BMJ 2002;324:91
( 12 January )
Primary care
Reducing antibiotic use for acute bronchitis in primary
care: blinded, randomised controlled trial of patient information leaflet
John Macfarlane
a Respiratory Medicine, Nottingham
City Hospital NG5 1PB, b Sherrington Park Medical Practice,
Nottingham NG5 2EJ, c Arnold Health Centre, Arnold, Nottingham
NG5 7BP, d Stenhouse Medical Centre, Arnold, Nottingham NG5
7BP, e Respiratory Infection Research Group, Nottingham City
Hospital, f University of Nottingham, Clinical Sciences
Building, Nottingham City Hospital
Correspondence to: J Macfarlane [log in to unmask]
|
|
Abstract |
Objective: To assess whether sharing the
uncertainty of the value of antibiotics for acute bronchitis in the
form of written and verbal advice affects the likelihood of patients
taking antibiotics.
Design: Nested, single blind,
randomised controlled trial.
Setting: Three suburban general
practices in Nottingham
Participants: 259 previously well
adults presenting with acute bronchitis.
Intervention: In group A,
212 patients were judged by their general practitioner not to
need antibiotics that day but were given a prescription to use if
they got worse and standard verbal reassurance. Half of them (106)
were also given an information leaflet. All patients in group B (47)
were judged to need antibiotics and were given a prescription and
encouraged to use it.
Main outcome measures: Antibiotic
use in the next two weeks. Reconsultation for the same symptoms in
the next month.
Results: In group A fewer patients
who received the information leaflet took antibiotics compared with
those who did not receive the leaflet (49 v 63, risk ratio 0.76, 95%
confidence interval 0.59 to 0.97, P=0.04). Numbers
reconsulting were similar (11 v
14). In group B, 44 patients took the antibiotics.
Conclusion: Most previously well
adults with acute bronchitis were judged not to need antibiotics.
Reassuring these patients and sharing the uncertainty about
prescribing in a information leaflet supported by verbal advice is a
safe strategy and reduces antibiotic use.
|
What is already known on this topic For most patients antibiotics do not modify the natural
course of the symptoms The widespread belief among patients that infection is
the problem and antibiotics the solution has considerable influence on
prescribing by general practitioners, even when they judge that antibiotics
are not definitely indicated What this study adds Antibiotic use was reduced by a quarter in such patients,
who received verbal and written information and reassurance in addition to a
prescription for antibiotics Sharing with the patient the uncertainty about the
decision to prescribe seems safe and effective |
|
|
Introduction |
Acute bronchitis is a common condition that results in nearly
2 million consultations in England and Wales each year. 1 2 General
practitioners prescribe antibiotics in three quarters of such
consultations, even though there is little evidence to justify it. 2 3 The
widespread belief among patients with acute bronchitis that
infection is the problem and antibiotics the solution has
considerable influence on prescribing of antibiotics by general
practitioners, even when their clinical judgment is that antibiotics
are not definitely indicated.3-5 This is
a factor in the overuse of antibiotics and the increasing prevalence
of drug resistance, adverse effects, and cost.6
As a major reason for the use of antibiotics in acute bronchitis
seems to be the expectations of patients, we conducted a randomised,
controlled, clinical trail to determine the impact of a patient
information leaflet on the use of antibiotics in patients with this
condition.
|
|
Methods |
Recruitment and initial assessment of
participants
Participants for the trial were recruited from three general practices
in Nottingham familiar with research in this topic. 3 4 7-9 Between
September 1999 and August 2000 (excluding a month over
Christmas and the millennium period), we recruited consecutive
adults presenting with "acute bronchitis," defined as a
"new, acute lower respiratory tract illness in a previously
well adult," using previously reported definitions (box 1). 4 8-11
|
The study was approved by the Nottingham City
Hospital ethics committee, and all participants provided written consent.
Each general practitioner managed the patients according to their
usual clinical practice and based on their clinical judgment divided
them into two groups: group A, in which antibiotics were not
definitely indicated that day, and group B, in which antibiotics were
definitely indicated that day. This decision was made without additional
guidance or investigations.
Antibiotic prescriptions and randomisation
All patients were given a prescription for an antibiotic, the choice
of which was left to the general practitioner, and a sealed envelope
containing a two week diary card with instructions, pen, and a
stamped, addressed return envelope. Patients in group B were advised
to take the antibiotics.
|
For all patients in group A the general
practitioner provided verbal information based on a prompt card (box 2). These patients
were then randomised by using permuted blocks of four to receive or
not receive a patient information leaflet about the natural course
of lower respiratory tract symptoms and the advantages and
disadvantages of antibiotic use (fig 1). The patient
information leaflet was in the sealed envelope, blinded from the
general practitioner by means of a blank leaflet, together with the
diary card and return envelope. Patients were asked to open and read
the contents of the envelope after the consultation.
|
End points and follow up
The primary end point was whether the patient took the antibiotics
they had been prescribed. This information was obtained from the
symptom diary, which included a space to record daily antibiotic
use, and by telephone contact. Patients were contacted by telephone
at around one week and two weeks after the consultation by research
assistants blinded to the grouping of the patients. Answers to
structured questions regarding antibiotic use were recorded.
The secondary outcome was whether patients initiated a further
consultation for the same symptoms within the next month. Patients were
not asked to return routinely by the general practitioner. We have
previously reported that reconsultation is an easily measured and
consistent end point for acute bronchitis and relates to persistent cough
and patient dissatisfaction with their progress. 8 9 11 12
We carried out a pilot study of 33 consecutive patients with
acute bronchitis to develop consistency of data collection by the
general practitioners and telephone follow up by the research assistants.
Statistical analysis
Our primary hypothesis was that the proportion of patients in group
A who would take antibiotics during the two week follow up period
would be lower in those who received the leaflet than in those in
the control group. We calculated the risk ratio and 95% confidence interval
using EpiInfo and used a ![]() 2 test with Yates's correction for the hypothesis test.
Using these data we calculated the number need to treat as the
reciprocal of the absolute difference in antibiotic uptake between
the two groups.
2 test with Yates's correction for the hypothesis test.
Using these data we calculated the number need to treat as the
reciprocal of the absolute difference in antibiotic uptake between
the two groups.
To calculate sample size we set a minimum difference of 20% in
primary outcome between the two intervention arms in group A and a
discriminatory power of 80%. The required number in group A was
206.
To look for possible confounding by age, sex, surgery, smoking
status, description of cough, duration of cough, and the presence of
chest signs we used a series of bivariate logistic regression models
within Stata (version 5). We also examined whether the impact of the
leaflet on antibiotic uptake was modified by any of these variables
by fitting a series of multiplicative interaction terms and
comparing the nested models using the likelihood ratio test.
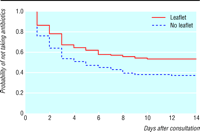
We constructed a Kaplan-Meier plot from the days between
consultation and the day antibiotics were started and calculated the
rate ratio using a Cox regression model within Stata. We tested the
proportional hazard assumption of this model using the diagnostic section
within Stata (ph1test).
|
|
Results |
Participants
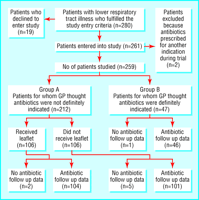
During the study, the general practitioners saw 280 patients
with acute bronchitis, 259 of whom agreed to participate in the
study (table, fig 2).
Of the 212 patients in group A, 106 received the patient
information leaflet and 106 did not. Among patients who were
given the leaflet, two were lost to follow up, and 49 (47%)
took their antibiotics. For patients in the control group five were
lost to follow up, and 63 (62%) took their antibiotics (risk
ratio 0.76, 95% confidence interval 0.59 to
0.97, P=0.04; number needed to treat 6.7).
|
|
Within the logistic regression model we found no
evidence of confounding by age, sex, smoking status, whether patients paid
for their prescriptions, description of cough or sputum, duration of
cough, presence of chest signs, or general practice. In addition there
was no evidence of significant effect modification by any of these
variables.
Figure 3
shows the Kaplan-Meier plot. The rate ratio for the intervention group compared
with the control group was 0.66 (0.46 to 0.96). The
reconsultation rates were similar for all patients in group A
(table). For the 47 patients in group B (20% of all patients),
all of whom were told by their doctor that antibiotics were
definitely indicated, 44 (94%) took their antibiotics.
|
|
|
Discussion |
Use of antibiotics by patients with acute bronchitis can be
reduced by providing patients with a simple information leaflet about
the use of antibiotics and the natural course of acute bronchitis and
giving reassurance after a consultation and examination that their
condition is not serious. The use of the patient information leaflet
reduced the use of antibiotics by nearly a quarter. If these results
are extrapolated to national figures, about 750 000 fewer courses of
antibiotics could be prescribed each year.
This may underestimate the true efficacy of the leaflet as all
patients were also reassured verbally by their general practitioner that
antibiotics were not definitely indicated at the time of the consultation.
The effect of the leaflet was seen not only at the time of the
consultation but continued over the following two weeks of
observation. By contrast, when the general practitioner recommended
that antibiotics were definitely indicated, nearly all patients said
they did take them, emphasising the strong influence of doctors'
advice on patient compliance.
Prescribing and management strategies for
acute bronchitis
Most episodes of acute bronchitis resolve on their own, and how to
identify those few patients who may benefit from antibiotics is not
clear. 2 13
Prescribing antibiotics for patients with such self limiting conditions
can be counterproductive as it reinforces the belief that
antibiotics are beneficial and encourages future consultations. 10 13
Providing patients with information and using a delayed
prescription have been advanced by the National Prescribing Centre of
the NHS13
and the Standing Medical Advisory Committee of the Departments of
Health14
as strategies for reducing antibiotic use in the community. Open
studies of managing uncomplicated respiratory infection in adults15 and sore
throat and otitis media in children in primary care16-18 have
shown that such strategies result in fewer people taking
antibiotics. Our study supports this approach for adults with acute
bronchitis. There are nearly three million consultations for acute
bronchitis annually in England and Wales1 and
an incidence of up to 70 per 1000 for a practice population of
previously well adults.8
Reducing antibiotic use by a quarter would substantially influence
antibiotic use in the community, as currently up to three quarters
of UK adults who consult with acute bronchitis receive antibiotics,
and the figures are even higher in some other European countries.10-13
Further studies could assess whether reassurance and sharing
information and prescribing decisions would lead to longer term benefits
for individuals and the community in terms of less dependence on
antibiotics. 10
13 19 Little
et al showed that prescribing antibiotics for sore throat and otitis
media increased the likelihood of consultations during future
episodes. 18
20 For
acute bronchitis, we have shown that pressures at home and work and
concerns about the seriousness of the problem are also associated
with the likelihood of seeking medical attention.21
The strategy of verbal and written information seems practical and
safe. The leaflet was cheap and simple to produce, and the study was
conducted during normal consultations by general practitioners. Most
patients seemed happy with the approach. Few declined to take part
in the study or expressed concern about sharing the prescribing
decision with their doctor. Rates of reconsultation were no higher
in the leaflet group, and no patients required referral to hospital
for respiratory illness during follow up. A similar study on
management of acute cough also showed that an information leaflet
led to fewer future consultations for minor coughs and no delays in
consultations for more serious respiratory symptoms.19 We
developed our leaflet from one we used successfully to reduce
reconsultation rates in a previous study of acute bronchitis (that
is, acute lower respiratory tract illness in a previously well
adult).9
Our results support the development of a more robust study in which
no prescription would be offered.
Study weaknesses
We did not measure antibiotic use directly, a problem shared with
other studies.15-18
We have previously reported on a simple technique using a bioassay
on urine to check whether patients in the community are using their
prescriptions for antibiotics.22 However,
in the current study we could not devise a method of collecting
urine from the patients in an informed manner without compromising
our objectives. We considered leaving the filled out prescription
with the practice receptionist and recording the number collected, a
method used in previous studies. 15 16 18 However,
this does not record antibiotic consumption and is more inconvenient
for both the patient and the practice than our approach. Arguably,
it is also less representative of typical practice and can lead to
patients with acute cough feeling dissatisfied and less empowered.15
Our practices were used to doing research in this topic, which may
make the doctors and patients unrepresentative. This may have
encouraged the general practitioners to include more patients in the
group thought not to need antibiotics and hence provide a sterner
test of the information strategy we used.
How this study helps general practitioners
Of course some patients with an acute lower respiratory tract
illness do benefit from antibiotics.23 In our
study nearly one in five patients were thought to need antibiotics, a
figure consistent with that found in previous studies.10 Further
research would identify those patients most likely to benefit from
antibiotics.2
We have shown that investigating patients for infection either at
first presentation or when they reconsult is not a useful strategy
for better targeting of antibiotic treatment. 7 8 For the
many patients (around 80%) for whom the general practitioner thinks
that antibiotics are not definitely indicated, we have shown that
sharing uncertainty about prescribing openly and honestly with the
patient is safe and effective and also reduces antibiotic use.
|
|
Acknowledgments |
We thank the general practitioners who
participated in the study: Gina Bajek, Stephen Bolsher, Anne Cockburn, Fiona
Coutts, Mike Elliott, Andrew Flewitt, Phil Gard, Brian Hammersley,
Bill Holmes, Richard Howard, Christine Leiper, Elaine Maddock, Fiona
McCracken, Suresh Patel, Peter Pavier, Kathy Scahill, David Thornhill,
and P Wilson. We also thank the practice staff, in particular Dawn
Hill, Jill Moon, and Karen Glover who coordinated the study in each
practice, Susan Allen and Tracy Broadhurst for performing the
patient telephone follow up, and Jennie Etches for help with data
entry.
Contributors: JM had the original idea for the study and all
authors were involved in the design and planning. RM coordinated the study
logistics throughout and WH, PG, and DT liaised with their colleagues and staff
in the three practices and monitored reconsultations. RM and RH performed the
data analysis. The paper was written by JM, who acts as guarantor (with RH as
guarantor for data analysis), with input from all authors.
|
|
Footnotes |
Funding: British Lung Foundation.
Competing interests: JM has received consultancy fees from Pfizer,
Abbott, Hoechst Marion Roussel, Trinity, Glaxo Wellcome; research
funding from Hoechst Marion Roussel, Rhone Poulenc Rorer, and Bayer;
lecture fees from AstraZeneca, Hoechst Marion Roussel, and Pfizer;
and support for attending conferences from Astra, Pfizer, Allen and
Hanbury, and 3M. WH has received consultancy fees from Glaxo
Wellcome, Schering Plough, Boehringer Ingleheim, Hoechst Marion
Roussel, Astra, 3M, Zeneca, and Rhone Poulenc Rorer; research
funding from 3M and Rhone Poulenc Rorer; and support for attending
conferences or courses from Glaxo Wellcome, Schering Plough, Zeneca,
and 3M. RH received support from Bayer for attending two scientific
meetings and to support a research project.
|
|
References |
|
1. |
Office of Population Censuses and
Surveys. Morbidity statistics from general
practice: fourth national study 1991-1992. London: HMSO, 1995
(series MB 5;3). |
|
2. |
Arroll B, Kenealy T. Antibiotics for
acute bronchitis. BMJ 2001;
322: 939-940 |
|
3. |
Macfarlane JT, Lewis SA, Macfarlane RM,
Holmes WF, et al. Contemporary use of antibiotics in 1089 adults
presenting with acute lower respiratory tract illness in general practice in
the UK: implications for developing management guidelines. Respir Med 1997; 91: 427-434 |
|
4. |
Macfarlane J, Holmes, Macfarlane R,
Britten N. Influence of patients' expectations on antibiotic management of
acute lower respiratory tract illness in general practice: questionnaire
study. BMJ 1997; 315: 1211-1214 |
|
5. |
Cockburn J, Pit S. Prescribing behaviour
in clinical practice: patients' expectations and doctors' perceptions of
patients' expectations |
|
6. |
Audit Commission. A prescription for improvement. Towards more rational
prescribing in general practice. London: HMSO, 1994. |
|
7. |
Macfarlane J, Prewett J, Rose D, Gard P,
Guion A, Cunningham R, et al. Prospective, case-control study of the role of
infection in patients who reconsult after initial antibiotic treatment for
lower respiratory tract infection in primary care. BMJ 1997; 315: 1206-1210 |
|
8. |
Macfarlane J, Holmes W, Gard P,
Macfarlane R, Rose D, Weston V, et al. Prospective study of the incidence,
aetiology and outcome of lower respiratory tract illness in the community. Thorax 2001; 56: 109-114 |
|
9. |
Macfarlane JT, Holmes WF, Macfarlane RM.
Reducing reconsulations for acute lower respiratory tract illness with an
information leaflet: a randomized controlled study of patients in primary
care. Br J Gen Pract 1997; 47:
719-722 |
|
10. |
Macfarlane J, Holmes WF, Macfarlane R.
Do hospital physicians have a role in reducing antibiotic prescribing in the
community? Thorax 2000; 55:
153-158 |
|
11. |
Holmes WF, Macfarlane JT, Macfarlane RM,
Hubbard R. Symptoms, signs, and prescribing for acute lower respiratory tract
illness. Br J Gen Pract 2001;
51: 177-181 |
|
12. |
Holmes WF, Macfarlane JT, Macfarlane RM,
Lewis S. The influence of antibiotics and other factors on reconsultation for
acute lower respiratory tract illness in primary care. Br J Gen Pract 1997; 47: 815-818 |
|
13. |
Anon. Antibiotic prescribing: a
challenge for primary care. MeReC Bulletin
2000; 11: 1-4 |
|
14. |
Standing Medical Advisory Committee.
Subgroup on Antimicrobial Resistance. The
path to least resistance. London: Department of Health, 1988. |
|
15. |
Dowell J, Pitkethly M, Bain J, Martin S.
A randomised controlled trial of delayed prescribing as a strategy for
managing uncomplicated respiratory tract infection in primary care. Br J Gen Pract 2001; 51: 200-205 |
|
16. |
Little P, Williamson I, Warner G, Gould
C, Gantley M, Kinmonth AL. Open randomised trial of prescribing strategies in
managing sore throat. BMJ 1997;
314: 722-727 |
|
17. |
Cates C. An evidence based approach to
reducing antibiotic use in children with acute otitis media: controlled
before and after study. BMJ
1999; 318: 715-716 |
|
18. |
Little P, Gould C, Williamson I, Moore
M, Warner G, Dunleavey J. Pragmatic randomised controlled trial of two
prescribing strategies for childhood acute otitis media. BMJ 2001; 322: 336-342 |
|
19. |
Rutten G, Van Eijk J, Beek M, Van der
Velden H. Patient education about cough: effect on the consulting behaviour
of general practice patients. Br J Gen
Pract 1991; 41: 289-292 |
|
20. |
Little P, Gould C, Williamson I, Warner
G, Gantley M, Kinmonth AL. Reattendance and complications in a randomised
trail of prescribing strategies for sore throat: the medicalising effect of
prescribing antibiotics. BMJ
1997; 315: 350-352 |
|
21. |
Holmes WF, Macfarlane RM, Macfarlane JT.
Why do patients attend their physician with lower respiratory tract illness
and what do they think of their treatment and infection? Am J Resp Crit Care Med 1998; 157: A500 |
|
22. |
Lim WS, Garner S, Finch RG, Macfarlane
JT. A novel method for collecting and detecting amoxycillin in urine: a tool
for testing antibiotic compliance in the community. J Antimicrob Chemother 2000; 46: 835-837 |
|
23. |
Gonzales R, Sande M. What will it take
to stop physicians from prescribing antibiotics in acute bronchitis? Lancet 1995; 345: 665-666 |
(Accepted 20 September 2001)
Commentary: More self reliance
in patients and fewer antibiotics: still room for improvement
Chris van Weel
Department of General Practice, University Medical Centre St
Radboud, Nijmegen, Netherlands
The study of Macfarlane et al examines the old problem of
overprescribing of antibiotics, but it approaches the problem in a
highly original way. To what extent can their findings be applied to
routine care in general practice.
Firstly the reduction of antibiotic use. The empirical findings of
acute bronchitis in general practice can in all probability be
generalised: many prescriptions for antibiotics are given for episodes
of illness that usually are self limiting. Use of antibiotics under
these circumstances is often spurious and does not contribute to
patients' wellbeing. Undue use of antibiotics may at the same time
contribute to the growing concerns about resistance. These are sound
professional arguments for the restriction of prescribing.
But patients influence prescribing, and there is a strong
perception among practitioners![]() whether true or
not
whether true or
not![]() that patients
in general value a prescription for antibiotics. Macfarlane et al
focused their intervention on the interaction between professional opinion
and patients' values. The intervention of inviting patients not to use
the prescribed antibiotics is something most general practitioners
do most days. They offer reassurance and encouragement to the
patient to await the natural, benign course of an infection, without
removing the possibility of antibiotic treatment. The advantages are
obvious. The procedure takes away the power struggle between the
patient and the general practitioner, who is in charge of
prescribing, and focuses the patient's decision on the content of
the advice. This paper shows that general practitioners can distinguish
between those in need of antibiotic treatment and those who can do
without it and can substantially reduce the reliance on antibiotics.
But it is important to note that about half of the patients still
used the antibiotics that their general practitioner thought they
could do without. So there is substantial room for improvement.
that patients
in general value a prescription for antibiotics. Macfarlane et al
focused their intervention on the interaction between professional opinion
and patients' values. The intervention of inviting patients not to use
the prescribed antibiotics is something most general practitioners
do most days. They offer reassurance and encouragement to the
patient to await the natural, benign course of an infection, without
removing the possibility of antibiotic treatment. The advantages are
obvious. The procedure takes away the power struggle between the
patient and the general practitioner, who is in charge of
prescribing, and focuses the patient's decision on the content of
the advice. This paper shows that general practitioners can distinguish
between those in need of antibiotic treatment and those who can do
without it and can substantially reduce the reliance on antibiotics.
But it is important to note that about half of the patients still
used the antibiotics that their general practitioner thought they
could do without. So there is substantial room for improvement.
One problem with the authors' intervention is the message it gives
to the patients, and here the approach used may not be as easy to
transfer to routine care. The explicit message ("antibiotics are
not required") was accompanied by the handing out of a prescription that
implied a totally different message. This inconsistency may trigger
doubt and lack of confidence in the proposed self reliance, particularly
in patients who value medical as opposed to self treatment and
prefer external powers to deal with their problems. This group is
particularly at risk of medicalisation, including repeated
prescriptions of for unnecessary antibiotics for self limiting infections.
The medical setting is not a harmless placebo and can have
positive and negative effects. Macfarlane et al should be complimented on
their way of bringing this setting into the test of effectiveness. An
obvious alternative way to test their current intervention would be
to examine the patient and give advice to come back in a couple of
days if the predicted wearing off of their symptoms did not occur.
Continuity of care is not a panacea, but I would not be surprised if
it were able to reduce such unnecessary use of antibiotics by more
than half.
Edward E.
Rylander, M.D.
Diplomat American
Board of Family Practice.
Diplomat American
Board of Palliative Medicine.