are usually minor,
involving an avulsion injury after an ankle sprain. Talar neck fractures and
dislocations require emergent referral, however, because the tenuous blood
supply to the body of the talus arrives through the neck.[11] [28] [32] Avascular necrosis is a serious sequela
of failure to identify or appropriately refer talus injuries.[11] [28] [32] [37]
Midfoot fractures are uncommon except as the result of blunt or
severe trauma. Because the midfoot bones are the least mobile bones of the
foot, fractures to this area usually involve multiple bones. Crush injuries to
the midfoot result in multiple comminuted fractures, and identification of one
fracture necessitates a more detailed evaluation of the surrounding midfoot.[7] [10] Navicular fractures are mostly eversion
injuries resulting in dorsal avulsion fractures. Stress fractures to the
navicular are common among runners, and point tenderness to this area with no
evidence of fracture on normal plain films should prompt additional studies
(bone scan or CT scan).[10] [38]
Imaging of the Tarsal
Bones
The standard foot radiographic series includes AP, lateral, and
internal (medial) oblique views.[14] [30] When dealing with the varying densities
between the forefoot and hindfoot, additional views are useful for certain
fractures. Suspected fractures to the calcaneus are best visualized with a
standard foot lateral view and an axial calcaneus projection.[30] Because intra-articular fractures have
poor outcomes, a clear understanding of fracture extension is critical. The
addition of a calcaneus lateromedial oblique view can improve visualization of
the anterior aspect of the subtalar joint. If questions still exist about the
presence of intra-articular extension, a CT scan should be ordered.[14] [30] Bohler's angle is measured to evaluate
the magnitude of calcaneus compression.[11] [30] Bohler's angle can be determined by
measuring the angle formed between two lines, one of which is drawn along the
superior surface of the posterior tuberosity and the other connecting the
superior tip of the subtalar articular surface and the superior tip of the
anterior process (Fig.
16) . Although a normal Bohler's angle does not exclude a calcaneal
fracture, angles less than 20° are found with compressive injuries.[30] Bilateral calcaneus fractures are
common; therefore, radiographic examination of the uninjured foot should be
considered.[30]
The talus is evaluated with a standard ankle series (AP, mortise,
and lateral) and a 45° internal oblique view to see the body of the talus, if
needed.[14] [30] Because radiographic evaluation of the
talar neck can be difficult, CT examination may be needed when there is strong
suspicion of a talar neck injury.[30] [37] Talar neck fractures occur after
forcible dorsiflexion of the talar neck against the tibial plafond, as occurs
when the foot is slammed on the brake during a motor vehicle accident.
Acute Care
After evaluation for distal pulses and nerve function, application
of a padded posterior splint, compressive dressing, elevation, and ice are the
mainstays of care. The patient should be instructed not to bear weight until
radiographic evaluation has taken place. Fractures that require casting should
be re-evaluated in 3 to 4 days for definitive care.[32]
Calcaneus Fractures
Primary care management of calcaneus fractures is based on
distinguishing between intra-articular and extra-articular fractures. Because
70% of calcaneus fractures involve the subtalar joint, the finding of an
isolated extra-articular fracture should prompt close inspection of the
subtalar joint.[28] [30] [37] Extra-articular fractures generally
result from twisting injuries, such as an avulsion of the anterior process
(bifurcate ligament rupture). Some of the common extra-articular fractures that
can be managed by primary care physicians include simple nondisplaced (less
than 2 mm) fractures involving the posterior tuberosity, anterior process, or
lateral process and body fractures with no subtalar joint involvement.[10] [11] [28] [37] Most intra-articular calcaneus injuries
present with significant heel pain, difficulty with walking, plantarflexion
pain, and ecchymosis after an axial load from jumping or falling. These
injuries merit orthopedic referral.
Treatment
Acute care consists of RICE therapy with a bulky compressive
dressing to help control swelling.[10] [28] [37] Fracture blisters are a common complication
with calcaneus fractures, and many physicians advocate bed rest and elevation
to help minimize their formation. The patient should not bear weight until
follow-up in 4 to 5 days. Generally, nondisplaced extra-articular fractures can
be managed with either a short leg cast or walking boot for 4 to 6 weeks.[3] [10] [11] [28] [37] Small minimally displaced avulsion
fractures do well, but larger displaced avulsion and intra-articular fractures
should be referred promptly for ORIF.[3] [10] [11] [13] [18] [28] [37] Healing time for most fractures is
between 6 and 12 weeks, but pain and stiffness in the area may continue for
months. Follow-up visits should be made every 3 to 4 weeks, and repeat
radiographs should be done after immobilization.
Tuberosity fractures usually result from an Achilles tendon
avulsion injury. Patients present with pain, swelling, ecchymosis, and weakness
with stair climbing. Small, nondisplaced fractures may be treated with a short
leg cast (5° to 10° of plantarflexion) for 6 weeks.[11] [26] [30] [37] Fracture stabilization should be
confirmed radiographically in 1 week. A small avulsion of the distal Achilles
tendon insertion can occur and, if nondisplaced with a negative (intact)
Thompson test, can be managed with a short leg cast in plantarflexion.[28] Larger displaced fragments should be
referred for ORIF. After 6 to 8 weeks, physical therapy is initiated, because a
progressive stretching program is needed.[11] [28]
Inversion and axial forces may cause tenderness over the
posterolateral heel. The axial calcaneal view is the best for evaluation of
medial or lateral process injuries. Nondisplaced fractures of the lateral
process can be treated with a short leg walking cast for 4 weeks.[11] [28] [37]
Ankle sprains with planterflexion and inversion forces may cause
avulsion of the anterior process at the insertion site of the bifurcate
ligament.[11] [13] [18] [28] [37] Localized swelling and tenderness are
present about 1.5 to 2.5 cm distal and slightly inferior to the lateral
malleolus (anterior and inferior to the anterior talofibular ligament
insertion). This fracture is best viewed on the lateral radiograph and is
easily missed unless the anterior process is specifically examined.[30] Small avulsion fractures with minimal
displacement can be treated with a walking cast boot for 2 to 4 weeks.[10] Larger fragments or significant displacement
should be referred for ORIF.[13] [18]
Nondisplaced fractures to the body of the calcaneus without
subtalar joint involvement tend to do well regardless of the method of
treatment.[11] [13] [18] [28] [37] When uncertainly exists concerning
subtalar joint involvement, oblique radiographic views or CT scans should be
considered. Fractures that show loss of Bohler's angle, widening of the heel,
or displacement should be referred for orthopedic management.[28] After the acute phase, range-of-motion
exercises should begin, and toe-touch ambulation should be used for 4 to 6
weeks.[11] [28] Gradual progression to full weight
bearing should start with clinical and radiographic evidence of healing.
Fractures of the Talus
The talus is a unique bone, because about 60% of it is covered by
cartilage, and it acts as the distribution point for the body's weight to the
foot. The tenuous blood supply enters distally and flows in a posterior
direction. The talus articulates with the tibial plafond above, the calcaneus
below, and the navicular anteriorly.[28] [38] The posterior and lateral processes of
the talus are prone to injury with eversion and inversion.[10] [37] [38] Although most fractures to the talus are
small chip or avulsion fractures, osteochondral fractures can occur with severe
ankle sprains, when the talar head impacts against either the medial or lateral
malleolus, resulting in cartilage injury.
It is important to recognize talar neck injuries, because
displacement should be managed with urgent surgical intervention. Avascular
necrosis is a serious complication, and controversy exists over the best
management.[3] [8] [11] [28] Although nondisplaced vertical fractures
can be managed with a short leg non-weight bearing cast, it is best to refer
these patients' management. [28] When questions exist about whether the
fracture is displaced, a CT evaluation should be done. All displaced fractures
of the talar neck and minimal displacements of the subtalar joint should be
referred promptly.[8] [28]
Fractures of the lateral process of the talus occur after severe
inversion and dorsiflexion injury.[28] [37] Patients will present with minimal
tenderness over the anterior talofibular ligament (ATF) and have a normal
anterior drawer test and pain with inversion. Localized tenderness below the
fibula is common, and careful attention to this area on plain film should help
localize the fracture.[37] Small nondisplaced fractures with joint
involvement of less than 10% can be treated symptomatically with a cast boot or
short leg walking cast for 6 weeks.[10] [28] [37] Displaced fractures greater than 3 mm
and those involving the subtalar articulation should be referred. CT scanning
may be necessary, because joint involvement can be difficult to determine on
radiographs.
A fracture to the os trigonum or posterior process of the talus
occurs primarily from repeated forceful plantarflexion.[10] This injury is more common in athletes
such as ballet dancers assuming pointe or demipointe positions and ice skaters.
They present with pain localized to the posterior ankle and anterior to the
Achilles tendon. Because most of these injuries are a form of impingement,
conservative management should be tried initially with nonsteroidal
anti-inflammatory drugs (NSAIDs), limiting plantarflexion, taping, or bracing.[10] CT scan or bone scan is often needed
when conservative care fails. Use of a short leg walking cast for 4 to 6 weeks
should be considered for recalcitrant cases.
Acute osteochondral fractures generally result from inversion
injury during sports. The patient will have significant pain with weight
bearing and complain of pain inside the ankle rather than instability symptoms.
A joint effusion may be seen on physical examination. The examiner should palpate
the lateral talar dome in plantarflexion and the medial aspect in dorsiflexion,
because most lesions are either posteromedial or anterolateral.[28] [37] It is common for the initial radiographs
to be negative, and the patient should be instructed about the importance of
follow-up should pain continue. Patients with chronic pain should have repeat
radiographs, and if these radiographs are negative, a bone scan or CT scan is
appropriate. Osteochondral lesions are classified into four stages. Stage I is a
small area of compression of the subchondral bone. Stage II lesions are
partially attached but nondisplaced osteochondral fragments, whereas stage III
lesions are completely detached but nondisplaced fragments. Stage IV lesions
are completely displaced fragments.[28] Acute stage I and II fractures can be
treated with a non-weightbearing short leg cast for 6 weeks, but referral is
indicated for all stage III and IV injuries.[28] [37] [38] [41]
MIDFOOT
Fractures to the midfoot are uncommon and generally are found only
in the setting of local trauma or eversion plantarflexion injury. The midfoot
is made up of the navicular, cuboid, and cuneiforms bones, which articulate
with the metatarsals anteriorly and with the talus and calcaneus posteriorly.
Imaging
Midfoot fractures are best evaluated with a standard three-view
foot series with the addition of an external oblique foot view.[14] [30] Because navicular fractures can be
complicated by AVN and nonunion, CT evaluation is often necessary when there is
significant comminution or displacement. Care must be taken when evaluating
midfoot radiographs, because accessory bones are a common finding, and more
than one accessory navicular bone has been diagnosed as a fracture. The os
tibiale externum is frequently confused with a dorsal avulsion fracture.
Accessory bones are usually bilateral, smooth with rounded edges, and
nontender, whereas avulsion fractures are tender and have sharp, irregular
edges.[14] [37]
Acute Care
Early RICE therapy with a compressive dressing and posterior
splint for comfort is appropriate for the acute injury. Stress fractures can be
casted at the initial office visit. Compartment syndrome can occur with crush
or trauma midfoot injuries, so patients should be appropriately educated about
its signs and symptoms.
Navicular Fractures
Minimally displaced dorsal avulsion fractures usually do not
involve a significant portion of the articular surface. They can be treated
with a short leg walking cast or cast boot for 4 to 6 weeks. Fragments that
involve more than 20% of the talonavicular joint should be referred for
orthopedic management, because they should be reduced acutely to restore the
articular surface. Persistent pain after casting should be evaluated for
surgical excision.[10] [11] [28] [38]
Eversion injury may result in significant tension to the insertion
sites for the posterior tibial tendon and the anterior fibers of the deltoid
ligament, causing an avulsion injury to the navicular tuberosity. Passive eversion or active inversion of
the foot will cause tenderness to this area and is characteristic of this
injury. An associated fracture to the cuboid is common with midfoot trauma, and
the finding of a navicular fracture should prompt the examiner to inspect the
radiographs closely. With minimally displaced fractures, a short leg walking
cast with the foot in neutral position can be used for 4 to 6 weeks.[10] [11] [28] [38] During casting, particular attention
should be paid to molding an adequate longitudinal arch. Nonunion may occur and
can be managed with additional immobilization for 2 to 4 weeks. Continued,
symptomatic nonunion requires referral for possible surgical excision.[28]
Fractures to the body of the navicular are usually associated with
other midfoot injuries. Nondisplaced fractures can be treated with a
below-the-knee walking cast with a well-molded longitudinal arch.[10] [11] [28] [38] Between 6 and 8 weeks are needed for
union, at which time the patient can be advanced to a molded arch support for
ambulation. All displaced fractures should be referred for orthopedic
management, because recurrent displacement can occur.
Cuboid Fracture
This classic nutcracker fracture results from a compressive force
between the calcaneus and the fifth metatarsal.[32] Crush injury to the Lisfranc joint
should also be suspected with the findings of distal cuboid or cuneiform
fractures. Cuboid fractures cause considerable pain, and patients have
difficulty walking. Treatment for nondisplaced cuboid fractures is 6 weeks in a
short leg walking cast that is well-molded and with an adequate arch support.[11] [28] [32] After the immobilization period, a
molded hard plastic foot orthotic should be used to maintain adequate arch
support for up to 6 months. Displaced and dislocated cuboid injuries should be
referred for orthopedic management.
Cuneiform Fracture
Injury to the cuneiform bones is uncommon except with direct
trauma or crushing injury. Pain and swelling are localized to the involved
area, and weight bearing is difficult. Comparison radiograph views are
frequently needed, because these fractures are often subtle. Nondisplaced
fractures can be treated with a well-molded short leg walking cast for 6 weeks.[32] [37] Displaced fractures and
fracture-dislocation injuries should be considered unstable and referred
promptly for orthopedic management.
Lisfranc Injury
The tarsometatarsal joint or the Lisfranc joint is made up of the
five metatarsal bases and the articulation with the bones of the midfoot. Most
injuries to this area are subtle, and a high index of suspicion must be present
for diagnosis. Up to 20% of Lisfranc injuries are missed on radiographic
evaluation.[7] [28] [30] The classical Lisfranc injury was first
described during the Napoleonic Wars when a rider was thrown from his horse and
was dragged with his foot caught in the stirrup. Today's version is an axial
force to the metatarsals when the toes are dorsiflexed and the ankle
plantarflexed (kneeling position).[7] [10] [30] The axial force causes the metatarsal
base to be displaced dorsally and laterally, resulting in ligamentous injury
and fracture dislocation. The most common radiographic finding is disruption of
the normal anatomic relationship between the first and second metatarsals.
Occasionally, small avulsion fragments from the medial cuneiform can be seen
between the bases of the first and second metatarsals.[30]
Imaging
A standard foot series (weight-bearing if possible) is usually
adequate for identification of a Lisfranc injury. The AP view should be
inspected closely for malalignment of the medial border of the second
metatarsal and the medial border of the medial cuneiform. On the oblique view,
the medial border of the fourth metatarsal forms a continuous line with the
medial border of the cuboid and the third metatarsal forms a continuous line
with the lateral borders of the third metatarsal and lateral cuneiform.[7] [10] [28] [30] [38] If the patient is able to stand,
weight-bearing views should be used. The lateral view should be inspected for
dorsal displacement of the proximal base of the second metatarsal and
flattening of longitudinal arch (during weight bearing).[30] Comparison views are often helpful, and
for questionable cases CT evaluation is necessary.[7] [30]
Treatment
The key to treatment is early recognition, because Lisfranc
injuries can be difficult to treat. If suspected, each metatarsal and each bone
of the midfoot should be palpated. Pain localized to the tarsometatarsal joints
should prompt careful radiologic evaluation. Inability to bear weight standing
on tiptoes is another diagnostic clue. Considerable controversy exists over
open versus closed management of a Lisfranc fracture or dislocation. Treatment
largely depends on the magnitude of injury, and any displacement greater than 1
mm should be referred for ORIF.[7] [10] [28] Patients with mild to moderate trauma
and no tarsometatarsal ligament instability on weight-bearing radiographs can
be managed with immobilization. Most primary care physicians, however, should
refer these patients for orthopedic management.
FOREFOOT
Fractures of the forefoot, which is composed of the metatarsal and
phalanges, are among the fractures most commonly seen by primary care
physicians.[11] [28] [38] [41] Most isolated forefoot fractures are
treated conservatively. Fractures to the base of the fifth metatarsal, however,
must be accurately diagnosed to avoid nonunion with a Jones fracture. Most
metatarsal fractures result from trauma or from an inversion ankle injury that
causes an avulsion fracture to the base of the fifth metatarsal. Generally,
metatarsal fractures are isolated and minimally displaced, because the
surrounding supporting ligaments tend to splint the fractured bone in place.[11] [28] [38] [41] Localized pain and tenderness are
usually present, as is difficulty with weight bearing. Swelling can be severe,
and the potential for compartment syndrome exists.
Imaging
Metatarsal and phalanges fractures are usually well visualized
with the standard foot series; however, distal phalanx fractures may be
difficult to visualize, as the central ray of the x-ray beam is focused near
the midfoot. As a coned down AP view may be beneficial in some situations.[30] Fractures are described as transverse,
oblique, spiral, comminuted, intra-articular, or extra-articular to the base,
shaft, or head of the metatarsal.[28]
Acute Care
Initial management of a metatarsal fracture should focus on
reducing swelling and immobilization with a posterior splint. Patients should
not bear weight until follow-up examination. Initial follow-up should be in 3
to 5 days for casting or a postoperative wooden shoe.
Fractures of the Fifth
Metatarsal
The most common fracture to the base of the fifth metatarsal
results from an inversion ankle injury. The peroneus brevis tendon insertion
causes an avulsion of the proximal portion of the metatarsal base.[10] [11] [38] [41] Confusion exists for some primary care
physicians, because this tuberosity avulsion fracture has been inappropriately
called a "pseudo-Jones fracture" (Fig.
17) . Properly designated, a Jone's fracture is a transverse fracture
through the proximal fifth metatarsal shaft and has a considerable incidence of
nonunion because it is in a watershed area of blood supply.[10] [11] [28] [30] [38] [41]
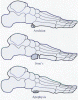 Figure 17. Types of fifth metatarsal fractures.
Figure 17. Types of fifth metatarsal fractures.
Avulsion injury to the base of the fifth metatarsal is commonly
missed, because it is frequently not included in a routine ankle series or
palpated during physical examination.[30] An unfused apophysis is frequently
confused in children and adolescents as a fifth metatarsal avulsion injury.
Tuberosity avulsion fractures are transverse, whereas the unfused apophysis is
oriented along the long axis of the metatarsal.[28] [38] [41] Also, the os vesalianum is an accessory
bone that is often mistaken for a fracture. Accessory bones have smooth
cortical margins and are usually bilateral.[30]
Nondisplaced tuberosity fractures can be managed with a wooden
postoperative shoe or cast fracture boot, with weight bearing as tolerated for
2 to 4 weeks.[10] [11] [38] [41] For those with a displaced fragment
greater than 3 mm, or- thopedic referral should be considered. Fractures to the
metaphysealdiaphyseal junction (Jone's fractures) result from a vertical load
placed on the lateral foot. Jones fractures can be managed with 6 to 8 weeks in
a non-weight-bearing short-leg cast if nondisplaced but are best referred.[11] [28] Frequent follow-up is essen-tial, and
nonunion after 3 months of therapy should be referred for ORIF. Because a high
rate of delayed union and nonunion occurs with this fracture, consultation for
ORIF should be considered.[10] [28] [38] [41] All displaced Jones fractures and
intraarticular tuberosity fractures should be referred for orthopedic
management.
Fractures of the First
to Fourth Metatarsal
Fractures to the metatarsal bones are usually caused by direct
impact from falling objects or indirect forces such as a twisting fall.
Crushing injuries to the foot are frequently associated with compartment
syndrome, neurovascular dysfunction, and decreased tissue viability.[10] [28] [38] [41] Initial inspection should focus on a
thorough musculoskeletal examination and documentation of neurovascular
function. Because the first metatarsal has important weight-bearing function,
suspected fractures to this area should be carefully evaluated for any displacement
on the radiograph.[28] [41] Fracture to the metatarsals from direct
trauma usually causes displacement in the sagittal or AP plane. Therefore, the
lateral radiograph should be thoroughly inspected for angular deformity.[28] [41]
Fractures to the metatarsal bases are rare and should increase
suspicion for a Lisfranc injury. Most nondisplaced metatarsal shaft fractures
heal well and can be treated by primary care physicians.[11] [38] All displaced fractures to the first or
fifth metatarsal should be referred for possible ORIF.[28] [41] Nondisplaced or minimally displaced
second through fourth metatarsal shaft and neck fractures can be treated with a
stiff shoe, short-leg cast, or walking fracture boot for 2 to 4 weeks.[10] [11] [28] [38] [41] Early ambulation as tolerated should be
the goal, because reflex sympathetic dystrophy is associated with prolonged
immobilization.[38] [41] Medial or lateral displacement of the
second, third, and fourth metatarsals in the frontal plane is generally well
tolerated and heals without risk of any long-term disability.[41] Dorsal or sagittal plane angulation is
poorly tolerated, however, and should be referred for closed reduction.[28] [41] Nondisplaced fractures to the first
metatarsal are best treated with a non-weight-bearing short leg cast for 2 to 3
weeks. After initial immobilization, a wooden postoperative shoe can be used
for comfort.
Phalangeal Fractures
Toe fractures are often trivialized, but they can be quite
painful. Phalanx fracture to the second through fifth toes can be managed with
buddy taping, a small piece of gauze to prevent maceration of the skin, and a
wooden postoperative shoe for comfort.[32] [37] [41]
Most fractures to the great toe are caused by trauma from a direct
blow or an axial compression. Nondisplaced fractures can be treated with a
wooden postoperative shoe or a walking cast with a toe plate.[10] [11] [32] [38] Fractures that are displaced or have an
intra-articular component may require surgical fixation. Usually 2 to 4 weeks
is adequate for treatment. A subungual hematoma is often indicative of a
phalanx fracture.
SUMMARY
This review of acute fracture management is designed to provide a
quick reference for many common fractures but is not all inclusive. The
referral guidelines depend on physician experience; when questions exist
concerning fracture management, consultation is generally advisable. The
enclosed fracture management summary tables will hopefully provide a quick
reference for which radiologic views to order, treatment pearls, basic
management, and when to refer (Tables
6 ,
7 , and 8)
. Finally, inspection of radiographs whenever possible should not only include
the radiologist interpretation, but evaluation by the physician as well. The
benefit of knowing the location of point tenderness, swelling, and ecchymosis
gives the primary care physician the advantage in making the correct diagnosis.
|
TABLE 6 -- Fracture Management Summary: Knee |
|||||||
|
Fracture Type |
Radiographic View |
Landmarks |
Acute Treatment Maxims |
Definitive Treatment |
Follow-up |
Repeat Radiographs |
Referral |
|
Femoral condylar |
AP,
lateral knee, and sunrise (AP pelvis; AP and lateral hip) |
Medial
femoral condyle is usually larger than lateral condyle on lateral radiograph |
Check
the popliteal fossa for hematoma |
ORIF |
Orthopedic |
Orthopedic |
Always |
|
|
|
|
|
Cast
bracing |
|
|
|
|
Patella |
Sunrise,
AP and lateral knee or merchant view |
Patella
ratio (0.8-1.2) |
Check
extensor mechanism knee immobilizer |
Long
leg immobilizer or cylinder cast for 4-6 weeks |
4-5
days, then every 3-4 weeks |
At
2 weeks, then 4-6 weeks |
Displaced
|
|
Tibial plateau |
AP
and lateral knee, oblique or tunnel view ± sunrise view |
ACL
rupture is suggested with Segond fracture |
Arthrocentesis
for tense hemarthrosis. Long leg splint (NWB) |
Low-energy
types 1-3 nondisplaced |
Weekly
for 3-4 weeks then every 3 weeks until brace d/c |
Weeks
1, 2, 3, then every 2-3 weeks |
Displaced
fractures and fractures with |
|
|
|
|
|
Hinged
knee brace at full ext. for 2 weeks (NWB). Then gradual passive flexion to
90° by 4 weeks. Total immobilization 8-12 weeks |
|
|
|
|
|
|
Ottawa
Knee rules > 55 years of age, fibula head tenderness, isolated patella
tenderness, inability to flex > 90° or bear weight for 4 steps |
|
|
|
|
|
|
|
|
|
|
|
|
|
All
medial condyle fractures, types V & VI. |
|
Tibial spine |
Standard
knee + tunnel view |
Suspect
ACL rupture |
Straight-leg
knee immobilizer |
Full-length
cast with 10°-15° flexion for 4-6 weeks. |
Week
1 and then every 3-4 weeks. |
After
reduction, week 1 then week 4-6 |
Displaced
or irreducible fracture; all type 3 and ACL ruptures. |
|
|
|
|
Arthrocentesis
for pain control |
|
|
|
|
|
Tibial tuberosity |
Lateral
knee |
Type
2 extends to physis; type 3 extends to joint |
Check
extension mechanism |
Full-length
cast at 0° for 6 weeks |
Week
1 then every 3-4 weeks |
After
reduction, then week 1 and week 4-6 |
Displacement
|
|
|
|
|
|
|
|
|
Types
2 and 3 |
|
AP = anterior-posterior; NWB =
non-weight bearing; RICE = rest, ice, compression, elevation; d/c =
discontinued. |
|||||||
|
TABLE 7 -- Fracture Management Summary: Ankle |
|||||||
|
Fracture Type |
Radiographic View |
Landmarks |
Acute Treatment Maxims |
Definitive Treatment |
Follow-up |
Repeat Radiographs |
Referral |
|
Tibia shaft |
AP
and lateral lower leg |
Location,
configuration, displacement, angulation, length, rotation, associated
injuries |
Compartment
syndrome 20% |
Plaster
cast (0°-5°) for 4 weeks. Gradual weight bearing to full by 2 weeks. Then
short leg walking brace until clinical and radiographic healing. |
After
acute swelling for casting, then weekly for 4 weeks, then every 2-3 weeks. |
Weeks
1, 2, 3, and 4 and then every 2-3 weeks |
All
high-energy fractures. Combined tibiafibula |
|
|
|
|
Full-length
posterior splint or stirrup splint |
|
|
|
|
|
|
|
|
|
|
|
|
Should
refer unless experienced in long leg casting. |
|
Fibula |
AP
and lateral |
Proximal
fibular fractures indicate knee instability until proven other-wise. Check
peroneal nerve. |
Knee
immobilizer or hinged knee brace locked in extension (small avulsion
fracture). NWB acutely |
Short
leg walking cast or cast walking boot for nondisplaced midshaft fracture, 4-6
weeks. Advance weight bearing as tolerated. |
Acutely
3-4 days, then every 3-4 weeks until healed |
To
confirm fracture healing 4-6 weeks |
Significant
displacement, comminution, peroneal nerve involvement, or unstable knee |
|
Ankle |
AP,
lateral, and mortise view (Include 3 views of foot if midfoot pain or fifth
metatarsal pain) |
AP:
tibiofibular overlap |
Ottawa
Ankle Rule: Inability to bear weight, malleolus tenderness (posterior edge to
6 cm proximal), bone tender-ness of navicular, fifth metatarsal, or midfoot
pain |
Weber
Type A: Acute: posterior or stirrup splint. |
Casting
3-5 days after acute injury |
Assess
fracture healing at 4 weeks |
Displacement
greater than 2 mm or unstable Danis-Weber type B or C fractures trimalleolar
and bimalleolar fractures |
|
|
|
Mortise:
medial clear space <4 mm, tibiofibular overlap 14; |
|
|
Evaluate
healing at 4-6 weeks |
|
|
|
|
|
|
|
Short-leg
walking cast or walking fracture boot for 4-6 weeks |
|
|
|
|
Talus |
AP,
mortise, lateral ankle, and 45° internal oblique |
Talar
neck injuries are at risk for AVN; therefore CT scan for suspected injury |
5
most commonly missed ankle fractures: |
Lateral
Process Avulsion ( |
In
2-4 weeks |
4
weeks |
All
displaced fractures with >3 mm or |
|
|
|
|
Fifth
metatarsal |
|
|
|
|
|
|
|
|
Lateral
process talus |
|
|
|
All
talar neck fractures unless experienced |
|
|
|
|
Os
trigone |
|
|
|
|
|
|
|
|
Anterior
process calcaeus |
|
|
|
|
|
|
|
|
Talar
dome |
|
|
|
|
|
AP = anterior-posterior; ACL = anterior
cruciate ligament; ORIF = open reduction with internal fixation; NWB =
non-weight bearing. |
|||||||
|
TABLE 8 -- Fracture Management Summary: Foot |
|||||||
|
Fracture Type |
Radiograpic View |
Landmarks |
Acute Treatment Maxims |
Definitive Treatment |
Follow-up |
Repeat Radiographs |
Referral |
|
Calcaneous |
AP
and lateral foot, axial projection |
Bohler's
angle (20°-40°) |
Elevation,
ice, compression, and NWB to prevent fracture blisters |
Anterior
process: Small avulsion fracture with minimal displace-ment-use walking cast
boot for 2-4 weeks |
2-4
weeks |
4
weeks |
Displaced
fractures, subtalar joint involvement, delayed union or nonunion |
|
|
|
Less
than 20° suggests fracture |
|
|
|
|
|
|
Midfoot |
AP,
lateral, and internal oblique |
AP
view: second and third metatarsal aligns with medial and lateral second and
third cuneiforms |
Posterior
splint acutely and NWB |
Dorsal
avulsion fracture of the navicular (< 20% of joint) |
2-4
weeks |
4
weeks |
Displacement,
nonunion or delayed union |
|
|
CT
scan for navicular body fractures |
|
Watch
for compartment syndrome with crush injuries. |
|
|
|
|
|
|
|
|
|
Cast
walking boot for 4-6 weeks |
|
|
|
|
|
|
Oblique
view: fourth medial metatarsal aligns with medial edge of cuboid |
|
|
|
|
|
|
First Metatarsal |
AP,
lateral oblique foot and coned down view for first metatarsal |
No
dorsal or sagittal angulation |
Posterior
splint and RICE |
Non-weight
bearing short leg cast for 2-3 weeks. Postoperative wooden shoe for comfort
for 2-3 weeks |
2-3
weeks |
4
weeks |
Intra-articular
or displaced |
|
Second- Fourth Metatarsal |
AP,
lateral and oblique foot |
Frontal
plane displacement is OK. Dorsal or Sagittal displacement refers |
RICE
therapy and posterior splint 2-4 days |
Wooden
post-operative shoe, cast walking boot, or short leg cast for 2-3 weeks if
significant pain |
2-3
weeks |
4
weeks |
Displacement
greater than 10° in the dorsal or sagittal plane, intra-articular, or
multiple |
|
Fifth Metatarsal |
AP,
lateral and oblique foot |
Apophysis
= long axis Tuberosity = transverse Jones = Metaphysis/shaft |
Weight
bearing as tolerated |
Nondisplaced
tuberosity Fracture: postoperative wooden shoe 2-4 weeks |
2-4
weeks |
4
weeks |
Jone's
fractures, displaced tuberosity fracture > 3 mm |
|
AP = anterior-posterior; NWB =
non-weight bearing; RICE = rest, ice, compression, elevation. |
|||||||
|
Key Points
|
References
1.
Alonso JE, Lee J, Burgess AR, et al: The management of complex
orthopedic injuries. Surg Clin North Am 76:879-902, 1996
Full Text
2.
Bach BR: Acute knee injuries. The Physician and Sports-medicine
25:39-50, 1997
3.
Baxter DE: The Foot and Ankle in Sport. St. Louis, Mosby, 1995
4.
Beaty JH, Kumar A: Current concepts review. Fractures about the
knee in children. J Bone Joint Surg (Am) 76A:1870-1880, 1994
Citation
5.
Bone LB, Sucato D, Stegemann PM: Displaced isolated fractures of
the tibial shaft treated with either a cast or intramedullary nailing. An outcome
analysis of matched pairs of patients. J Bone Joint Surg (Am) 79A:1336, 1997
Abstract
6.
Brand DA, Frazier WH, Kohlhepp WC, et al: A protocol for selecting
patients with injured extremities who need x-rays. N Engl J Med 306:833-339,
1982
Abstract
7.
Burroughs KE, Reimer CD, Fields KB: Lisfranc injury of the foot: A
commonly missed diagnosis. Am Fam Physician 58:118-124, 1998
Abstract
8.
Canale ST: Campbell's Operative Orthopaedics, ed: 9. St. Louis,
Mosby, 1998
9.
Carpenter JE, Kasman R, Matthews LS: AAOS instructional course
lectures, fractures of the patelia. J Bone Joint Surg (Am) 75A:1550-1561, 1993
10.
Clanton TO, Porter DA: Primary care of foot and ankle injuries in
the athlete. Clin Sports Med 16:435-466, 1997
Full Text
11.
Eiff PM, Hatch RL, Walter CL: Fracture Management for Primary
Care. Philadelphia, WB Saunders, 1998
12.
Gaston P, Will E, Elton A: Fractures of the tibia, can their
outcome be predicted. J Bone Joint Surg (Br) 81B:71-76, 1999
Abstract
13.
Giachino AA, Uhthoff HK: Intra-articular fractures of the
calcaneus. J Bone Joint Surg (Am), 71A:784-787, 1989
Citation
14.
Greenspan A: Orthopedic Radiology, ed 2. New York, Raven Press,
1992
15.
Hughston JC, Whatley GS, Bearden JM: Tibia fractures. South Med J
62:931-940, 1969
Citation
16.
Jensen DB, Rude C, Bjerg-Nielsen A: Tibial plateau fractures. J
Bone Joint Surg (Br) 72B:49-52, 1990
Abstract
17.
Kaufman D, Leung J: Evaluation of the patient with extremity
trauma: An evidence based approach. Emerg Med Clin North Am 17:77-95, 1999
Full Text
18.
Kitaoka HB, Chao EJ, Edumund YS: Displaced intra-articular
fractures of the calcaneus treated non-operatively. J Bone Joint Surg (Am)
76A:1531-1540, 1994
Abstract
19.
Leddy JJ, Smolinski RJ, Lawrence J, et al: Prospective evaluation
of the Ottawa Ankle Rules in a university sports medicine center. Am J Sports
Med 26:158-165, 1998
Full Text
20.
Littenberg QB, Swiontkowski MF, Rudicel SA: Closed fractures of
the tibial shaft. A meta-analysis of three methods of treatment: J Bone Joint
Surg (Am) 80A:174-183, 1998
Abstract
21.
Marder RA: AAOS instructional course lectures: Current methods for
the evaluation of ankle ligament injuries. J Bone Joint Surg (Am)
76A:1103-1111, 1994
22.
Markert RJ, Walley ME, Guttman TG, et al: A pooled analysis of the
Ottawa Ankle Rules used on adults in the ED. Am J Emerg Med 16:564-567, 1998
Full Text
23.
Meredith RM, Butcher JD: Field splinting of suspected fractures.
The Physician and Sportsmedicine 25:29-39, 1997
24.
Michelson JD: Current concepts review: Fractures about the ankle.
J Bone Joint Surg (Am) 77A:142-150, 1995
25.
O'Shea KJ, Murphy KP, Heekin DR, et al: The diagnostic accuracy of
history, physical examination, and radiographs in the evaluation of traumatic
knee disorders. Am J Sports Med 24:164-168, 1996
Full Text
26.
Olson SA: AAOS instruction course lectures: Open fractures of the
tibial shaft. J Bone Joint Surg (Am) 78A:1428-1435, 1996
28.
Rockwood & Green's Fractures in Adults, ed 4. Philadelphia,
Lippincott-Raven, 1996
29.
Sarmiento A: Functional bracing of tibial fractures. Clin Orthop
105:202-219, 1974
Citation
30.
Schwartz DT, Reisdorff E: Emergency Radiology. New York,
McGraw-Hill, 1999
31.
Seaberg DC, Yealy DM, Lukens T, et al: Multicenter comparison of
two clinical decision rules for the use of radiography in acute, high-risk knee
injuries. Ann Emeg Med 32: 8-13,1998
32.
Simon RR, Koenigsknecht S: Emergency Orthopedics. Norwalk, CT,
Appleton and Lange, 1995
33.
Steill, IG, Greenberg GH, Wells GA, et al: Prospective validation
of a decision rule for the use of radiography in acute knee injuries. JAMA
275:611-615, 1996
Abstract
34.
Stiell IG, Wells GA, Hoag RH, et al: Implementation of the Ottawa
Knee Rule for the use of radiography in acute knee Injuries. JAMA
278:2075-2079, 1997
Abstract
35.
Steinberg GG, Akins CM, Baran DT: Orthopaedics in Primary Care, ed
3. Philadelphia, Lippincott Williams & Wilkins, 1998
36.
Tandeter HB, Shvartzman P: Acute ankle injuries: Clinical decision
rules for radiographs. Am Family Physcian 55:2721-2728, 1997
37.
Thordarson DB: Detecting and treating common foot and ankle fractures,
part I. The Physician and Sportsmedicine 24:29-38, 1996
38.
Thordarson DB: Detecting and treating common foot and ankle
fractures, part II. The Physician and sportsmedicine 24:58-64, 1996
39.
Vander GR, Michelson JD, Bone LB: AAOS instructional course
lectures, fractures of the ankle and the distal part to the tibia. J Bone Joint
Surg (Am) 78A:1772-1783, 1996
Abstract
40.
Watson JT: Current concepts review: Treatment of unstable
fractures of the shaft of the tibia. J. Bone Joint Surg (Am) 76A:1575-1583,
1994
41.
Wedmore IS, Charette J: Emergency department evaluation and
treatment of ankle and foot injuries. Emerg Med Clin North Am 18:85-113, 2000
Full Text
42.
Wyrsch B, McFerran MA: McAndrew M. Operative treatment of
fractures of the tibial plafond. A randomized, prospective study. J Bone Joint
Surg (Am) 78A:1646, 1996
Abstract
Edward E.
Rylander, M.D.
Diplomat American
Board of Family Practice.
Diplomat American
Board of Palliative Medicine.