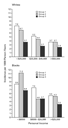|
|
Neighborhood of Residence and Incidence of
Coronary Heart Disease
Ana V. Diez Roux, M.D., Ph.D., Sharon Stein Merkin, M.H.S.,
Donna Arnett, Ph.D., Lloyd Chambless, Ph.D., Mark Massing, M.D., Ph.D., F.
Javier Nieto, M.D., Ph.D., Paul Sorlie, Ph.D., Moyses Szklo, M.D., Dr.P.H.,
Herman A. Tyroler, M.D., and Robert L. Watson, Ph.D.
|
|
ABSTRACT
Background Where a
person lives is not usually thought of as an independent predictor
of his or her health, although physical and social features of
places of residence may affect health and health-related behavior.
Methods Using data
from the Atherosclerosis Risk in Communities Study, we examined the
relation between characteristics of neighborhoods and the incidence
of coronary heart disease. Participants were 45 to 64 years of age
at base line and were sampled from four study sites in the United
States: Forsyth County, North Carolina; Jackson, Mississippi; the
northwestern suburbs of Minneapolis; and Washington County, Maryland.
As proxies for neighborhoods, we used block groups containing an
average of 1000 people, as defined by the U.S. Census. We
constructed a summary score for the socioeconomic environment of
each neighborhood that included information about wealth and income,
education, and occupation.
Results During a
median of 9.1 years of follow-up, 615 coronary events occurred in
13,009 participants. Residents of disadvantaged neighborhoods (those
with lower summary scores) had a higher risk of disease than
residents of advantaged neighborhoods, even after we controlled for
personal income, education, and occupation. Hazard ratios for
coronary heart disease among low-income persons living in the most
disadvantaged neighborhoods, as compared with high-income persons in
the most advantaged neighborhoods, were 3.1 among whites (95 percent
confidence interval, 2.1 to 4.8) and 2.5 among blacks (95 percent
confidence interval, 1.4 to 4.5). These associations remained
unchanged after adjustment for established risk factors for coronary
heart disease.
Conclusions Even after
controlling for personal income, education, and occupation, we found
that living in a disadvantaged neighborhood is associated with an
increased incidence of coronary heart disease.
Today, where a person lives is not usually
thought of as an important predictor of his or her health. Lifestyle
and genetic explanations for the causes of disease predominate.
Nevertheless, the neighborhoods where people live may differ in many
aspects potentially related to health.1,2,3 The
socioeconomic environment of neighborhoods has been shown to be
related to health status and mortality4,5,6,7,8,9 as
well as to health-related behavior such as smoking, dietary habits,
and physical activity.10,11,12,13,14
The relation between the characteristics of a neighborhood and health
outcomes appears to be independent of the socioeconomic position of
individual persons.4,5,6,7,8,9,10,11,12,13,14
This suggests that attributes of neighborhoods themselves may be
important to health.
A variety of characteristics of neighborhoods, including the availability
of resources and services to promote or maintain healthy lifestyles
as well as the physical and social environment, may be related to
cardiovascular risk. Although studies have suggested that
neighborhood characteristics may be related to the prevalence of,
risk factors for, and mortality due to coronary heart disease,8,9,13,14,15
the extent to which neighborhood characteristics are related to the
incidence of coronary heart disease has not been established. We
examined the relation of neighborhood characteristics to the
incidence of coronary heart disease (indicated by the occurrence of
coronary events) among men and women in four diverse regions of the
United States.
Methods
Study Population and Study Variables
The Atherosclerosis Risk in Communities Study is a prospective
investigation of atherosclerosis in four U.S. communities: Forsyth County,
North Carolina; Jackson, Mississippi; the northwestern suburbs of
Minneapolis; and Washington County, Maryland. The cohort was
composed of 15,792 persons 45 to 64 years of age at base line who
were selected by probability sampling.16
Virtually all of the subjects from Washington County and the suburbs
of Minneapolis were white. Eighty-five percent of the subjects from
Forsyth County were white. All of the subjects from Jackson were
black. The base-line examination took place between 1987 and 1989.
Follow-up examinations were carried out every three years, and
participants were contacted annually by telephone between visits to
the clinic.
Participants were linked to their neighborhood of residence by
their home address at base line. Census-block groups, which are subdivisions
of U.S. Census tracts containing an average of 1000 people,17
were used as proxies for neighborhoods. A summary neighborhood score
was used as the main indicator of the socioeconomic environment of
the neighborhood.
The variables used in the construction of the neighborhood score
were selected on the basis of factor analyses of data from census-block
groups. Factor analysis is a statistical technique that can be
used to determine which variables out of a large set (for example,
out of a large set of socioeconomic indicators obtained from the
Census) can be meaningfully combined into a summary score. Six
variables representing the dimensions of wealth and income (log of
the median household income; log of the median value of housing
units; and the percentage of households receiving interest,
dividend, or net rental income), education (the percentage of adults
25 years of age or older who had completed high school and the percentage
of adults 25 years of age or older who had completed college), and
occupation (the percentage of employed persons 16 years of age or
older in executive, managerial, or professional specialty
occupations) were combined into the neighborhood summary score. For
each variable, a z score for each block group was estimated by
subtracting the overall mean (across all block groups in the sample)
and dividing by the standard deviation. The z score reflects the
deviation of the value from the mean. For example, a score of 2.0
for the log of the median household income for a given block group
means that the value for that block group is 2 SD above the overall
mean; a value of –2.0 is 2 SD below the mean. The neighborhood
summary score was constructed by summing the z scores for each of
the six variables. For example, if z scores for the six variables
for a given block group were 1.0, 1.5, 1.8, 2.0, 1.9, and 1.8, then
the neighborhood score for that block group would be 10.0.
Neighborhood scores for block groups in the sample ranged from –11.3
to 14.4, with an increasing score signifying an increasing
neighborhood socioeconomic advantage.
Subjects of each race were divided into three roughly equal groups
according to the summary socioeconomic scores for their neighborhoods.
Neighborhood characteristics for these groups are shown in Table 1. Over 80
percent of the members of the cohort continued to live in the same
block group six years after base line. For those who had moved,
correlations between base-line and follow-up measures of the
neighborhood score and its components were in the range of 0.4 to
0.6.
|
Information on personal income, education, and occupation was obtained
from each member of the cohort during the base-line interview.
Participants selected their total combined family income from eight
categories (under $5,000; $5,000 to $7,999; $8,000 to $11,999;
$12,000 to $15,999; $16,000 to $24,999; $25,000 to $34,999; $35,000
to $49,999; and $50,000 or more). Approximately 6 percent of study
participants did not provide information on income, and their data
were coded as a separate category. The level of education attained
was classified as high school not completed, high school or general
equivalency diploma completed, one to three years of college, four
years of college completed, and some graduate or professional
school. Information on the current or most recent occupation was
collected for employed, unemployed, and retired participants.
Occupations were coded according to the criteria of the 1980 U.S.
Census and categorized according to six occupational groups:
executive, managerial, and professional; technical, sales, and
administrative support; service; farming, forestry, and fishing and
precision production, craft, and repair; operators, fabricators, and
laborers; and homemakers.18
Information on income was updated at the six-year follow-up
examination.
Coronary events were ascertained by contacting participants annually
by telephone, by conducting follow-up examinations, and by surveying
discharge lists from local hospitals and death certificates from
state vital-statistics offices.16,19,20
Data from all hospitalizations were abstracted according to standard
criteria. Death certificates were obtained, and for most deaths that
did not occur in a hospital, additional information was obtained
from the next of kin and from the physician. Coroners' and autopsy
reports, when available, were used for validation.
A coronary event was defined as a validated definite or probable
myocardial infarction for which the patient was hospitalized, a
death due to coronary heart disease, or an unrecognized new myocardial
infarction. The criteria for definite or probable myocardial
infarction were based on combinations of chest pain, electrocardiographic
changes, and levels of cardiac enzymes.19,20
The criteria for definite fatal coronary heart disease were based
on chest pain, the underlying cause of death on the death certificate,
and other associated information from medical records.19,20
Unrecognized new myocardial infarction was defined by the appearance,
between the first and subsequent examinations, of a major Q wave
or a minor Q wave with ischemic ST-T changes or an infarction, as
detected by computerized Novacode21
and confirmed by side-by-side visual comparison of
electrocardiograms. Persons who determined the occurrence of an
event were unaware of the hypothesis being investigated. Events that
occurred through December 31, 1997, were included in these analyses.
The median follow-up was 9.1 years, and the maximal follow-up was
11.1 years.
For each participant, information on cardiovascular risk factors
(smoking status, the level of physical activity, diet, plasma levels
of low-density and high-density lipoprotein cholesterol, the
presence or absence of hypertension, body-mass index [the weight in
kilograms divided by the square of the height in meters], and the
presence or absence of diabetes) was obtained from the base-line
examination as described elsewhere.16
The level of physical activity was summarized in three indexes
corresponding to leisure, sport, and work.22
The dietary intake of saturated fat, polyunsaturated fat, and
cholesterol was summarized with the use of the Keys score.23
Persons were classified as having diabetes if they had fasting
plasma glucose levels of 126 mg per deciliter or more, if they had
nonfasting plasma glucose levels of 200 mg per deciliter or more, or
if they reported having diabetes. Persons were classified as having
hypertension if they had a systolic blood pressure of 140 mm Hg or
more, if they had a diastolic blood pressure of 90 mm Hg or more,
or if they were taking antihypertensive medication. Information on
smoking, blood lipids, body-mass index, hypertension, and diabetes
was also obtained at the three-year and six-year follow-up examinations.
Information on diet and physical activity was updated at the
six-year follow-up examination.
Of the 15,792 participants at base line, 14,158 were linked to
block-group data. Ninety-eight participants who were neither white
nor black or who were black and living in the suburbs of Minneapolis
or in Washington County were excluded, because small numbers made
analyses for these groups unreliable. Fifty-seven participants were
excluded because information on education, information on
occupation, or follow-up information was unavailable. After the
exclusion of 994 participants with preexisting coronary heart
disease (electrocardiographic signs of a previous myocardial infarction
or a history of physician-diagnosed myocardial infarction, coronary
heart surgery, or balloon angioplasty) or unknown disease status at
base line, 13,009 participants in 595 block groups (with a median of
16 participants per block group) were available for analysis.
Adjusted analyses of risk factors at base line were limited to
12,243 participants because of missing data on risk factors. The
study was approved by the institutional review board at each site.
All participants gave written informed consent.
Statistical Analysis
Because of large differences in the distribution of neighborhood
characteristics, analyses were performed separately for blacks in
Jackson and Forsyth County and for whites in Washington County, Forsyth
County, and the suburbs of Minneapolis. Base-line values for
neighborhood characteristics and personal socioeconomic indicators
were compared with the use of linear and logistic regression for
participants in whom coronary heart disease did and did not develop.24
Incidence rates were calculated by dividing the number of events by
the person-years of follow-up within race-specific groups of
participants defined according to the neighborhood score. Incidence
rates were adjusted for age at base line and for study site with the
use of Poisson regression.25
Patterns were consistent across all components of the neighborhood score,
so only results for the summary score are reported. Proportional-hazards regression26
was used to obtain hazard ratios for coronary heart disease
according to the three groups of neighborhood scores after
adjustment for personal indicators of social position (income,
education, and occupation) and after additional adjustment for
cardiovascular risk factors. We performed tests for trend by
introducing neighborhood groups defined according to summary scores
(lowest, intermediate, and highest) as ordinal variables in
regressions.25
The combined effects of neighborhood characteristics and personal
socioeconomic status were examined by estimating incidence rates (and
hazard ratios) for nine cross-classified categories of neighborhood
score and personal income. For these analyses, annual income in each
racial group was categorized as less than $25,000 (25 percent of the
sample), $25,000 to $49,999 (43 percent), and $50,000 or more (32
percent) for whites and as less than $8,000 (26 percent), $8,000 to
$24,999 (43 percent), and $25,000 or more (31 percent) for blacks.
In order to account for potential within-neighborhood correlations
in outcomes, models were run with the use of SUDAAN statistical
software.27
All reported P values are two-tailed.
Results
A total of 615 coronary events occurred during the follow-up period
in the 13,009 participants. Age-adjusted incidence rates of coronary
heart disease were 7.3 per 1000 person-years among white men, 2.8
per 1000 among white women, 8.0 per 1000 among black men, and 4.5
per 1000 among black women. Participants in whom disease developed
were generally more likely to live in disadvantaged neighborhoods
(those with lower summary scores) than those in whom disease did not
develop (Table 2).
Persons in whom coronary disease developed also tended to have lower
levels of income and education and were less likely to have executive,
managerial, or professional occupations than those in whom coronary
disease did not develop (Table 2). All
risk factors investigated, such as smoking and hypertension, were
generally associated with an increased incidence of coronary heart
disease (data not shown).
|
The incidence of coronary heart disease generally decreased with
increasing neighborhood scores (Table 3).
Although associations of the neighborhood score with incidence were
reduced after adjustment for personal socioeconomic indicators (Table 4), differences
between the most disadvantaged and the most advantaged neighborhood
categories remained. Living in the most disadvantaged group of
neighborhoods, as compared with the most advantaged group, was
associated with a 70 to 90 percent higher risk of coronary disease
in whites and a 30 to 50 percent higher risk in blacks.
|
|
Persons living in disadvantaged neighborhoods often had more unfavorable
risk-factor profiles for coronary heart disease than those in more
advantaged neighborhoods (data not shown). However, the differences
were often small (and sometimes absent) after we controlled for
personal socioeconomic indicators (which were also generally
inversely associated with cardiovascular risk-factor levels). We
observed more unfavorable risk profiles in more advantaged
neighborhoods with respect to plasma levels of low-density
lipoprotein and high-density lipoprotein cholesterol in black men
and for the work component of the physical-activity index in white
men in both unadjusted analyses and those that controlled for
personal socioeconomic indicators. The addition of cardiovascular
risk factors to regression models already containing personal
socioeconomic indicators had little effect on the relation between
neighborhood characteristics and the incidence of coronary heart
disease (Table 4).
We obtained similar results when we included risk factors and
personal income as time-dependent covariates (data not shown).
Both neighborhood characteristics and personal income were
independently associated with the incidence of coronary heart
disease (Figure 1).
Overall, in whites, the neighborhood score was inversely associated
with the risk of disease in all categories of personal income, and
income was inversely associated with risk in all three neighborhood
groups. Similar patterns were observed in blacks, but analyses were
limited by small samples. Hazard ratios for coronary events for
low-income persons in the group of neighborhoods with the lowest
scores as compared with high-income persons in the group of
neighborhoods with the highest scores were 3.1 in whites (95 percent
confidence interval, 2.1 to 4.8) and 2.5 in blacks (95 percent
confidence interval, 1.4 to 4.5). These patterns were similar after
adjustment for changes in income between base line and the six-year
follow-up examination (data not shown).
|
Discussion
The relation between the incidence of coronary heart disease and
socioeconomic factors has been documented repeatedly.28
Our findings demonstrate the additional contribution of the neighborhood
of residence to the risk of coronary heart disease. Coronary heart
disease was more likely to develop in persons living in the most
disadvantaged group of neighborhoods than those living in the most
advantaged group, even after we controlled for personal
socioeconomic indicators. We minimized the possibility of residual
confounding by socioeconomic position by simultaneously adjusting
for income, education, and occupation, each divided into multiple
categories.
Previous studies have documented geographic variations in
mortality due to coronary heart disease,29,30,31,32
but the areas examined have often been large. In addition, because
areas rather than individual persons were the units of analysis in
these studies, it is difficult to determine whether geographic
variations are due to differences among the residents of various
areas or to characteristics of the areas themselves. The
availability of Census data linked to personal data allowed us to
examine directly whether the characteristics of smaller areas (akin
to neighborhoods) are related to the risk of disease independently
of the attributes of individual persons.
Neighborhood characteristics could contribute to the development
and persistence of established risk factors. Thus, risk factors may
be thought of as mediators (rather than confounders) of the effects
of neighborhoods. Neighborhoods may differ in the amount of tobacco
advertising33,34
and in the availability and cost of healthful foods.35,36,37
Individual behavior may, in turn, influence the neighborhood, making
both factors mutually reinforcing.38 Differences
among neighborhoods in the physical environment, in the availability
and quality of public spaces and recreational facilities, and in
perceived safety may affect patterns of physical activity.39,40
Social norms may emerge and exert their effects in neighborhoods,
influencing health-related behavior. Living in various types of
neighborhoods may be associated with exposure to sources of chronic
stress (such as noise, violence, and poverty itself) and to sources
of social support, both of which may be linked to the risk of
cardiovascular disease.41,42
We did document some differences (albeit often small) among neighborhoods
in established risk factors for cardiovascular disease after
controlling for personal socioeconomic status. However, additional
adjustment for these risk factors did not substantially alter our
estimates of differences in the incidence of coronary heart disease
among neighborhoods. The failure of risk factors to explain
differences in the risk of cardiovascular disease among
socioeconomic groups is a common finding, even in studies focusing
on traditional measures of personal income, education, and
occupation (which are often strongly associated with risk factors).28
Errors in the measurement of risk factors remain a possibility.
Unaccounted-for interactions between risk factors (or between risk
factors and unmeasured characteristics, such as psychosocial factors
related to neighborhood characteristics) may play a part.
Alternatively, mediating mechanisms that do not involve established
risk factors may be involved. However, the method of investigating
whether a set of factors mediates an observed effect by comparing
estimates before and after adjustment has limitations.43
Therefore, we caution against concluding that the risk factors we
investigated (or the interactions involving these risk factors) do not
mediate any part of the differences among neighborhoods that we
observed. The causal chains involved are likely to be complex.
Effects of neighborhoods were observed in both racial groups,
despite the fact that blacks were drawn from significantly more disadvantaged
neighborhoods than whites — a fact that limited the range of
neighborhood environments that could be examined. In previous
cross-sectional analyses, we documented an unexpectedly low
prevalence of coronary heart disease among black men living in the
most disadvantaged neighborhoods.13
This pattern was not apparent for the incidence of coronary heart
disease, although associations with the neighborhood score were
weaker and less consistent in blacks than in whites. These differences
should be interpreted with caution, given the differences in sample
size and in the range of neighborhood scores (and personal
socioeconomic indicators) investigated in both groups.
Important strengths of our study include its population-based
nature and the availability of detailed and validated information on
coronary outcomes and risk factors. However, nearly 90 percent of
the sample of black subjects was drawn from a single southern city,
which may limit the generalizability of our results to blacks in
other areas. Whites were drawn from three diverse regions, but the
sample did not include persons living in large urban areas. Thus,
our findings need to be confirmed in samples from other geographic
regions. Differences in the geographic areas from which blacks and
whites were drawn also limit the comparisons between races.
Another limitation of our study is the use of block groups as
proxies for neighborhoods. The neighborhood socioeconomic score was
used as an indirect marker of a variety of specific attributes of
neighborhoods that may affect the risk of cardiovascular disease. It
is striking that we observed associations even with these crude
proxies. Changes over time in the neighborhood of residence may have
hampered our ability to estimate the effects of neighborhoods.
However, the areas of residence of the members of our cohort were
relatively stable. Only 18 percent of our subjects had moved six
years after the base-line examination, and for those who had moved,
correlations between the base-line and follow-up measures of the
neighborhood score were relatively high.
The finding that neighborhood characteristics are related to the
incidence of coronary heart disease suggests that strategies for
disease prevention may need to combine person-centered approaches with
approaches aimed at changing residential environments. More
generally, our findings point to the role of the broader social and
economic forces that generate differences among neighborhoods in
shaping the distribution of health outcomes. At a time of growing
economic segregation of residential areas,44,45
differences among places may become even more relevant to
explanations of disparities in health.
Supported by a grant (R29 HL59386, to Dr. Diez Roux) from the
National Heart, Lung, and Blood Institute. The Atherosclerosis Risk
in Communities Study was supported by contracts (N01-HC-55015, N01-HC-55016,
N01-HC-55018, N01-HC-55019, N01-HC-55020, N01-HC-55021, and
N01-HC-55022) with the National Heart, Lung, and Blood Institute.
We are indebted to the staff and participants in the
Atherosclerosis Risk in Communities Study for their important
contributions and to Dr. David Jacobs for helpful comments.
Source Information
From the Division of General Medicine, Columbia College of Physicians
and Surgeons (A.V.D.R., S.S.M.), and the Division of Epidemiology, Joseph T.
Mailman School of Public Health (A.V.D.R.), Columbia University, New York; the
Division of Epidemiology, School of Public Health, University of Minnesota,
Minneapolis (D.A.); the Department of Biostatistics and Collaborative Studies
Coordinating Center (L.C.) and the Department of Epidemiology (M.M., H.A.T.),
University of North Carolina at Chapel Hill, Chapel Hill; the Department of
Epidemiology, Johns Hopkins University School of Hygiene and Public Health,
Baltimore (F.J.N., M.S.); the Division of Epidemiology and Clinical
Applications, National Heart, Lung, and Blood Institute, Bethesda, Md. (P.S.);
and the Department of Preventive Medicine, University of Mississippi Medical
Center, Jackson (R.L.W.).
Address reprint requests to Dr. Diez Roux at the Division of
General Medicine, Columbia Presbyterian Medical Center, 622 W. 168th St., PH9
E., Rm. 105, New York, NY 10032, or at [log in to unmask].
References
- Kaplan
G. People and places: contrasting perspectives on the association between
social class and health. Int J Health Serv 1996;26:507-519.
[Medline]
- Macintyre
S, Maciver S, Sooman A. Area, class, and health: should we be focusing on
places or people? J Soc Policy 1993;22:213-234.
- Robert
S. Socioeconomic position and health: the independent contribution of
community socioeconomic context. Annu Rev Sociol 1999;25:489-516.
- Haan M,
Kaplan G, Camacho T. Poverty and health: prospective evidence from the
Alameda County Study. Am J Epidemiol 1987;125:989-998.
[Abstract]
- Anderson
RT, Sorlie P, Backlund E, Johnson N, Kaplan GA. Mortality effects of
community socioeconomic status. Epidemiology 1997;8:42-47.
[Medline]
- Robert
S. Community-level socioeconomic status effects on adult health. J Health
Soc Behav 1998;39:18-37.
[Medline]
- Yen IH,
Kaplan G. Neighborhood social environment and risk of death: multilevel
evidence from the Alameda County Study. Am J Epidemiol 1999;149:898-907.
[Abstract]
- Smith
GD, Hart C, Watt G, Hole D, Hawthorne V. Individual social class,
area-based deprivation, cardiovascular disease risk factors, and
mortality: the Renfrew and Paisley Study. J Epidemiol Community Health
1998;52:399-405.
[Abstract]
- Waitzman
NJ, Smith KR. Phantom of the area: poverty-area residence and mortality in
the United States. Am J Public Health 1998;88:973-976. [Erratum, Am J
Public Health 1998;88:1122.]
[Medline]
- Kleinschmidt
I, Hills M, Elliott P. Smoking behaviour can be predicted by neighbourhood
deprivation measures. J Epidemiol Community Health 1995;49:Suppl 2:S72-S77.
[Medline]
- Yen IH,
Kaplan GA. Poverty area residence and changes in physical activity level:
evidence from the Alameda County Study. Am J Public Health 1998;88:1709-1712.
[Medline]
- Duncan
C, Jones K, Moon G. Smoking and deprivation: are there neighbourhood
effects? Soc Sci Med 1999;48:497-505.
[Medline]
- Diez-Roux
AV, Nieto FJ, Muntaner C, et al. Neighborhood environments and coronary
heart disease: a multilevel analysis. Am J Epidemiol 1997;146:48-63.
[Abstract]
- Diez-Roux
AV, Nieto FJ, Caulfield L, Tyroler HA, Watson RL, Szklo M. Neighbourhood
differences in diet: the Atherosclerosis Risk in Communities (ARIC) Study.
J Epidemiol Community Health 1999;53:55-63.
[Abstract]
- Hart C,
Ecob R, Smith GD. People, places, and coronary heart disease risk factors:
a multilevel analysis of the Scottish Heart Health Study archive. Soc Sci
Med 1997;45:893-902.
[Medline]
- The ARIC
Investigators. The Atherosclerosis Risk in Communities (ARIC) Study:
design and objectives. Am J Epidemiol 1989;129:687-702.
[Abstract]
- Geographic
areas reference manual. Washington, D.C.: Bureau of the Census, 1994.
- Bureau
of the Census. 1980 Census of population: classified index of industries
and occupations. Final ed. Washington, D.C.: Government Printing Office,
1982.
- White
AD, Folsom AR, Chambless LE, et al. Community surveillance of coronary
heart disease in the Atherosclerosis Risk in Communities (ARIC) Study:
methods and initial two years' experience. J Clin Epidemiol
1996;49:223-233.
[Medline]
- National
Heart, Lung, and Blood Institute. Atherosclerosis Risk in Communities
(ARIC) Study. Operations manual no. 3. Surveillance components procedures,
version 1.0. Chapel Hill, N.C.: ARIC Coordinating Center, School of Public
Health, University of North Carolina, 1987.
- Rautaharju
PM, Warren JW, Jain U, Wolf HK, Nielsen CL. Cardiac infarction injury
score: an electrocardiographic coding scheme for ischemic heart disease.
Circulation 1981;64:249-256.
[Abstract]
- Baecke
JA, Burema J, Frijters JER. A short questionnaire for the measurement of
habitual physical activity in epidemiological studies. Am J Clin Nutr
1982;36:936-942.
[Abstract]
- Anderson
JT, Jacobs DR Jr, Foster N, et al. Scoring systems for evaluating dietary
pattern effect on serum cholesterol. Prev Med 1979;8:525-527.
[Medline]
- Kahn HA,
Sempos CT. Statistical methods in epidemiology. New York: Oxford
University Press, 1989.
- Szklo M,
Nieto FJ. Epidemiology: beyond the basics. Gaithersburg, Md.: Aspen, 2000.
- Cox DR.
Regression models and life-tables. J R Stat Soc [B] 1972;34: 187-220.
- Shah BV,
Barnwell BG, Bieler GS. SUDAAN user's manual, release 7.5. Research
Triangle Park, N.C.: Research Triangle Institute, 1997.
- Kaplan
GA, Keil JE. Socioeconomic factors and cardiovascular disease: a review of
the literature. Circulation 1993;88:1973-1998.
[Abstract]
- Fabsitz
R, Feinleib M. Geographic patterns in county mortality rates from
cardiovascular disease. Am J Epidemiol 1980;111:315-328.
[Abstract]
- Elford
J, Phillips AN, Thomson AG, Shaper AG. Migration and geographic variations
in ischaemic heart disease in Great Britain. Lancet 1989;1:343-346.
[Medline]
- Wing S,
Dargent-Molina P, Casper M, Riggan W, Hayes CG, Tyroler HA. Changing
association between community occupational structure and ischaemic heart
disease mortality in the United States. Lancet 1987;2:1067-1070.
[Medline]
- Wing S,
Casper M, Riggan W, Hayes C, Tyroler HA. Socioenvironmental
characteristics associated with the onset of decline of ischemic heart
disease mortality in the United States. Am J Public Health 1988;78:923-926.
[Medline]
- Hackbarth
DP, Silvestri B, Cosper W. Tobacco and alcohol billboards in 50 Chicago
neighborhoods: market segmentation to sell dangerous products to the poor.
J Public Health Policy 1995;16:213-230.
[Medline]
- Pucci
LG, Joseph HM Jr, Siegel M. Outdoor tobacco advertising in six Boston
neighborhoods: evaluating youth exposure. Am J Prev Med 1998;15:155-159.
[Medline]
- Mooney
C. Cost and availability of healthy food choices in a London health
district. J Hum Nutr Diet 1990;3:111-120.
- Troutt
D. The thin red line: how the poor still pay more. San Francisco:
Consumers Union of the United States, 1993.
- Green M.
The poor pay more . . . for less. Part 1. Grocery shopping. New York: City
of New York, Department of Consumer Affairs, 1991.
- Cheadle
A, Psaty BM, Curry S, et al. Community-level comparisons between the
grocery store environment and individual dietary practices. Prev Med
1991;20:250-261.
[Medline]
- King AC,
Blair SN, Bild DE, et al. Determinants of physical activity and
interventions in adults. Med Sci Sports Exerc 1992;24:Suppl:S221-S236.
[Medline]
- Neighborhood
safety and the prevalence of physical activity -- selected states, 1996.
MMWR Morb Mortal Wkly Rep 1999;48:143-146.
[Medline]
- Henry
JP. Mechanisms by which stress can lead to coronary heart disease.
Postgrad Med J 1986;62:687-693.
[Abstract]
- Shumaker
SA, Czajkowski SM. Social support and cardiovascular disease. New York:
Plenum Press, 1994.
- Robins
JM, Greenland S. Identifiability and exchangeability for direct and
indirect effects. Epidemiology 1992;3:143-155.
[Medline]
- Jargowsky
PA. Take the money and run: economic segregation in US metropolitan areas.
Am Sociol Rev 1996;61:984-998.
- Massey
DS. The age of extremes: concentrated affluence and poverty in the
twenty-first century. Demography 1996;33:395-412.
[Medline]
Edward E.
Rylander, M.D.
Diplomat American
Board of Family Practice.
Diplomat American
Board of Palliative Medicine.