|
|
|||||
|
|
Coronary Magnetic Resonance Angiography for the
Detection of Coronary Stenoses
W. Yong Kim, M.D., Ph.D., Peter G. Danias, M.D., Ph.D., Matthias
Stuber, Ph.D., Scott D. Flamm, M.D., Sven Plein, M.D., Eike Nagel, M.D., Susan
E. Langerak, M.Sc., Oliver M. Weber, Ph.D., Erik M. Pedersen, M.D., Ph.D.,
Matthias Schmidt, M.D., René M. Botnar, Ph.D., and Warren J. Manning, M.D.
ABSTRACT
Background An accurate,
noninvasive technique for the diagnosis of coronary disease would be
an important advance. We investigated the accuracy of coronary
magnetic resonance angiography among patients with suspected
coronary disease in a prospective, multicenter study.
Methods Coronary
magnetic resonance angiography was performed during free breathing
in 109 patients before elective x-ray coronary angiography, and the
results of the two diagnostic procedures were compared.
Results A total of
636 of 759 proximal and middle segments of coronary arteries (84
percent) were interpretable on magnetic resonance angiography. In
these segments, 78 (83 percent) of 94 clinically significant lesions
(those with a ![]() 50 percent reduction in
diameter on x-ray angiography) were also detected by magnetic resonance
angiography. Overall, coronary magnetic resonance angiography had an
accuracy of 72 percent (95 percent confidence interval, 63 to 81
percent) in diagnosing coronary artery disease. The sensitivity,
specificity, and accuracy for patients with disease of the left main
coronary artery or three-vessel disease were 100 percent (95 percent
confidence interval, 97 to 100 percent), 85 percent (95 percent confidence
interval, 78 to 92 percent), and 87 percent (95 percent confidence
interval, 81 to 93 percent), respectively. The negative predictive
values for any coronary artery disease and for left main artery or
three-vessel disease were 81 percent (95 percent confidence interval,
73 to 89 percent) and 100 percent (95 percent confidence interval,
97 to 100 percent), respectively.
50 percent reduction in
diameter on x-ray angiography) were also detected by magnetic resonance
angiography. Overall, coronary magnetic resonance angiography had an
accuracy of 72 percent (95 percent confidence interval, 63 to 81
percent) in diagnosing coronary artery disease. The sensitivity,
specificity, and accuracy for patients with disease of the left main
coronary artery or three-vessel disease were 100 percent (95 percent
confidence interval, 97 to 100 percent), 85 percent (95 percent confidence
interval, 78 to 92 percent), and 87 percent (95 percent confidence
interval, 81 to 93 percent), respectively. The negative predictive
values for any coronary artery disease and for left main artery or
three-vessel disease were 81 percent (95 percent confidence interval,
73 to 89 percent) and 100 percent (95 percent confidence interval,
97 to 100 percent), respectively.
Conclusions Among
patients referred for their first x-ray coronary angiogram,
three-dimensional coronary magnetic resonance angiography allows for
the accurate detection of coronary artery disease of the proximal
and middle segments. This noninvasive approach reliably identifies
(or rules out) left main coronary artery or three-vessel disease.
Despite progress in prevention and early
diagnosis, coronary artery disease remains the leading cause of
death in both men and women in the United States1 and
throughout the Western world. Invasive x-ray coronary angiography
remains the gold standard for the identification of clinically
significant coronary artery disease. Although numerous noninvasive
tests have been developed to assist in the identification of
patients with coronary artery disease, a substantial minority of
patients referred for elective diagnostic x-ray coronary angiography
are found not to have clinically significant coronary stenosis
(defined as a reduction in the luminal diameter of at least 50
percent).2
A noninvasive test that could directly assess the integrity of the
coronary lumen would therefore be desirable.
Coronary magnetic resonance angiography makes possible the
noninvasive visualization of the major epicardial coronary arteries
in the majority of subjects. Since the first reports by Paulin et
al.3
and Edelman et al.,4 coronary
magnetic resonance angiography has undergone technological advances
leading to enhanced spatial resolution and the possibility of
imaging while the patient is breathing freely, but assessment of its
usefulness has been hampered by the lack of standardized hardware,
software, and scanning protocols. The results from single-center
studies therefore vary considerably.5,6,7,8,9,10,11,12,13,14
Coronary magnetic resonance angiography15,16
performed while the patient is breathing freely has reached
sufficient technical maturity to allow more widespread application
with a standardized protocol. Therefore, we conducted a prospective,
international, multicenter study to determine the clinical
usefulness of coronary magnetic resonance angiography in the
diagnosis of native-vessel coronary artery disease.
Methods
Participating Institutions
The subjects were recruited from seven institutions: Skejby Hospital,
Aarhus University Hospital, Aarhus, Denmark (7 subjects), the German
Heart Institute, Berlin, Germany (18 subjects), Beth Israel
Deaconess Medical Center, Boston (18 subjects), St. Luke's Episcopal
Hospital, Houston (25 subjects), Leeds General Infirmary, Leeds,
United Kingdom (23 subjects), Leiden University Medical Center,
Leiden, the Netherlands (9 subjects), and the University and
Eidgenoessische Technische Hochschule Zurich, Zurich, Switzerland (9
subjects). The review board at each institution approved the study,
and written informed consent was obtained from all subjects. In all
cases, coronary magnetic resonance angiography was performed before
x-ray angiography.
Patients
The study population consisted of 109 subjects who were
consecutively enrolled between June 24, 1999, and October 18, 2000.
The subjects could be of either sex and had to be at least 21 years
of age with sinus rhythm and with a body weight of 100 kg or less
and to be scheduled to undergo elective x-ray coronary angiography
for suspected coronary artery disease within 14 days. The exclusion criteria
were a contraindication to magnetic resonance imaging17
(for example, a pacemaker, intraauricular implants, or intracranial clips),
previous x-ray coronary angiography or thoracotomy, claustrophobia,
orthopnea, and inability to take sublingual nitroglycerin (as a
result, for example, of aortic stenosis or obstructive
cardiomyopathy).
Protocol for Magnetic Resonance
Angiography
Each center performed coronary magnetic resonance angiography
according to a standard protocol16
with use of common hardware and software on a 1.5-T system (Gyroscan
ACS-NT, Philips Medical Systems, Best, the Netherlands) equipped
with PowerTrak 6000 gradients (23 mT per meter, 219 µsec rise time).
The subjects were examined with a commercial five-element cardiac
synergy receiver coil during uncoached free breathing. To compensate
for artifacts due to respiratory motion, a right hemidiaphragmatic navigator18
with real-time slice correction19
and a 5-mm end-expiratory gating window were used. For cardiac
synchronization and monitoring, three or four20
electrodes were placed on the left anterior hemithorax of the
subject with the R wave of the electrocardiogram used as a trigger
for image acquisition. All coronary images were acquired in
mid-diastole.19
Magnetic Resonance Localization Scans
The first magnetic resonance localizing scan (approximately one
minute) employed a multistack and multislice, segmented k-space
gradient–echo sequence for localization of the heart and diaphragm
in three orthogonal planes (transverse, sagittal, and coronal).15,16
From the coronal data set, a navigator-gated transverse
three-dimensional segmented echo localizing planar scan
(approximately two minutes) with 40 slices was acquired around the
base of the heart to cover the region extending from the apex of the
left ventricle to the pulmonary artery.16
This allowed identification of the course of the major right and
left coronary arteries. With the use of a three-point planscan tool,16 a
plane through the major axis of the proximal and middle segments of
the right coronary artery was subsequently prescribed.
Three-Dimensional Magnetic Resonance
Angiography
Coronary magnetic resonance angiography was performed, after sublingual
administration of isosorbide dinitrate (2.5 mg), with the use of a
three-dimensional segmented k-space gradient–echo sequence (echo
time, 2.2 msec; repetition time, 7.7 msec) during free breathing
(for about 10 to 15 minutes).15,16
For contrast enhancement between blood and the surrounding
myocardium and epicardial fat, a T2-weighted preparation
prepulse and a frequency-selective fat-saturation prepulse were
applied.15
For the right coronary artery, a double-oblique three-dimensional
volume was imaged with use of the coordinates prescribed by the
three-point planscan tool. For the left main, left anterior
descending, and left circumflex coronary arteries, a double-oblique
transverse three-dimensional volume with anterior–posterior and
left–right angulations (5 degrees each) was imaged with the volume
centered on the origin of the left main coronary artery (as defined
from the second localizing scan). For both the left and the right
coronary systems, the three-dimensional volumes were reconstructed
to 20 slices, with an individual slice thickness of 1.5 mm. A field
of view of 360 mm and a 512-by-360 matrix yielded an in-plane voxel
size of 0.7 by 1.0 mm. No signal averaging was performed.
Analysis of Coronary Magnetic Resonance
Angiograms
Source coronary magnetic resonance angiograms were evaluated at
each site (before x-ray angiography) and again by consensus of two
experienced investigators (from the core magnetic resonance imaging
laboratory at the Beth Israel Deaconess Medical Center) who were
blinded to the patients' clinical data and the x-ray data. The
original source images were analyzed by scrolling through individual
slices from the three-dimensional data set with the use of a
commercial software package (EasyVision 4.0, Philips Medical
Systems, Best, the Netherlands). Seven coronary segments were
evaluated: the left main coronary artery and the proximal and middle
segments of the left anterior descending coronary artery (0 to 2 cm
and 2 to 4 cm), the left circumflex coronary artery (0 to 1.5 cm and
1.5 to 3 cm), and the right coronary artery (0 to 2 cm and 2 to 5
cm). For each segment, image quality was visually graded21
as 1, indicating poor or uninterpretable (coronary artery visible,
with markedly blurred borders or edges); 2, good (coronary artery
visible, with moderately blurred borders or edges); 3, very good
(coronary artery visible, with mildly blurred borders or edges); or
4, excellent (coronary artery visible, with sharply defined borders
or edges). If the segments were not imaged or if the image quality
was graded as poor or uninterpretable (grade 1), no further
evaluation was performed. Segments that were not visualized or that
were graded as poor or uninterpretable were not included in the
subsequent analysis. Images of good, very good, and excellent
quality (grades 2, 3, and 4) were further classified according to
the visual assessment of the coronary-artery lumen as having no
coronary artery disease, minimal disease, or clinically significant
disease (if there was prominent attenuation of the coronary-lumen
signal).
Acquisition and Analysis of Coronary X-Ray
Angiograms
Conventional x-ray coronary angiography was performed by standard
techniques22
and in multiple projections after sublingual administration of
isosorbide dinitrate (2.5 mg). An experienced invasive cardiologist at
the institution where angiography was performed analyzed each x-ray
angiogram without knowledge of the magnetic resonance data. Each
coronary vessel was assessed, and the visual estimation of the
segment and the maximal percentage reduction of the luminal diameter
for each lesion were reported. In addition, in 99 patients (91
percent), quantitative x-ray angiographic analysis was performed by
an independent core laboratory (Brigham and Women's Hospital Angiographic
Core Laboratory, Boston) without access to the magnetic resonance
data. Quantitative angiographic analysis was performed according to
a standard algorithm,23
with clinically significant disease defined as stenosis of at least
50 percent of the vessel diameter. For 10 subjects for whom
quantitative analysis was not performed because of administrative
issues (e.g., images could not be located or were unreadable), the
visual evaluation reported from the site was used for the analyses.
Statistical Analysis
The data were retained at the Beth Israel Deaconess Medical Center,
and the primary data analysis was performed by one of us. For each
individual vessel and for each patient, the sensitivity, specificity,
and accuracy (percentage of segments correctly classified) were
determined, as well as the positive and negative predictive values
for coronary magnetic resonance angiography as compared with x-ray
coronary angiography. All data are reported as means ±SD or rates
with 95 percent confidence intervals.
Results
All subjects completed coronary magnetic resonance angiography
without complications. Of the 109 subjects, 69 percent were men
(Table 1).
The majority of the subjects had a history of chest pain, smoking,
and hypercholesterolemia. Sixty-four of the subjects (59 percent)
had x-ray angiographic evidence of coronary artery disease,
including 12 percent with three-vessel disease (Table 1).
|
The mean total magnetic resonance scanning time (including scout imaging)
was 70 minutes (median, 66; range, 33 to 145). The median interval
between the performance of coronary magnetic resonance angiography
and x-ray angiography was 1 day (mean, 3; range, 0 to 14), with no
clinical cardiac events reported between the examinations. Right
coronary x-ray angiography was not performed in two subjects. Thus,
759 coronary segments were potentially available for analysis. Of
these, 636 (84 percent) could be assessed by coronary magnetic
resonance angiography; the proportions of segments for which images
could be assessed ranged from 68 percent (for the middle left
circumflex coronary artery) to 93 percent (for the proximal and
middle right coronary artery) (Table 2).
Coronary segments were not interpretable by magnetic resonance
angiography when scans were not obtained because of time constraints
(39 segments), when image quality was poor (grade 1, 58 segments),
or when the three-dimensional volume did not include the segment (26
segments).
|
In the magnetic resonance angiographic assessment of diagnostic accuracy
for each individual vessel, we included all vessels for which the
proximal segment was graded as having an image quality of at least 2
(good or better). In the analyses for any coronary artery disease
and for left main coronary artery or three-vessel disease, 103
subjects (94 percent) were eligible according to the consensus
readings, and 101 (93 percent) were eligible according to the
readings at the sites. Patients were considered eligible if
clinically significant coronary artery disease identified on x-ray
angiography was found in any coronary artery segment with a readable
magnetic resonance image.
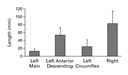
The overall image quality was 2.6±0.7 (Table 2).
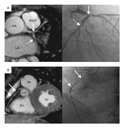
Individual segment lengths are shown in Figure 1. An
example of a coronary magnetic resonance angiogram and a
corresponding x-ray contrast angiogram for a patient with left and
right coronary artery disease are shown in Figure 2.
|
|
Seventy-eight of 94 clinically significant coronary stenoses (83
percent) identified on x-ray angiography were correctly identified
on magnetic resonance angiography. The sensitivity of coronary
magnetic resonance angiography for identifying a patient as having
clinically significant coronary artery disease, according to the consensus
of the two interpreters, was 93 percent (95 percent confidence
interval, 88 to 98 percent) (Table 3). All
four patients who had clinically significant coronary artery disease
that was not diagnosed by coronary magnetic resonance angiography
had isolated single-vessel disease, with two (50 percent) having
isolated left circumflex artery disease. In the consensus
interpretation, the overall diagnostic accuracy of coronary magnetic
resonance angiography in identifying a patient as having any
coronary artery disease was 72 percent (95 percent confidence
interval, 63 to 81 percent), increasing to 87 percent (95 percent
confidence interval, 81 to 93 percent) for the identification of a
patient with left main coronary artery or three-vessel disease. The
prevalence, sensitivity, specificity, and positive and negative
predictive values for individual coronary vessels and patients
according to the consensus and the site-reported interpretations are
summarized in Table
3.
|
Discussion
In this prospective, multicenter study comparing noncontrast coronary
magnetic resonance angiography with x-ray angiography among patients
referred for a first elective coronary angiogram, we found that
coronary magnetic resonance angiography had a high sensitivity,
negative predictive value, and overall accuracy for detecting
coronary artery disease, especially in subjects with left main
coronary artery disease or three-vessel disease. Coronary magnetic
resonance angiography is not exercise-dependent, and its high
negative predictive value suggests that it may have a role in ruling
out clinically significant coronary disease in this population of
patients, among whom the prevalence of disease is intermediate.
Indeed, 41 percent of study subjects had no clinically significant
coronary artery disease, a prevalence similar to that in previously
published data,2
a fact that emphasizes the need for an accurate, noninvasive
technique that can rule out clinically significant disease before
invasive x-ray coronary angiography. On the basis of the finding of
no clinically significant disease on magnetic resonance angiography,
x-ray angiography could have been avoided in 18 subjects (according
to the consensus reading) or 25 subjects (according to the site
reading) — those with true negative results (Table 3), or 42
to 58 percent of subjects without clinically significant coronary
artery disease. With the use of standardized technology and a
standardized scanning protocol, all patients with left main coronary
artery or three-vessel disease were identified as having clinically
significant coronary artery disease. These data therefore support
the use of coronary magnetic resonance angiography to identify (or
rule out) left main coronary artery disease or three-vessel disease
reliably. Such information is clinically relevant, since surgical
revascularization in patients with such disease is associated with a
more favorable long-term survival benefit.24
The protocol for three-dimensional, noncontrast, free-breathing
coronary magnetic resonance angiography facilitated visualization of
the vast majority of the proximal and middle segments of the left
main, left anterior descending, and right coronary arteries.
Coronary magnetic resonance angiography would detect 94 percent of
all patients with any coronary artery disease or with left main
coronary artery or three-vessel disease. The left circumflex artery
was less reliably visualized, but isolated disease of this artery
was found in only 4 percent of subjects, suggesting that the absence
of clinically significant disease in the remaining coronary system
makes left circumflex artery disease unlikely. This observation is
in agreement with other reports.25
The accuracy of coronary magnetic resonance angiography for the
detection of coronary disease in the left circumflex artery was also
low in prior single-center studies.5,6,9,13
This poor accuracy may be due to the relatively small caliber and
posterior location of the circumflex artery, which results in a
lower signal-to-noise ratio because of the increased distance from
the artery to the receiver coils.
Other minimally invasive imaging methods have recently been advocated
for coronary-artery imaging. Electron-beam computed tomography is a
highly sensitive technique for detecting calcium in the coronary
arteries.2
Recent studies using multislice computed tomography in combination
with iodinated contrast medium to visualize the coronary-artery
lumen demonstrated very good diagnostic accuracy for detecting
coronary artery disease when image quality was adequate (that is,
when 70 to 80 percent of images could be assessed).26,27,28 A
potential advantage of this method is the acquisition of a complete
data set during a single, though prolonged, breath-holding period
(30 to 40 seconds). As compared with computed tomography, the
magnetic resonance approach has the advantage of requiring no
exposure to ionizing radiation or injection of a contrast agent, and
it allows for more comfortable free breathing during the entire examination.
Both the magnetic resonance29
and computed tomographic approaches are safe in patients with
intracoronary stents, but interpretation is difficult.
Coronary magnetic resonance angiography has already been
demonstrated to be of clinical value for the assessment of anomalous
coronary artery disease, and it is often superior to x-ray coronary
angiography in delineating the course of the anomalous vessels.30,31,32,33
However, coronary magnetic resonance angiography was considered an
investigational technique for the assessment of stenotic native-vessel
disease in task-force reports from Europe and the United States in
1998.34,35
The results of single-center investigations of coronary magnetic
resonance angiography that used different hardware, software, and
scanning protocols have been variable.5,6,7,8,9,10,11,12,13,14
Single-center experience (often including patients who had
previously undergone angiography or a coronary intervention) may
also be difficult to translate into general clinical practice. Clinical
acceptance of coronary magnetic resonance angiography will probably
require standardization to ensure optimal test results. The findings
of the present multicenter study should reflect the clinical value
of coronary magnetic resonance angiography more accurately, because
we evaluated a relatively large number of patients at seven
international institutions and used common hardware and software and
a common scanning protocol. Only one of the seven participating
institutions had extensive experience with coronary magnetic
resonance angiography. Furthermore, the independent consensus
analyses and those reported from individual sites were quite similar
(Table 3).
Subgroups of patients who may initially benefit from coronary
magnetic resonance angiography are likely to include patients who
present with severe left ventricular systolic dysfunction in the
absence of a clinical history of myocardial infarction. For these
patients, the underlying disease process is either severe
multivessel coronary artery disease or nonischemic cardiomyopathy. Conventional
stress tests are often inaccurate in this group, resulting in
frequent referral for diagnostic coronary angiography. Although this
possibility was not directly tested in our study, the data suggest
that coronary magnetic resonance angiography may be able to
discriminate between these two causes; thus, x-ray angiography could
be avoided for those without magnetic resonance evidence of coronary
disease. It should be remembered, however, that coronary magnetic
resonance angiography was unable to assess 16 percent of coronary
segments and that 6 percent of the study patients could not be
assessed for the presence of any coronary disease or for left main
coronary artery or three-vessel disease.
Supported in part by Philips Medical Systems, Best, the
Netherlands, which funded the quantitative coronary angiographic
analysis (but not the selection of the analysis laboratory or data
interpretation) and by an Established Investigatorship Grant from
the American Heart Association, Dallas (9740003N, to Dr. Manning).
Source Information
From the Cardiovascular Division, Department of Medicine (W.Y.K.,
P.G.D., M. Stuber, R.M.B., W.J.M.), and the Department of Radiology (W.J.M.),
Beth Israel Deaconess Medical Center and Harvard Medical School, Boston; the
Magnetic Resonance Center, Department of Cardiology, and Institute of
Experimental Clinical Research, Skejby Hospital, Aarhus University Hospital,
Aarhus, Denmark (W.Y.K., E.M.P.); Philips Medical Systems, Best, the
Netherlands (M. Stuber, R.M.B.); St. Luke's Episcopal Hospital and the Texas
Heart Institute, Houston (S.D.F.); the Yorkshire Heart Centre, Leeds General
Infirmary, Leeds, United Kingdom (S.P.); Internal Medicine Cardiology, German
Heart Institute, Berlin, Germany (E.N.); the Department of Radiology and
Cardiology, Leiden University Medical Center, Leiden, the Netherlands (S.E.L.);
the Institute for Biomedical Engineering, University of Zurich, and the Swiss
Federal Institute of Technology Zurich, Zurich, Switzerland (O.M.W.); and the
Klinik und Poliklinik für Nuklearmedizin der Universität zu Köln, Cologne,
Germany (M. Schmidt).
Address reprint requests to Dr. Manning at the Beth Israel
Deaconess Medical Center, 330 Brookline Ave., Boston, MA 02215, or at [log in to unmask].
References
- 2001
Heart and stroke statistical update. Dallas: American Heart Association,
2000.
- Budoff
MJ, Georgiou D, Brody A, et al. Ultrafast computed tomography as a
diagnostic modality in the detection of coronary artery disease: a
multicenter study. Circulation 1996;93:898-904.
[Abstract/Full Text]
- Paulin
S, von Schulthess GK, Fossel E, Krayenbuehl HP. MR imaging of the aortic
root and proximal coronary arteries. AJR Am J Roentgenol 1987;148:665-670.
[Medline]
- Edelman
RR, Manning WJ, Burstein D, Paulin S. Coronary arteries: breath-hold MR
angiography. Radiology 1991;181:641-643.
[Abstract]
- Manning
WJ, Li W, Edelman RR. A preliminary report comparing magnetic resonance
coronary angiography with conventional angiography. N Engl J Med
1993;328:828-832. [Erratum, N Engl J Med 1993;330:152.]
[Abstract/Full Text]
- Duerinckx
AJ, Urman MK. Two-dimensional coronary MR angiography: analysis of initial
clinical results. Radiology 1994;193:731-738.
[Abstract]
- Pennell
DJ, Bogren HG, Keegan J, Firmin DN, Underwood SR. Assessment of coronary
artery stenosis by magnetic resonance imaging. Heart 1996;75:127-133.
[Abstract]
- Oshinski
JN, Hofland L, Mukundan S Jr, Dixon WT, Parks WJ, Pettigrew RI.
Two-dimensional coronary MR angiography without breath holding. Radiology
1996;201:737-743.
[Abstract]
- Post JC,
van Rossum AC, Hofman MB, de Cock CC, Valk J, Visser CA. Clinical utility
of two-dimensional magnetic resonance angiography in detecting coronary
artery disease. Eur Heart J 1997;18:426-433.
[Medline]
- Müller
MF, Fleisch M, Kroeker R, Chatterjee T, Meier B, Vock P. Proximal coronary
artery stenosis: three-dimensional MRI with fat saturation and navigator
echo. J Magn Reson Imaging 1997;7:644-651.
[Medline]
- Woodard
PK, Li D, Haacke EM, et al. Detection of coronary stenoses on source and
projection images using three-dimensional MR angiography with retrospective
respiratory gating: preliminary experience. AJR Am J Roentgenol
1998;170:883-888.
[Abstract]
- van
Geuns RJ, Wielopolski PA, de Bruin HG, et al. MR coronary angiography with
breath-hold targeted volumes: preliminary clinical results. Radiology
2000;217:270-277.
[Abstract/Full Text]
- Regenfus
M, Ropers D, Achenbach S, et al. Noninvasive detection of coronary artery
stenosis using contrast-enhanced three-dimensional breath-hold magnetic
resonance coronary angiography. J Am Coll Cardiol 2000;36:44-50.
[Medline]
- Moustapha
AI, Pereyra M, Muthupillai R, Wilson JM, Flamm SD. Coronary magnetic
resonance angiography using a free-breathing T2 weighted,
three-dimensional gradient echo sequence with navigator respiratory and
ECG gating can be used to detect coronary artery disease. J Am Coll
Cardiol 2001;37:Suppl A:380A-380A.abstract
- Botnar
RM, Stuber M, Danias PG, Kissinger KV, Manning WJ. Improved coronary
artery definition with T2-weighted, free-breathing three-dimensional coronary
MRA. Circulation 1999;99:3139-3148.
[Abstract/Full Text]
- Stuber
M, Botnar RM, Danias PG, et al. Double-oblique free-breathing high
resolution three-dimensional coronary magnetic resonance angiography. J Am
Coll Cardiol 1999;34:524-531.
[Medline]
- Sawyer-Glover
AM, Shellock FG. Pre-MRI procedure screening: recommendations and safety
considerations for biomedical implants and devices. J Magn Reson Imaging
2000;12:92-106. [Erratum, J Magn Reson Imaging 2000;12:510.]
[Medline]
- Ehman
RL, Felmlee JP. Adaptive technique for high-definition MR imaging of
moving structures. Radiology 1989;173:255-263.
[Abstract]
- Stuber
M, Botnar RM, Danias PG, Kissinger KV, Manning WJ. Submillimeter
three-dimensional coronary MR angiography with real-time navigator
correction: comparison of navigator locations. Radiology 1999;212:579-587.
[Abstract/Full Text]
- Fischer
SE, Wickline SA, Lorenz CH. Novel real-time R-wave detection algorithm
based on the vectorcardiogram for accurate gated magnetic resonance
acquisitions. Magn Reson Med 1999;42:361-370.
[Medline]
- McConnell
MV, Khasgiwala VC, Savord BJ, et al. Comparison of respiratory suppression
methods and navigator locations for MR coronary angiography. AJR Am J
Roentgenol 1997;168:1369-1375.
[Abstract]
- Baim DS,
Grossman W, eds. Cardiac catheterization, angiography, and intervention.
5th ed. Philadelphia: Williams & Wilkins, 1996.
- van der
Zwet PM, Reiber JH. A new approach for the quantification of complex
lesion morphology: the gradient field transform: basic principles and
validation results. J Am Coll Cardiol 1994;24:216-224.
[Medline]
- Eagle
KA, Guyton RA, Davidoff R, et al. ACC/AHA guidelines for coronary artery
bypass graft surgery: executive summary and recommendations: a report of
the American College of Cardiology/American Heart Association Task Force
on Practice Guidelines (Committee to Revise the 1991 Guidelines for
Coronary Artery Bypass Graft Surgery). Circulation 1999;100:1464-1480.
[Full Text]
- Hillis
LD, Winniford MD. Frequency of severe (70% or more) narrowing of the
right, left anterior descending, and left circumflex coronary arteries in
right dominant circulations with coronary artery disease. Am J Cardiol
1987;59:358-359.
[Medline]
- Rensing
BJ, Bongaerts A, van Geuns RJ, van Ooijen P, Oudkerk M, de Feyter PJ.
Intravenous coronary angiography by electron beam computed tomography: a
clinical evaluation. Circulation 1998;98:2509-2512.
[Abstract/Full Text]
- Achenbach
S, Moshage W, Ropers D, Nossen J, Daniel WG. Value of electron-beam
computed tomography for the noninvasive detection of high-grade
coronary-artery stenoses and occlusions. N Engl J Med 1998;339:1964-1971.
[Abstract/Full Text]
- Nieman
K, Oudkerk M, Rensing BJ, et al. Coronary angiography with multi-slice
computed tomography. Lancet 2001;357:599-603.
[Medline]
- Hug J,
Nagel E, Bornstedt A, Schnackenburg B, Oswald H, Fleck E. Coronary
arterial stents: safety and artifacts during MR imaging. Radiology
2000;216:781-787.
[Abstract/Full Text]
- McConnell
MV, Ganz P, Selwyn AP, Li W, Edelman RR, Manning WJ. Identification of
anomalous coronary arteries and their anatomic course by magnetic
resonance coronary angiography. Circulation 1995;92:3158-3162.
[Abstract/Full Text]
- Post JC,
van Rossum AC, Bronzwaer JG, et al. Magnetic resonance angiography of
anomalous coronary arteries: a new gold standard for delineating the
proximal course? Circulation 1995;92:3163-3171.
[Abstract/Full Text]
- Taylor
AM, Thorne SA, Rubens MB, et al. Coronary artery imaging in grown up
congenital heart disease: complementary role of magnetic resonance and
x-ray coronary angiography. Circulation 2000;101:1670-1678.
[Abstract/Full Text]
- Razmi
RM, Meduri A, Chun W, Rathi VK, Pohost GM. Coronary magnetic resonance
angiography (CMRA): the gold standard for determining the proximal course
of anomalous coronary arteries. J Am Coll Cardiol 2001;37:Suppl
A:380A-380A.abstract
- Budinger
TF, Berson A, McVeigh ER, et al. Cardiac MR imaging: report of a working
group sponsored by the National Heart, Lung, and Blood Institute.
Radiology 1998;208:573-576.
[Medline]
- Task
Force of the European Society of Cardiology, Association of European
Paediatric Cardiologists. The clinical role of magnetic resonance in
cardiovascular disease. Eur Heart J 1998;19:19-39.
[Medline]
Appendix
The following investigators also participated in this study: A.D.
Blankholm, Skejby Hospital, Aarhus University Hospital, Aarhus,
Denmark; C. Klein, E. Fleck, J. Hug, and A. Bornstedt, German Heart
Institute, Berlin, Germany; K.V. Kissinger and L.A. Goepfert, Beth
Israel Deaconess Medical Center, Boston; A. Moustapha, M. Pereyra,
B. Lambert, J.M. Wilson, and R. Muthupillai, St. Luke's Episcopal
Hospital, Houston; M.U. Sivananthan, J.P Ridgway, T.R. Jones, and
T.N. Bloomer, Leeds General Infirmary, Leeds, United Kingdom; A. de
Roos, P. Kunz, H. Lamb, J.W. Jukema, and E.E. van der Wall, Leiden
University Medical Center, Leiden, the Netherlands; and J.
Schwitter, University Hospital, Zurich, Switzerland.
|
|
Edward E.
Rylander, M.D.
Diplomat American
Board of Family Practice.
Diplomat American
Board of Palliative Medicine.