Evaluation and Management of Chronic Mitral
Regurgitation
Catherine M. Otto, M.D.
This Journal
feature begins with a case vignette highlighting a common clinical
problem. Evidence supporting various strategies is then presented,
followed by a review of formal guidelines, when they exist. The
article ends with the author's clinical recommendations.
A 56-year-old man with no history of
cardiac disease and no cardiac symptoms has a holosystolic murmur at
the apex that radiates to the axilla. Echocardiography shows
moderate mitral regurgitation with mild left ventricular dilatation.
How should this patient's care be managed?
There are about 500,000 discharge diagnoses of mitral-valve disease
annually in the United States.1
However, estimates of the prevalence of mitral regurgitation are
confounded by the presence of benign flow murmurs in many adults and
by the small amount of physiologic regurgitation detected on
echocardiography in 80 percent of adults. Only about 18,000 patients
undergo mitral-valve surgery annually, suggesting that most patients
with a diagnosis of mitral regurgitation never need surgical intervention.
Thus, the challenge for the clinician is first to determine which
patients have pathologic mitral regurgitation and then to provide
them with appropriate care.
The Clinical Problem
Causation
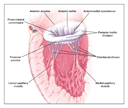
Normal mitral-valve function depends on the complex interactions
of all the components of the valve apparatus (Figure 1). In
surgical series, the most common causes of severe mitral regurgitation
are mitral-valve prolapse (20 to 70 percent of cases), ischemia (13
to 30 percent), rheumatic heart disease (3 to 40 percent), and
endocarditis (10 to 12 percent).2
Although mitral-valve prolapse is common in surgical series, most
patients with mitral-valve prolapse have only mild disease and never
need surgery. Mitral-valve prolapse and ischemic disease are also
common in patients with milder regurgitation, but the most common
causes are ventricular dilatation and systolic dysfunction. In the
elderly, mitral regurgitation may be due to annular calcification;
typically, regurgitation in older persons is mild to moderate and
intervention is rarely necessary. Accurate identification of the
mechanism of mitral regurgitation is essential because the clinical
outcome, the medical therapy prescribed, and the potential need for
surgical intervention depend as much on the cause as on the severity
of disease.
|
Pathophysiological Process
Chronic left ventricular volume overload as a result of mitral
regurgitation leads to compensatory dilatation of the left ventricle.
Although this response initially maintains cardiac output, myocardial
decompensation eventually results in symptoms of heart failure and
an increased risk of sudden death.3 In
some patients, left ventricular contractility is irreversibly
impaired in the absence of symptoms.4 In
addition, backflow into the left atrium results in enlargement of
the left atrium, atrial fibrillation, and elevated pulmonary
pressures.
Diagnosis
Mitral regurgitation may be diagnosed on the basis of the presence
of a systolic murmur in asymptomatic adults or incidentally when
echocardiography is performed for other indications. Some patients
with primary disease of the valve leaflets present with symptoms of
heart failure, atrial fibrillation, or endocarditis. The symptoms
may be precipitated by a superimposed hemodynamic stress, such as
that induced by pregnancy, anemia, or an infection. In patients with
secondary regurgitation, valve dysfunction is most often identified
during an evaluation of the underlying disease process.
On physical examination, the murmur of mitral regurgitation is
classically an apical holosystolic murmur that radiates to the
axilla. However, physical examination is not always reliable in
distinguishing mitral regurgitation from other types of systolic murmurs
and does not provide an accurate measure of the severity of
regurgitation.5
On electrocardiography and chest radiography, evidence of
enlargement of the left atrium, left ventricle, or both is seen only
late in the course of disease and is not sensitive or specific for
the diagnosis of mitral regurgitation.
Echocardiography
Echocardiography allows accurate evaluation of the presence or
absence, severity, and cause of mitral regurgitation. Echocardiography is
indicated in patients who have a systolic murmur and any cardiac
symptoms, a loud murmur (![]() grade 3/6) alone, or other
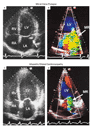
cardiac findings on physical examination. In most cases, the cause
of mitral regurgitation can be deduced from the two-dimensional images
(Figure 2).
Although Doppler echocardiography provides several methods of
quantifying the severity of regurgitation, none have been shown to
predict the clinical outcome. Most centers grade regurgitation as
mild, moderate, or severe using a combination of color flow,
continuous, and pulsed-wave Doppler imaging.6
grade 3/6) alone, or other
cardiac findings on physical examination. In most cases, the cause
of mitral regurgitation can be deduced from the two-dimensional images
(Figure 2).
Although Doppler echocardiography provides several methods of
quantifying the severity of regurgitation, none have been shown to
predict the clinical outcome. Most centers grade regurgitation as
mild, moderate, or severe using a combination of color flow,
continuous, and pulsed-wave Doppler imaging.6
|
The most important aspect of the echocardiographic examination is
the quantitation of left ventricular systolic performance. Although calculation
of the ejection fraction is an imperfect means of assessing
contractility, from a practical point of view, the ejection fraction
in conjunction with the end-systolic dimension provides a clinically
useful measure of ventricular performance. Transesophageal
echocardiography allows accurate assessment of the feasibility of
valve repair and should be performed before surgical intervention.7
Outcome
Patients with mitral regurgitation may remain asymptomatic for
many years; the average interval from diagnosis to the onset of
symptoms is 16 years.8
There are few data on the rate of hemodynamic progression of disease
in patients with mild-to-moderate regurgitation, since most series
are restricted to patients with severe regurgitation. In addition,
the available data are difficult to interpret, since the criteria
for evaluating the severity of regurgitation vary and are not always
clearly defined. Furthermore, even though the clinical outcome is
strongly dependent on the cause of the disease, patients with
diverse mechanisms of regurgitation are often included in the same
study.
In patients with severe symptomatic mitral regurgitation, the
clinical outcome is poor: survival rates are as low as 33 percent at
eight years in the absence of surgical intervention. The average
mortality rate is approximately 5 percent per year; most deaths are
related to heart failure, but there is a substantial incidence of
sudden death, suggesting that ventricular arrhythmias may be an
important feature of the disease process.8,9
Other complications include atrial fibrillation, cerebral ischemic
events, and endocarditis.
In patients with mitral-valve prolapse, the clinical outcome depends
on the extent of leaflet disease and the severity of mitral
regurgitation. The progression of disease may be slow and insidious
or may be abrupt, as a result of a chordal rupture leading to flail
leaflet. In one study of patients with initially asymptomatic severe
mitral regurgitation caused by mitral-valve prolapse, only 28
percent required surgery within five years because of the onset of
symptoms.10
In contrast, 90 percent of patients with a flail mitral-valve
leaflet died or underwent surgery within 10 years, whether or not
they initially had symptoms.11
Mitral regurgitation as a sequela of rheumatic fever is uncommon
in the United States and is typically associated with some degree of
mitral stenosis.12
Ischemic mitral regurgitation encompasses several mechanisms,
including papillary-muscle dysfunction, regional ventricular
dysfunction, and left ventricular dilatation. The outcome is related
to the severity of symptoms at presentation and the extent of
underlying coronary disease.13
In patients with dilated cardiomyopathy, mitral regurgitation has
diverse causes, including annular dilatation, changes in the shape
and size of the left ventricle, and systolic dysfunction.14
Strategies and Evidence
Most patients in whom chronic mitral regurgitation is diagnosed
have mild-to-moderate disease and are unlikely ever to need surgical
intervention. Management is directed toward identifying the cause
and severity of the regurgitation, treating underlying disease
processes, preventing complications, educating the patient, and
evaluating risk factors for coronary disease. In patients with
primary mitral-valve disease, periodic echocardiography allows early
detection of impaired left ventricular systolic function on the
basis of the measurement of the end-systolic dimension and ejection
fraction (Table
1). Other echocardiographic measures that are useful in clinical
decision making include assessment of the size of the left atrium
and pulmonary systolic pressure.
|
Medical Therapy
No known medical therapies directly affect the disease process
in the valve leaflets in patients with mitral-valve prolapse or
rheumatic valve disease. There has been sustained interest in the
concept of using vasodilator therapy to decrease the severity of
mitral regurgitation and the rate of left ventricular dilatation.
The rationale for vasodilator therapy is that a reduction in the
afterload may increase aortic flow and decrease mitral backflow. To
some extent, this rationale has been validated in small, short-term
studies that demonstrated a decrease in systemic vascular resistance
and regurgitant fraction and an increase in cardiac output with
vasodilator therapy, often with a decrease in ventricular volumes
and end-diastolic pressure.15,16
However, these studies show that vasodilators are most effective in
improving symptoms in patients with mitral regurgitation associated
with ventricular dilatation and impaired systolic function.17
There are no data that support the use of vasodilator therapy in
patients with asymptomatic mitral regurgitation and normal
ventricular function.18
Most important, the use of medical therapy should not delay
consideration of surgical intervention in patients with symptoms or
evidence of left ventricular systolic dysfunction.
Medical therapy is primarily directed toward the treatment of
the complications of mitral regurgitation and the prevention of
endocarditis with antibiotic prophylaxis. If atrial fibrillation occurs,
standard approaches to rate control, cardioversion, and
anticoagulation are indicated.18
In patients with mitral regurgitation as a result of ischemic
disease, prevention of ischemia with medical therapy, percutaneous
transluminal coronary intervention, or bypass grafting is
appropriate. In patients with mitral regurgitation due to dilated
cardiomyopathy, medical therapy for heart failure, including
afterload reduction, often results in improvement in left
ventricular shape, size, and systolic function in association with a
reduction in the severity of regurgitation.
Mitral-Valve Surgery
The optimal surgical intervention for mitral regurgitation is
valve repair. As compared with valve replacement, successful valve
repair results in superior hemodynamics and ventricular function,
avoidance of a prosthetic valve and the need for long-term anticoagulation,
and less distortion of ventricular shape. The feasibility of valve
repair is highest in patients with mitral-valve prolapse, especially
in those whose disease is confined to the posterior leaflet. As
surgical techniques improve, an increasing number of patients are
becoming candidates for this procedure. When valve repair is not
technically possible, every effort is made to maintain the integrity
of the mitral chordal apparatus. With chordal preservation, there is
little change in the ejection fraction after surgery, as compared
with an average decline of 10 ejection-fraction units in patients
with transected chords. The operative mortality rate is lower for
mitral-valve repair than for valve replacement (2 to 4 percent vs. 5
to 10 percent). In patients with mitral-valve prolapse, long-term
clinical outcome is excellent, with survival rates of 80 to 94
percent at 5 to 10 years with valve repair as compared with 40 to 60
percent with valve replacement.19,20
In patients with symptoms due to mitral regurgitation, surgical
intervention is indicated, unless they have severe left ventricular dysfunction.
In asymptomatic patients with severe mitral regurgitation, the
outcome is improved if surgery is performed before the onset of
irreversible ventricular dysfunction. No randomized trials have
assessed the optimal timing of intervention for asymptomatic severe
mitral regurgitation, and the ideal measure of ventricular contractility
remains elusive. However, a consensus has been reached that left
ventricular end-systolic dimension and ejection fraction can be used
to identify early systolic dysfunction. The evidence supporting this
approach is derived from studies in patients who were undergoing
valve surgery for severe mitral regurgitation that assessed the
value of preoperative variables as predictors of postoperative
ventricular performance.4,21,22,23
Indicators of early systolic dysfunction are an end-systolic dimension
of 45 mm or more or an ejection fraction of 0.60 or less. Systolic
dysfunction is most likely when both values are abnormal and
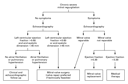
sequential studies show a progressive deterioration. Other factors
that may affect the timing of surgical intervention include the
feasibility of valve repair, the onset of atrial fibrillation, and
the development of progressive pulmonary hypertension (Figure 3).
There are two noteworthy features of these criteria: the degree of
ventricular dilatation seen with isolated volume overload due to
mitral regurgitation is much less than that seen in aortic
regurgitation, a condition characterized by combined pressure and
volume overload, and these criteria only apply to patients with
severe mitral regurgitation.
|
Areas of Uncertainty
Assessment of the Severity of Mitral
Regurgitation
The current definition of severe mitral regurgitation is based
on angiographic and echocardiographic descriptors of the degree of
backflow across the valve. An alternative physiological definition would
be mitral regurgitation severe enough to result in dilatation of the
left ventricle, left atrium, or both. However, the best definition
would be regurgitation leading to adverse clinical outcomes.
Unfortunately, prospective data based on quantitative measures of
severity are not available. Thus, it is not certain whether some
patients with moderate regurgitation have severe disease that has
not yet resulted in ventricular enlargement. The percentage of
patients with mild regurgitation who will have a progressive
increase in the severity of mitral regurgitation is also unknown.
Medical Therapy for Primary Valve Disease
In patients with severe mitral regurgitation due to primary valve
disease, there are no persuasive data that medical therapy decreases
the rate of ventricular dilatation or delays valve surgery. Some
clinicians argue that medical therapy may even be harmful if it
increases the severity of regurgitation in patients with mitral-valve
prolapse, prevents normal adaptive responses of the left ventricle,
or delays the recognition of early symptoms or ventricular
dysfunction.
Timing of Surgical Intervention
When severe mitral regurgitation and severely reduced ventricular
function are both present, it can be difficult to determine whether
ventricular dysfunction is the cause or a consequence of chronic
regurgitation. In either case, the surgical outcome is poor when the
ejection fraction is less than 0.30, unless chordal continuity is
preserved. In some patients, a trial of medical therapy for heart
failure and an evaluation for other causes of left ventricular
dysfunction may clarify the situation. Because the optimal approach
to these patients is controversial, clinical decision making must be
individualized on the basis of the evaluation of ventricular and
valvular function, the likelihood of valve repair, the presence of
other underlying conditions, and the patient's preferences.
Valve Repair in Patients with Secondary
Mitral Regurgitation
Some studies of patients with ischemic mitral regurgitation suggest
that revascularization alone decreases the severity of
regurgitation, whereas other studies suggest that concurrent valve
repair or the placement of an annuloplasty ring is necessary.24
Revascularization might be effective if regurgitation is due to
ischemia or if revascularization improves the shape of the mitral
valve. However, if there is irreversible myocardial damage or if
remodeling does not occur, then mitral regurgitation may persist. In
the absence of randomized clinical trials, the surgical decision is
currently individualized on the basis of the mechanism of
regurgitation in each patient.
In patients with dilated cardiomyopathy, mitral regurgitation
is due to the change in the shape of the valvular apparatus, so
that the severity of regurgitation is often decreased by medical
therapy that restores the ventricular size and shape. Some centers
advocate mitral-valve surgery in these patients, but this approach
is not widely accepted.25
Guidelines
The American College of Cardiology and the American Heart
Association have developed detailed guidelines for the evaluation,
follow-up, and optimal timing of surgical intervention in patients
with severe mitral regurgitation.18
Appropriate candidates for mitral-valve surgery include patients
with symptoms, except those with severe ventricular dysfunction, and
patients with no symptoms who have mild or moderate ventricular
dysfunction. Surgery is indicated in asymptomatic patients with
preserved ventricular function if there is a high likelihood of
valve repair or if there is evidence of pulmonary hypertension or
recent atrial fibrillation. Guidelines also address the use of
echocardiography, the prevention of rheumatic fever and
endocarditis, and indications for anticoagulation.
Conclusions and Recommendations
In the case of patients with a cardiac murmur, the threshold for
echocardiographic evaluation should be low. When the valve is
anatomically abnormal, periodic clinical and echocardiographic follow-up
allows early identification of symptoms, complications, and systolic
dysfunction. In patients with secondary mitral regurgitation,
echocardiography serves as the first step toward the evaluation and
treatment of the underlying disease process. Patient education is
vital, both to ensure compliance with follow-up and to allow the
patient to participate in the decision-making process.
In the case of the patient described in the vignette, annual echocardiography
and evaluation by a cardiologist are appropriate to monitor the
severity of mitral regurgitation, the size of the left ventricle,
and pulmonary-artery pressure. Surgical intervention in patients
with severe mitral regurgitation is indicated at the onset of
symptoms or in the presence of convincing evidence of left
ventricular systolic dysfunction. Valve repair rather than valve
replacement should be performed whenever possible. We should remain
cautious in recommending valve surgery for asymptomatic patients who
are considered to have severe mitral regurgitation but who have no
evidence of consequences of hemodynamic abnormalities. However, the
excellent anatomical and clinical outcomes of valve repair make
surgical intervention appropriate earlier in the course of disease
in many patients with severe mitral regurgitation as a means of
preventing chronic volume overload.
Source Information
From the Division of Cardiology, University of Washington,
Seattle.
References
- National
Center for Health Statistics, Owings MF, Lawrence L. Detailed diagnosis
and procedures: National Hospital Discharge Survey, 1997. Vital and health
statistics. Series 13. No. 145. Washington, D.C.: Government Printing
Office, December 1999. (DHHS publication no. (PHS) 2000-1716.)
- Olson
LJ, Subramanian R, Ackermann DM, Orszulak TA, Edwards WD. Surgical
pathology of the mitral valve: a study of 712 cases spanning 21 years.
Mayo Clin Proc 1987;62:22-34.
[Medline]
- Carabello
BA. The pathophysiology of mitral regurgitation. J Heart Valve Dis
2000;9:600-608.
[Medline]
- Corin
WJ, Sutsch G, Murakami T, Krogmann ON, Turina M, Hess OM. Left ventricular
function in chronic mitral regurgitation: preoperative and postoperative
comparison. J Am Coll Cardiol 1995;25:113-121.
[Medline]
- Desjardins
VA, Enriquez-Sarano M, Tajik AJ, Bailey KR, Seward JB. Intensity of
murmurs correlates with severity of valvular regurgitation. Am J Med
1996;100:149-156.
[Medline]
- Otto CM.
Valvular regurgitation: diagnosis, quantitation and clinical approach. In:
Otto CM, ed. Textbook of clinical echocardiography. Philadelphia: W.B.
Saunders, 2000:265-300.
- Enriquez-Sarano
M, Freeman WK, Tribouilloy CM, et al. Functional anatomy of mitral
regurgitation: accuracy and outcome implications of transesophageal
echocardiography. J Am Coll Cardiol 1999;34:1129-1136.
[Medline]
- Delahaye
JP, Gare JP, Viguier E, Delahaye F, De Gevigney G, Milon H. Natural
history of severe mitral regurgitation. Eur Heart J 1991;12:Suppl B:5-9.
- Grigioni
F, Enriquez-Sarano M, Ling LH, et al. Sudden death in mitral regurgitation
due to flail leaflet. J Am Coll Cardiol 1999;34:2078-2085.
[Medline]
- Rosen
SE, Borer JS, Hochreiter C, et al. Natural history of the
asymptomatic/minimally symptomatic patient with severe mitral
regurgitation secondary to mitral valve prolapse and normal right and left
ventricular performance. Am J Cardiol 1994;74:374-380.
[Medline]
- Ling LH,
Enriquez-Sarano M, Seward JB, et al. Clinical outcome of mitral
regurgitation due to flail leaflet. N Engl J Med 1996;335:1417-1423.
[Abstract/Full Text]
- Marcus
RH, Sareli P, Pocock WA, Barlow JB. The spectrum of severe rheumatic
mitral valve disease in a developing country: correlations among clinical
presentation, surgical pathologic findings, and hemodynamic sequelae. Ann
Intern Med 1994;120:177-183.
[Medline]
- Rankin
JS, Hickey MS, Smith LR, et al. Ischemic mitral regurgitation. Circulation
1989;79:116-121.
[Abstract]
- Kono T,
Sabbah HN, Rosman H, Alam M, Jafri S, Goldstein S. Left ventricular shape
is the primary determinant of functional mitral regurgitation in heart
failure. J Am Coll Cardiol 1992;20:1594-1598.
[Medline]
- Tischler
MD, Rowan M, LeWinter MM. Effect of enalapril therapy on left ventricular
mass and volumes in asymptomatic chronic, severe mitral regurgitation
secondary to mitral valve prolapse. Am J Cardiol 1998;82:242-245.
[Medline]
- Rothlisberger
C, Sareli P, Wisenbaugh T. Comparison of single dose nifedipine and
captopril for chronic severe mitral regurgitation. Am J Cardiol
1994;73:978-981.
[Medline]
- Levine
HJ, Gaasch WH. Vasoactive drugs in chronic regurgitant lesions of the
mitral and aortic valves. J Am Coll Cardiol 1996;28:1083-1091.
[Medline]
- ACC/AHA
guidelines for the management of patients with valvular heart disease: a
report of the American College of Cardiology/American Heart Association
Task Force on Practice Guidelines (Committee on Management of Patients
with Valvular Heart Disease). J Am Coll Cardiol 1998;32:1486-1588.
[Medline]
- David
TE, Armstrong S, Sun Z, Daniel L. Late results of mitral valve repair for
mitral regurgitation due to degenerative disease. Ann Thorac Surg
1993;56:7-12.
[Abstract]
- Akins
CW, Hilgenberg AD, Buckley MJ, et al. Mitral valve reconstruction versus
replacement for degenerative or ischemic mitral regurgitation. Ann Thorac
Surg 1994;58:668-675.
[Abstract]
- Enriquez-Sarano
M, Tajik AJ, Schaff HV, et al. Echocardiographic prediction of left ventricular
function after correction of mitral regurgitation: results and clinical
implications. J Am Coll Cardiol 1994;24:1536-1543.
[Medline]
- Crawford
MH, Souchek J, Oprian CA, et al. Determinants of survival and left
ventricular performance after mitral valve replacement: Department of
Veterans Affairs Cooperative Study on Valvular Heart Disease. Circulation
1990;81:1173-1181.
[Abstract]
- Flemming
MA, Oral H, Rothman ED, Briesmiester K, Petrusha JA, Starling MR.
Echocardiographic markers for mitral valve surgery to preserve left
ventricular performance in mitral regurgitation. Am Heart J
2000;140:476-482.
[Medline]
- Galloway
AC, Grossi EA, Spencer FC, Colvin SB. Operative therapy for mitral
insufficiency from coronary artery disease. Semin Thorac Cardiovasc Surg
1995;7:227-232.
[Medline]
- Bach DS,
Bolling SF. Improvement following correction of secondary mitral
regurgitation in end-stage cardiomyopathy with mitral annuloplasty. Am J
Cardiol 1996;78:966-969.
[Medline]
Edward E.
Rylander, M.D.
Diplomat American
Board of Family Practice.
Diplomat American
Board of Palliative Medicine.