|
|
Chronic Urticaria and Angioedema
Allen P. Kaplan, M.D.
|
|
This Journal feature
begins with a case vignette highlighting a common clinical problem.
Evidence supporting various strategies is then presented, followed
by a review of formal guidelines, when they exist. The article ends
with the author's clinical recommendations.
A 35-year-old woman presents with a
three-month history of daily generalized hives. The hives are
pruritic, red wheals that range from 1.5 to 8.0 cm (0.5 to 3 in.) in
diameter. She has frequent episodes of lip swelling and has also had
three episodes of tongue swelling, one of which was associated with
tightness of the throat. How should she be evaluated and treated?
The Clinical Problem
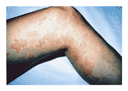
The case vignette describes a typical patient with chronic
urticaria (Figure 1) and
angioedema. The disorder is diagnosed when hives occur on a regular
basis for more than six weeks. This interval is sufficient to rule
out most identifiable causes of acute urticaria, such as drug
reactions and food or contact allergies. Angioedema accompanies
urticaria in approximately 40 percent of patients and, when present,
typically affects the lips, face (particularly the periorbital area),
hands, feet, penis, or scrotum. Occasionally there may be swelling
of the tongue or pharynx, but the larynx is virtually never
involved. Another 40 percent of patients have hives alone, and about
20 percent of patients have angioedema but not urticaria.
|
Strategies and Evidence
Diagnosis
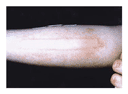
The most common alternative diagnosis is hives due to
dermatographism (Figure 2); in
severe cases, patients will have hives every day for months or
years. They are commonly linear, but they can be any shape. In
dermatographism, individual hives last 30 minutes to 2 hours, as
they do in most other types of physically induced hives (e.g., cold
urticaria, cholinergic urticaria, and solar urticaria). In contrast,
the hives associated with chronic urticaria last 4 to 36 hours.1
Patients with chronic urticaria may also have mild dermatographism,
but the hives associated with primary dermatographism are much more
severe.
|
The patient's history and findings on physical examination may suggest
an underlying cause of urticaria. Occasionally, chronic urticaria
and angioedema are manifestations of an underlying connective-tissue
disorder or a systemic vasculitis in which the findings on
histologic examination of the underlying skin may be consistent with
a leukocytoclastic angiitis rather than the nonnecrotizing
vasculopathy typical of chronic urticaria. However, cutaneous
vasculitis accounts for less than 1 percent of all cases of chronic
hives.
Hashimoto's disease is the only systemic disorder with a clear
and common association with chronic urticaria and angioedema.2,3
Less common is an association with Graves' disease. The percentage of
patients with chronic urticaria who have antithyroglobulin antibody,
antimicrosomal antibody, or both is 27 percent, and 19 percent have
abnormal thyroid function.3
There is no evidence to suggest that these antithyroid antibodies
are pathogenic; the thyroid abnormality appears to be a parallel
abnormality and may reflect the presence of an underlying autoimmune
process.
Chronic urticaria appears to be an autoimmune disorder in a substantial
fraction of patients. Approximately 35 to 40 percent of patients
have a circulating IgG antibody directed against the ![]() subunit of the IgE receptor.4,5,6 An
additional 5 to 10 percent have antibodies against the
subunit of the IgE receptor.4,5,6 An
additional 5 to 10 percent have antibodies against the ![]() subunit of IgE.7
These antibodies activate basophils and mast cells to release
histamine, and complement fixation augments histamine release by
formation of C5a anaphylatoxin.8 The
lesion is characterized by a perivascular infiltration of
lymphocytes that are predominantly CD4-positive, an increased number
of monocytes, and variable numbers of neutrophils and eosinophils,9,10
similar to the findings in a late-phase allergic reaction.
subunit of IgE.7
These antibodies activate basophils and mast cells to release
histamine, and complement fixation augments histamine release by
formation of C5a anaphylatoxin.8 The
lesion is characterized by a perivascular infiltration of
lymphocytes that are predominantly CD4-positive, an increased number
of monocytes, and variable numbers of neutrophils and eosinophils,9,10
similar to the findings in a late-phase allergic reaction.
Chronic urticaria was once considered to be a manifestation of
an anxiety disorder or an allergic or idiosyncratic reaction to
foods, food additives, or food dyes. There are no good data to
support these suppositions. Adherence to a diet of rice, lamb, and
water for five days has no effect on chronic urticaria or
angioedema.1
Data to support or refute an infectious cause of chronic urticaria,
such as Helicobacter pylori, are
still being debated, but an infectious cause is unlikely.11
An autoimmune mechanism appears to be most likely, at least in a
subpopulation of patients, but 60 percent of cases remain
idiopathic.
Evaluation
There are few, if any, diagnostic tests for chronic urticaria
and angioedema. The results of a complete blood count and urinalysis
are typically normal, as are the values for blood chemical variables
usually included in laboratory panels. If a connective-tissue disorder
is suspected, measurement of the erythrocyte sedimentation rate,
tests for antinuclear antibodies, and other serologic tests may be
indicated, followed by a skin biopsy. Complement determinations are
not indicated for patients who have hives alone (since the values
are normal), nor need they be done when angioedema accompanies
chronic urticaria, since patients with a hereditary or acquired
deficiency of C1 inhibitor do not have hives. Only in patients who
present with angioedema alone is measurement of C4 indicated,
followed by a determination of the levels and function of C1
inhibitor, if C4 levels are below normal. Thyroid-function tests,
including tests for antithyroglobulin and antimicrosomal antibodies,
may be helpful, given the association of chronic urticaria with
thyroid disease, with an annual reassessment of function in
euthyroid patients who have elevated antibody titers. Allergies (to
food or food additives) are so rarely a cause of chronic urticaria
that routine testing is not recommended unless particular clues are
present. A skin biopsy may be helpful in patients who have fever,
arthralgias, a prominently elevated sedimentation rate, lesions
lasting 36 hours or more, or associated petechiae or purpura.
Therapy
Histamine
H1–Receptor Antagonists
Nonsedating antihistamines such as loratadine,12
fexofenadine,13,14
and cetirizine15,16,17,18
alleviate pruritus and decrease the incidence of hives in patients with
mild chronic urticaria. Unfortunately, patients with more severe
cases may not benefit from the usual recommended doses of these
agents. A study of 439 patients revealed that fexofenadine, at a
dose of 60, 120, or 240 mg per day, was significantly more
efficacious than placebo, as assessed by the mean pruritus score,
the mean number of wheals per day, the mean daily symptom score (the
sum of the wheal and pruritus scores), and the degree of
interference with sleep, activities of daily living, or both.14
Increasing the dose from 120 to 240 mg per day increased the
efficacy only slightly13
and larger doses did not yield proportionate increases in efficacy.
A 10-mg dose of cetirizine, one of the active ingredients of hydroxyzine,
is approximately equivalent to a 30-mg dose of hydroxyzine but is
far less sedating.17
In a placebo-controlled study of cetirizine and hydroxyzine, 180
patients were assessed with respect to the severity of pruritus, the
number of lesions, the average size and duration of lesions, and the
number of episodes of hives.18
Both agents produced similar improvements in every measured
variable.18
Only four patients given hydroxyzine and one patient given
cetirizine withdrew from the study because of sedation. A potent new
nonsedating antihistamine, mizolastine, which is available in Europe
but not in the United States, appears to be efficacious for chronic
urticaria.
High doses of antihistamines have effects beyond the blockade
of histamine receptors, and actions that are not due to the antagonism
of H1 receptors19
may account for the efficacy of older antihistamines. In one study
of 19 patients, treatment with a combination of H1-receptor
antagonists20
(25 mg of hydroxyzine plus 4 mg of cyproheptadine, each given four
times a day) led to an improvement in symptoms and inhibited the
formation of histamine-induced wheals. When hydroxyzine (100 mg per
day) was compared with terfenadine (the precursor of fexofenadine,
now off the market), hydroxyzine was more effective.21
Combined
H1- and H2-Receptor Antagonists
Approximately 85 percent of histamine receptors in the skin are
of the H1 subtype, and the remaining 15 percent are H2
receptors. The addition of an H2-receptor antagonist to
an H1-receptor antagonist augments the inhibition of a
histamine-induced wheal-and-flare reaction once H1-receptor
blockade has been maximized. On the basis of this rationale, H2-receptor
antagonists have been combined with H1-receptor
antagonists in the treatment of chronic urticaria, with additional
benefit,20
although the increment is small. Doxepin, a tricyclic
antidepressant, blocks both types of histamine receptors and is a
much more potent inhibitor of H1 receptors than either
diphenhydramine or hydroxyzine; however, sedation is an even greater
problem and may limit the usefulness of this drug.22
Leukotriene
Antagonists
Leukotriene antagonists (zafirlukast and montelukast) have been
shown to be superior to placebo in the treatment of patients with
chronic urticaria,23,24
indicating that leukotrienes may also contribute to hives and
swelling. There are no data to support the hypothesis that these
agents have an additional effect once maximal H1- and H2-receptor
blockade has been achieved.
Sympathomimetic
Agents
Oral sympathomimetic agents such as terbutaline have been tried
in patients with chronic urticaria and angioedema in an attempt to
decrease erythema and swelling. However, since the side effects are
substantial and include difficulty sleeping, a jittery feeling, and
tachycardia — and since the efficacy of these agents is low — they
are not generally recommended.
Corticosteroids
There are many patients with chronic urticaria and angioedema
who have little response to even a combination of H1-receptor
blockers, H2-receptor blockers, and leukotriene-receptor
blockade and in whom disability due to the disease warrants
consideration of corticosteroid therapy. Although controlled studies
of the long-term use of corticosteroids have not been conducted,
there is truly no question regarding their efficacy.1
However, the incidence of side effects is substantial if the dose,
the duration of use, or both are too great; in addition, their use
may trigger diabetes or hypertension in patients at increased risk
for these diseases.
Experimental
Therapies
The best studied immunosuppressive therapy for chronic urticaria
is cyclosporine, although studies have been uncontrolled and have
involved only a small number of patients. A low dose (2.5 to 3 mg
per kilogram of body weight per day) appeared to be effective and
corticosteroid sparing,25
whereas a larger dose (6 mg per kilogram) was quite effective but
was associated with severe side effects that precluded its continued
use.26
A single case report indicated that sulfasalazine was effective
for chronic urticaria, and case reports have suggested that hydroxychloroquine
or dapsone might also be effective, but blinded studies involving a
large number of patients have not been conducted. Plasmapheresis has
been advocated for the subgroup of patients with demonstrable
antibodies against the IgE receptor,27
but this approach is impractical for long-term treatment.
Intravenous immune globulin was effective in one small study,28
but this report has not been confirmed. Treatment with levothyroxine
has been proposed in patients with antithyroid antibodies, even if
the patient is euthyroid.29 Such
treatment, however, carries a risk of inducing hyperthyroidism, and
its efficacy has not been proved.3
Areas of Uncertainty
We need to document whether high doses of antihistamines,
particularly the nonsedating types, are superior to lower doses.
Leukotriene-receptor antagonists need to be evaluated in combination
with antihistamine regimens, rather than in placebo-controlled
trials. Long-term studies of corticosteroids are needed to clarify
the dose range that yields the maximal benefit with the fewest side
effects, and to compare the effect of these agents when they are
used alone and when they are added to other regimens. Further
studies of experimental agents such as cyclosporine or perhaps
tacrolimus are needed to assess their safety and efficacy as
corticosteroid-sparing agents.
Guidelines
A "practice parameter" for the diagnosis and management
of acute and chronic urticaria was published in 200030;
it emphasizes the conditions that need to be considered in the
differential diagnosis, such as urticarial vasculitis,
connective-tissue disorders, systemic mastocytosis, and idiopathic
anaphylaxis.
Summary and Recommendations
In a patient with chronic urticaria who has no signs or symptoms
suggestive of an underlying condition, laboratory testing is not
indicated, other than measurement of serum thyrotropin levels and
antithyroid antibodies to rule out associated thyroid disease. These
are the only tests I would recommend for the patient described in
the vignette. Although there is no single right way to manage chronic
urticaria and angioedema, there is general agreement that
nonsedating antihistamines are the first choice for treatment. When
severe urticaria, severe angioedema, or both are present, I believe
that the older antihistamines are more effective than the newer
ones, when maximal doses of these agents are given (e.g., 100 to 200
mg of hydroxyzine or diphenhydramine per day) (Table 1). For
patients with severe angioedema (involving swelling of the face,
tongue, and pharynx), diphenhydramine is particularly effective.
|
Although patients become accustomed to the sedating effects of these
drugs after about a week, their performance on various tests, such
as driving, after a single 50-mg capsule of diphenhydramine31
reflects a decreased reaction time and decreased steadiness; these
effects are similar to the effects produced by alcohol. Yet the
effect of long-term treatment with hydroxyzine or diphenhydramine at
a dosage of 50 mg four times a day has not been assessed. H2-receptor
antagonists have very few side effects and may be useful as
adjunctive therapy. Leukotriene antagonists are also considered safe
and are worth trying. The goal is to maximize function (e.g., the
patient's ability to work or attend school) and minimize the use of
systemic corticosteroids.
There is an important role for alternate-day corticosteroid use
in patients with severe disease. One approach has been outlined in a
number of textbooks,1
although it has not been evaluated in clinical trials. Prednisone is
started at a dose of 15 to 20 mg every other day, and the dose is
gradually tapered to 2.5 to 5.0 mg every three weeks, depending on
the patient's response, and discontinued after four to five months.
Side effects are minimized with the use of dietary discretion and
exercise. Chronic urticaria improves with time, and the condition of
many patients can then be controlled without corticosteroids.
The patient described in the vignette may require not only the
maximal dosage of an H1-receptor antagonist (e.g., 50 mg of
hydroxyzine four times a day), plus an H2-receptor antagonist
and a leukotriene antagonist, but also alternate-day corticosteroids
if a satisfactory response is not achieved. Occasional episodes of
severe facial or pharyngeal swelling can be treated with one or two
doses of a corticosteroid, such as 40 to 60 mg of prednisone (Table 1).
Patients who require alternate-day corticosteroids for more than
six months should be examined annually by an ophthalmologist (for
cataracts and glaucoma) and should undergo bone-density testing
annually. In my practice, daily corticosteroids are never used, and
the dose of alternate-day corticosteroids rarely exceeds 20 mg (Table 1). Some
patients have no responses to any of these approaches, or have a
response only to prohibitively high doses of corticosteroids. Of the
experimental options, 200 to 300 mg of cyclosporine per day appears
to be the best, as long as renal function is closely monitored.
Source Information
From the Department of Medicine, Division of Pulmonary and
Critical Care Medicine and Allergy and Clinical Immunology, and Konishi–Medical
University of South Carolina Institute for Inflammation Research, Medical
University of South Carolina, Charleston.
Address reprint requests to Dr. Kaplan at Medical University of
South Carolina, Division of Pulmonary and Critical Care Medicine, Allergy and
Clinical Immunology, 96 Johnathan Lucas St., Suite 812 CSD, P.O. Box 250623,
Charleston, SC 29425, or at [log in to unmask].
References
- Kaplan
AP. Urticaria and angioedema. In: Middleton E Jr, Reed CE, Ellis EF,
Adkinson NF Jr, Yunginger JW, Busse WW, eds. Allergy: principles &
practice. 5th ed. Vol. 2. St. Louis: Mosby–Year Book, 1998:1104-22.
- Leznoff
A, Sussman GL. Syndrome of idiopathic chronic urticaria and angioedema
with thyroid autoimmunity: a study of 90 patients. J Allergy Clin Immunol
1989;84:66-71.
[Medline]
- Kaplan
AP, Finn A. Autoimmunity and the etiology of chronic urticaria. Can J
Allergy Clin Immunol 1999;4:286-92.
- Hide M,
Francis DM, Grattan CEH, Hakimi J, Kochan JP, Greaves MW. Autoantibodies
against the high-affinity IgE receptor as a cause of histamine release in
chronic urticaria. N Engl J Med 1993;328:1599-1604.
[Abstract/Full Text]
- Fiebiger
E, Maurer D, Holub H, et al. Serum IgG autoantibodies directed against the
 chain of Fc
chain of Fc RI: a selective
marker and pathogenetic factor for a distinct subset of chronic urticaria
patients? J Clin Invest 1995;96:2606-2612.
RI: a selective
marker and pathogenetic factor for a distinct subset of chronic urticaria
patients? J Clin Invest 1995;96:2606-2612.[Medline]
- Ferrer
M, Kinet JP, Kaplan AP. Comparative studies of functional and binding
assays for IgG anti-Fc
 RI
RI (
( -subunit) in
chronic urticaria. J Allergy Clin Immunol 1998;101:672-676. [Erratum, J
Allergy Clin Immunol 1998;102:156.]
-subunit) in
chronic urticaria. J Allergy Clin Immunol 1998;101:672-676. [Erratum, J
Allergy Clin Immunol 1998;102:156.][Medline]
- Gruber
BL, Baeza M, Marchese M, Agnello V, Kaplan AP. Prevalence and functional
role of anti-IgE autoantibodies in urticarial syndromes. J Invest Dermatol
1988;90:213-217.
[Abstract]
- Kikuchi
Y, Kaplan AP. A role for C5a in augmenting IgG-dependent histamine release
from basophils in chronic urticaria. J Allergy Clin Immunol (in press).
- Elias J,
Boss E, Kaplan AP. Studies of the cellular infiltrate of chronic
idiopathic urticaria: prominence of T-lymphocytes, monocytes, and mast
cells. J Allergy Clin Immunol 1986;78:914-918.
[Medline]
- Sabroe
RA, Poon E, Orchard GE, et al. Cutaneous inflammatory cell infiltrate in
chronic idiopathic urticaria: comparison of patients with and without
anti-Fc
 RI or anti-IgE
autoantibodies. J Allergy Clin Immunol 1999;103:484-493.
RI or anti-IgE
autoantibodies. J Allergy Clin Immunol 1999;103:484-493.[Medline]
- Greaves
MW. Chronic idiopathic urticaria (CIU) and Helicobacter pylori — not
directly causative but could there be a link? Allergy Clin Immunol Int
2001;13:23-7.
- Monroe
EW. Loratadine in the treatment of urticaria. Clin Ther 1997;19:232-242.
[Medline]
- Finn AF
Jr, Kaplan AP, Fretwell R, Qu R, Long J. A double-blind,
placebo-controlled trial of fexofenadine HCl in the treatment of chronic
idiopathic urticaria. J Allergy Clin Immunol 1999;103:1071-1078.
- Nelson
HS, Reynolds R, Mason J. Fexofenadine HCl is safe and effective for
treatment of chronic idiopathic urticaria. Ann Allergy Asthma Immunol
2000;84:517-522.
[Medline]
- Andri L,
Senna GE, Betteli C, et al. A comparison of the efficacy of cetirizine and
terfenadine: a double-blind, controlled study of chronic idiopathic
urticaria. Allergy 1993;48:358-365.
[Medline]
- Breneman
D, Bronsky EA, Bruce S, et al. Cetirizine and astemizole therapy for
chronic idiopathic urticaria: a double-blind, placebo-controlled,
comparative trial. J Am Acad Dermatol 1995;33:192-198.
[Medline]
- Kalivas
J, Breneman D, Tharp M, Bruce S, Bigby M. Urticaria: clinical efficacy of
cetirizine in comparison with hydroxyzine and placebo. J Allergy Clin
Immunol 1990;86:1014-1018.
[Medline]
- Breneman
DL. Cetirizine versus hydroxyzine and placebo in chronic idiopathic
urticaria. Ann Pharmacother 1996;30:1075-1079.
[Medline]
- Lichtenstein
LM, Gillespie E. The effects of H1 and H2
antihistamine on "allergic" histamine release and its inhibition
by histamine. J Pharmacol Exp Ther 1975;192:441-450.
[Abstract]
- Harvey
RP, Wegs J, Schocket AL. A controlled trial of therapy in chronic
urticaria. J Allergy Clin Immunol 1981;68:262-266.
[Medline]
- Brunet
C, Bedard P-M, Hebert J. Effects of H1-antihistamine drug
regimen on histamine release by nonlesional skin mast cells of patients
with chronic urticaria. J Allergy Clin Immunol 1990;86:787-793.
[Medline]
- Goldsobel
AB, Rohr AS, Siegel SC, et al. Efficacy of doxepin in the treatment of
chronic idiopathic urticaria. J Allergy Clin Immunol 1986;78:867-873.
[Medline]
- Ellis
MH. Successful treatment of chronic urticaria with leukotriene
antagonists. J Allergy Clin Immunol 1998;102:876-877.
[Medline]
- Spector
S, Tan RA. Antileukotrienes in chronic urticaria. J Allergy Clin Immunol
1998;101:572-572.
[Medline]
- Toubi E,
Blant A, Kessel A, Golan TD. Low-dose cyclosporin A in the treatment of
severe chronic idiopathic urticaria. Allergy 1997;52:312-316.
[Medline]
- Fradin
MS, Ellis CN, Goldfarb MT, Voorhees JJ. Oral cyclosporine for severe
chronic idiopathic urticaria and angioedema. J Am Acad Dermatol
1991;25:1065-1067.
[Medline]
- Grattan
CEH, Francis DM, Slater NGP, Barlow RJ, Greaves MW. Plasmapheresis for
severe, unremitting, chronic urticaria. Lancet 1992;339:1078-1080.
[Medline]
- O'Donnell
BF, Barr RM, Black AK, et al. Intravenous immunoglobulin in autoimmune
chronic urticaria. Br J Dermatol 1998;138:101-106.
[Medline]
- Gaig P,
Garcia-Ortega P, Enrique E, Richart C. Successful treatment of chronic
idiopathic urticaria associated with thyroid autoimmunity. J Investig
Allergy Clin Immunol 2000;10:342-5.
- Wanderer
AA, Bernstein IL, Goodman DL, et al. , eds. The diagnosis and management
of urticaria: a practice parameter. Ann Allergy Asthma Immunol
2000;85:521-544.
[Medline]
- Weiler
JM, Bloomfield JR, Woodworth GG, et al. Effects of fexofenadine,
diphenhydramine, and alcohol on driving performance: a randomized,
placebo-controlled trial in the Iowa Driving Simulator. Ann Intern Med
2000;132:354-363.
[Medline]
Edward E.
Rylander, M.D.
Diplomat American
Board of Family Practice.
Diplomat American
Board of Palliative Medicine.